What is Phlebitis?
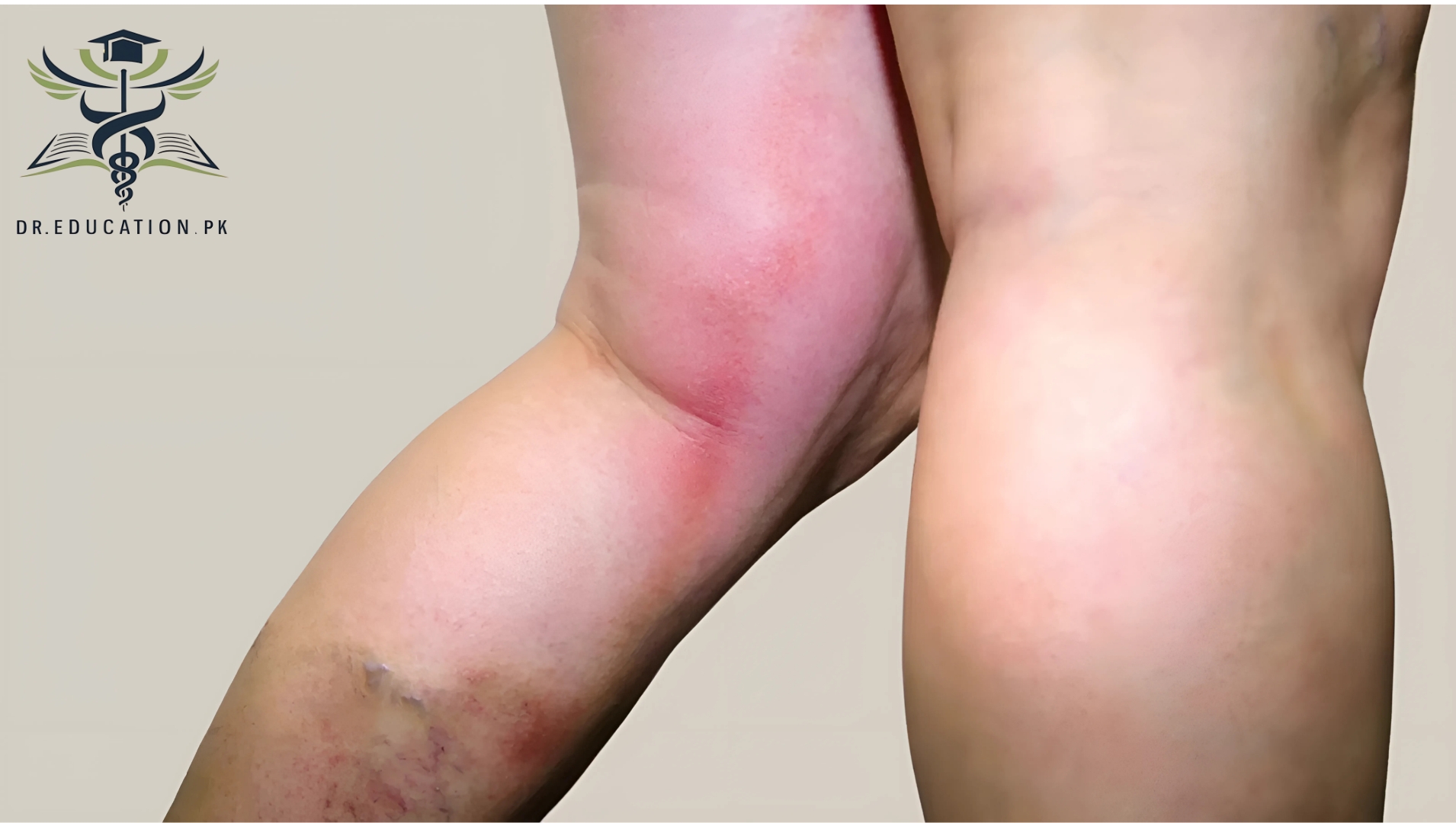
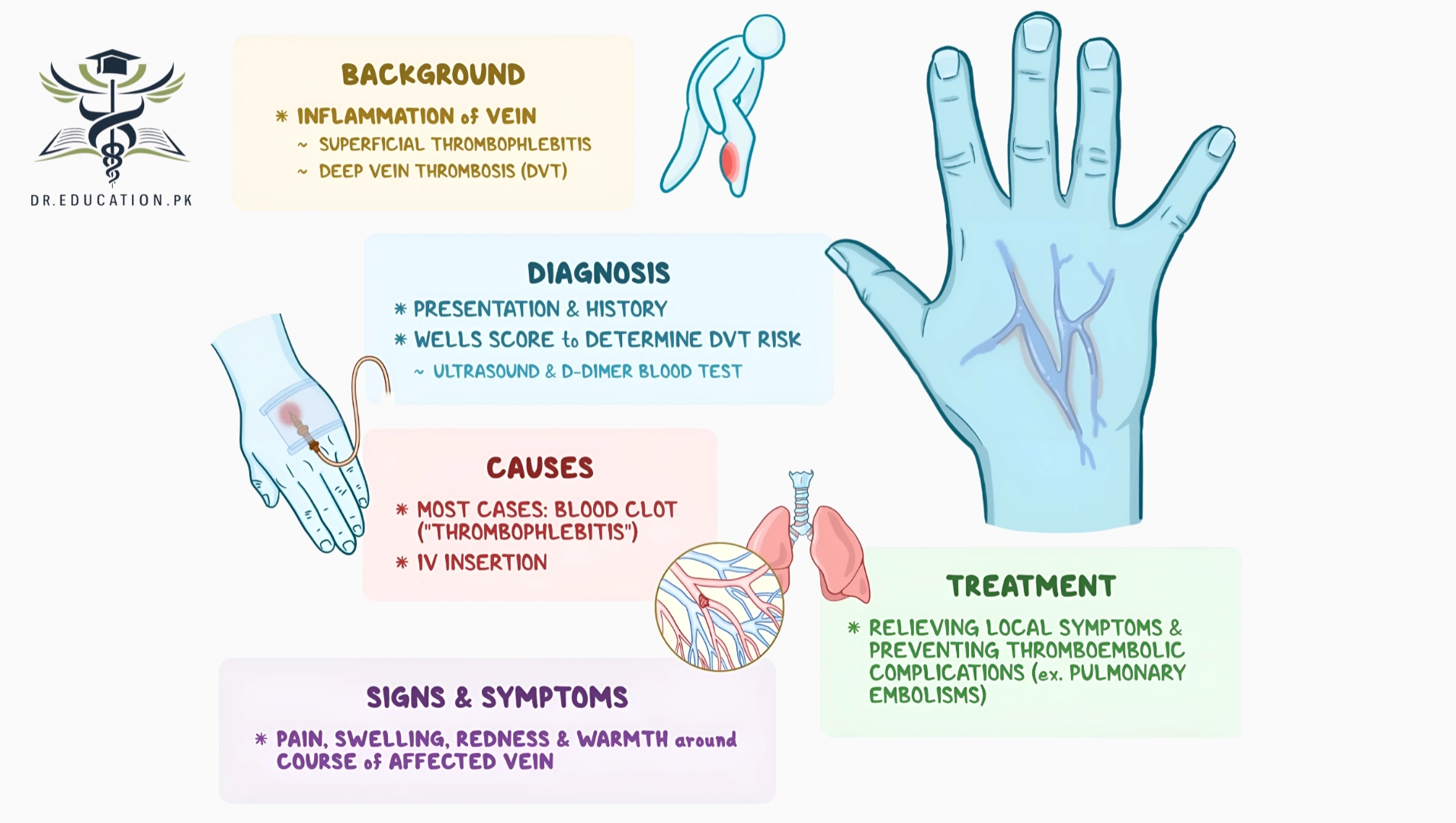
Phlebitis is the inflammation of a vein, typically occurring in the legs. It can result from various factors, such as injury, infection, or irritation, and is often associated with blood clots. When a blood clot causes the inflammation, the condition is referred to as thrombophlebitis. Symptoms of phlebitis may include redness, swelling, warmth, and pain in the affected area. Phlebitis can be superficial, affecting veins near the skin’s surface, or deep, involving deeper veins, which may pose a greater risk of complications like deep vein thrombosis (DVT).
