What is Mpox(Monkey Pox)?
According to WHO,
Mpox is an infectious disease that can cause a painful rash, enlarged lymph nodes, fever, headache, muscle ache, back pain and low energy. Most people fully recover, but some get very sick.
Overview
What is mpox?
Mpox (previously known as monkeypox) is a rare disease caused by a virus. It leads to rashes and flu-like symptoms. Like the better-known virus that causes smallpox, it’s a member of the genus Orthopoxvirus.
Mpox spreads through close contact with someone who’s infected. You can also get it from an infected animal.
There are two known types (clades) of mpox virus — one that originated in Central Africa (Clade I) and one that originated in West Africa (Clade II). The current world outbreak (2022 to 2023) is caused by Clade IIb, a subtype of the less severe West African clade.
How common is mpox?
Mpox is rare. But the number of cases is increasing in Africa, as well as in regions that haven’t seen these infections before.
History and Discovery
Mpox was first identified in 1958 when two outbreaks occurred in colonies of monkeys kept for research, giving the disease its original name. However, despite the initial association with monkeys, the natural reservoir of mpox is believed to be rodents, particularly those found in African rainforests. Human cases of mpox were first recorded in 1970 in the Democratic Republic of the Congo (DRC), during a period when intensified smallpox surveillance was underway.
Since then, the disease has become endemic in several parts of Africa, with the majority of cases concentrated in the DRC and Nigeria. Outside of Africa, mpox cases have been sporadic until recent years, when outbreaks in non-endemic countries have garnered global attention.
Who does mpox affect?
Anyone can get mpox. In Africa, most cases are among children under 15 years old. Outside of Africa, the disease appears to be more common in men who have sex with men (MSM), but there are numerous cases in people who don’t fall into that category.
Symptoms and Causes
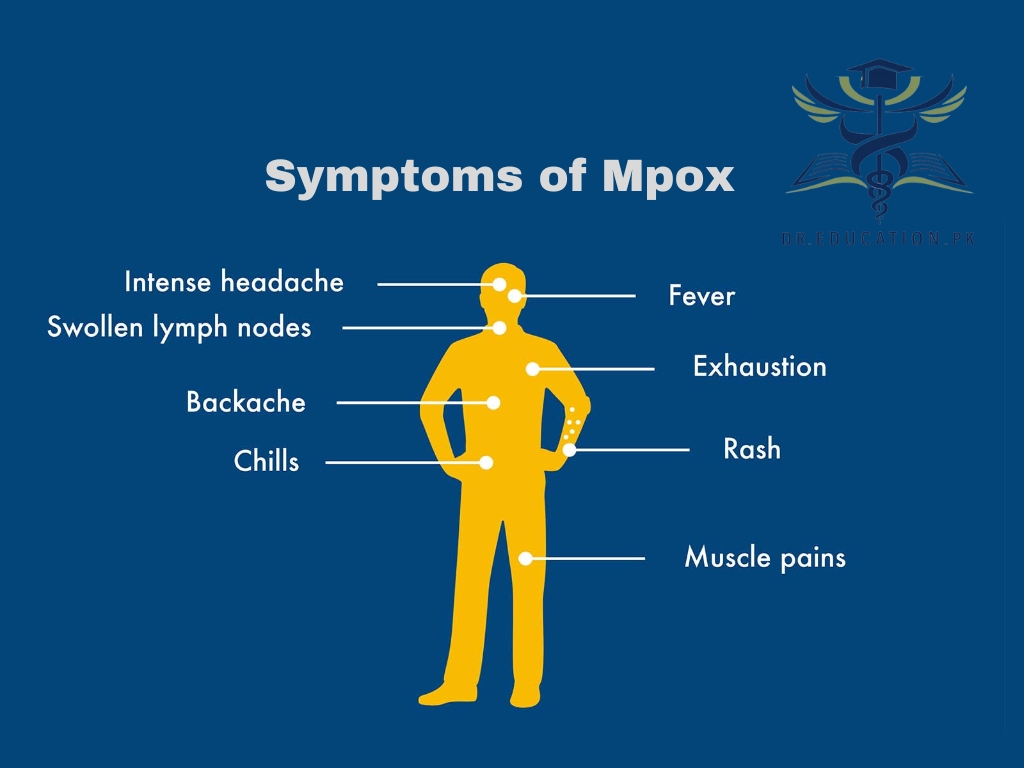
What are the signs and symptoms of mpox?
After exposure, it may be several days to a few weeks before you develop symptoms. Signs of mpox include:
- Fever.
- Rash.
- Swollen lymph nodes.
- Chills.
- Headache.
- Muscle aches.
- Fatigue.
A key feature that distinguishes mpox from other pox-like diseases, including smallpox, is lymphadenopathy (swollen lymph nodes), which occurs early in the disease. Lymphadenopathy tends to be localized in the neck, armpits, or groin and can be painful.