Overview
How to pronounce Phlebitis?
Phlebitis is Pronounced as (fle-BYE-tis).
What is Phlebitis?
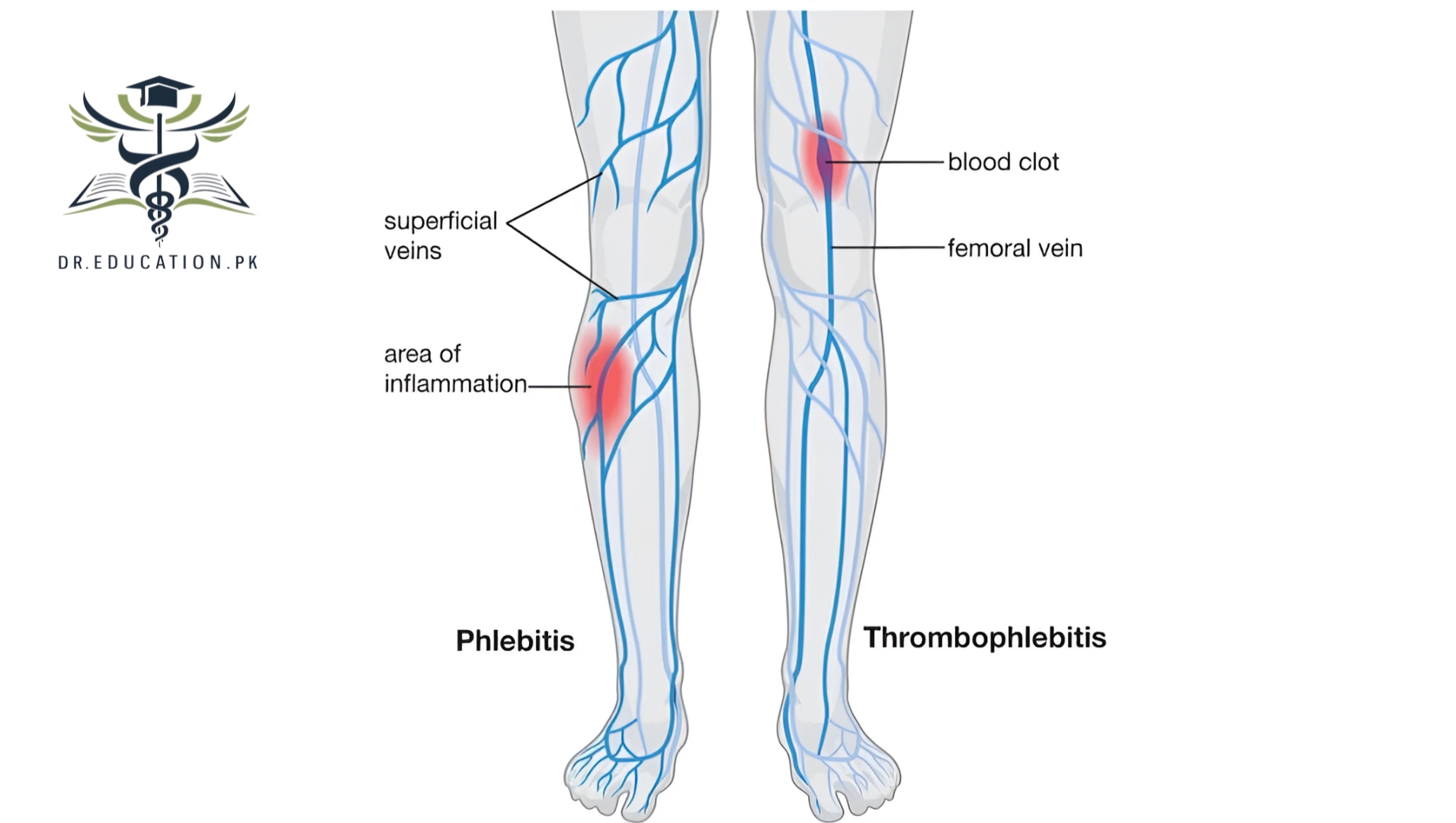
Phlebitis means inflammation of a vein. Thrombophlebitis is due to one or more blood clots in a vein that cause inflammation. Thrombophlebitis usually occurs in leg veins, but it may occur in an arm or other parts of the body. The thrombus in the vein causes pain and irritation and may block blood flow in the veins. Phlebitis can occur in both the surface (superficial) or deep veins.
- Superficial phlebitis affects veins on the skin surface. The condition is rarely serious and, with proper care, usually resolves rapidly. Sometimes people with superficial phlebitis also get deep vein thrombophlebitis, so a medical evaluation is necessary.
- Deep vein thrombophlebitis affects the larger blood vessels, usually deep in the legs. Large blood clots can form, which may break off and travel to the lungs. This is a serious condition called pulmonary embolism.
Types of phlebitis
Phlebitis can affect both superficial and deep veins.
Superficial phlebitis refers to the inflammation of a vein near the surface of your skin. It can result from a blood clot or from something causing irritation in a vein, such as an intravenous (IV) catheter.
This type of phlebitis usually isn’t serious, but it can lead to:
- infection of the surrounding skin
- wounds on the skin
- bloodstream infections
If a clot in the superficial vein is extensive enough and involves the area where the superficial vein and a deep vein come together, a DVT can develop.
Deep vein phlebitis refers to inflammation of a deeper, larger vein, such as those found in your legs. Deep vein phlebitis is more likely to be caused by a blood clot, which can have very serious consequences.
A blood clot may break off and travel to your lungs. This is called a pulmonary embolism (PE) and can be life threatening. It’s important to know the risk factors and symptoms of a DVT so you can seek prompt attention from a healthcare professional.
Phlebitis Causes
Superficial phlebitis can be a complication due to a medical or surgical procedure.
Injury to a vein increases the risk of forming a blood clot. Sometimes clots occur without an injury. Some risk factors for thrombophlebitis include the following:
- Prolonged inactivity – Staying in bed or sitting for many hours, as in a car or on an airplane, creating stagnant or slow flow of blood from the legs in a dependent position (This pooling of blood in the legs leads to thrombus formation.)
- Sedentary lifestyle – Not getting any exercise
- Obesity
- Smoking cigarettes
- Certain medical conditions, such as cancer or blood disorders, that increase the clotting potential of the blood
- Injury to your arms or legs
- Hormone replacement therapy or birth control pills
- Pregnancy
- Varicose veins
Symptoms
Inflammation is the body’s response to tissue damage. Symptoms that may occur in areas affected by superficial phlebitis include:
- tenderness
- redness, including long, thin lines along the vein’s path
- warm to the touch
- skin may feel hard
- itching and burning
- throbbing sensations
- swollen skin
- discomfort
- worsening symptoms when leg is lowered
- low grade fever if infection
Symptoms of acute superficial thrombophlebitis and DVT are similar to those of superficial phlebitis but more intense:
- more severe redness, warmth, swelling
- increased pain and discomfort
- occasionally discoloration can be more blue than red
- one leg more swollen than the other
- more feelings of aching, throbbing and leg heaviness
Who is at risk?
A number of factors can increase your risk of phlebitis. You may be more likely to experience phlebitis if you:
- have a personal or family history of blood clots
- have a blood clotting disorder, such as factor V Leiden thrombophilia
- take hormone therapy or birth control pills
- experience long periods of inactivity, which may be needed after surgery
- sit for long periods of time, such as during travel
- have certain cancers and cancer treatments
- are pregnant
- have overweight or obesity
- smoke
- misuse alcohol
- have varicose veins, which can increase your risk of superficial phlebitis
- are over age 60