Eruption Phase (Rash Development)
After the fever and other systemic symptoms subside, a distinctive rash emerges. The rash begins as small flat spots, which then develop into raised bumps, and ultimately form fluid-filled blisters (vesicles). Over time, these vesicles become pustules, which are filled with pus, and eventually crust over, forming scabs. These scabs later fall off as the lesions heal.
- The rash often starts on the face before spreading to other parts of the body, including the palms of the hands and soles of the feet.
- Lesions may also be present on the mucous membranes of the mouth, genitalia, and eyes.
- The number of lesions can vary widely from a few to several thousand.
The entire process of rash evolution, from onset to the scabbing and healing of lesions, typically lasts for 2 to 4 weeks.
Complications
While most individuals recover from mpox, the disease can be severe and sometimes fatal, particularly in young children, pregnant women, and immunocompromised individuals. Potential complications include:
- Bacterial infections of the skin due to broken lesions
- Pneumonia
- Septicemia
- Encephalitis (inflammation of the brain)
- Corneal infections, which can lead to vision loss
The case fatality rate for mpox varies based on the viral clade, with estimates of 1-10% for the Central African clade and less than 1% for the West African clade.
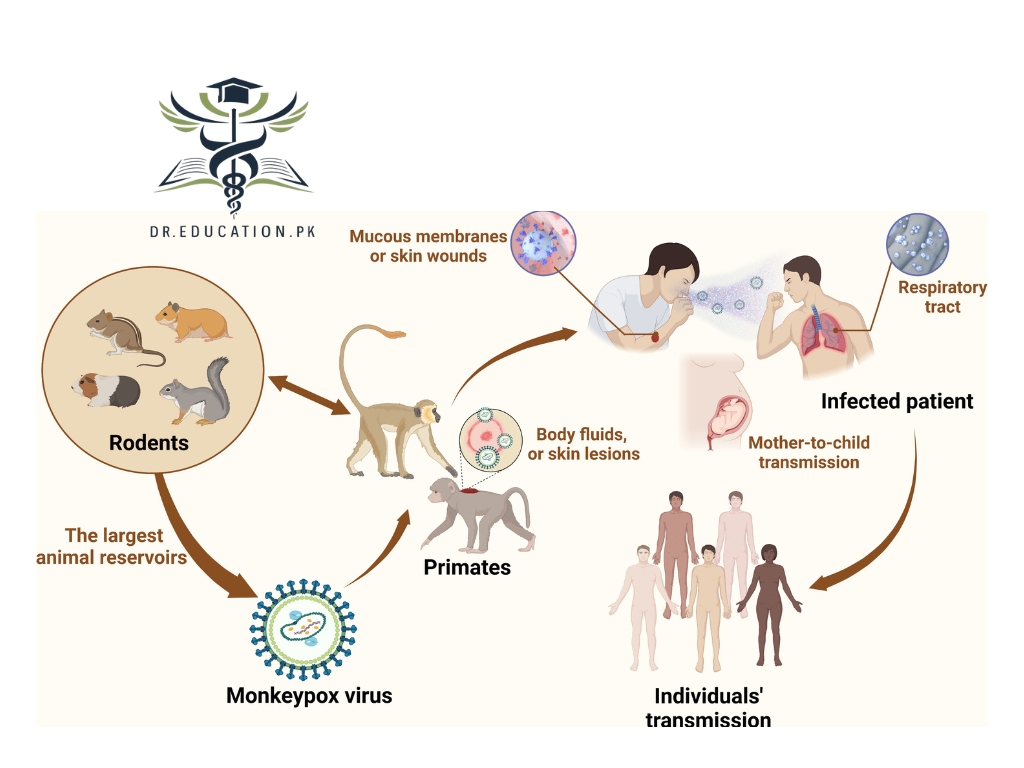
How do you catch mpox?
Mpox spreads when you come into contact with an animal or a person infected with the virus.
Person-to-person spread (transmission) occurs when you come in contact with the sores, scabs, respiratory droplets or oral fluids of a person who’s infected, usually through close, intimate situations like cuddling, kissing or sex. Research is ongoing, but experts aren’t sure if the virus is transmitted through semen or vaginal fluids.
Animal-to-person transmission occurs through broken skin, like from bites or scratches, or through direct contact with an infected animal’s blood, bodily fluids or pox lesions (sores).
You can also get mpox by coming into contact with recently contaminated materials like clothing, bedding and other linens used by a person or animal who’s infected.
Transmission and Risk Factors
Mpox is primarily transmitted to humans from animals, but human-to-human transmission can also occur. Transmission modes include:
Animal-to-Human Transmission
- Direct contact with the blood, bodily fluids, or lesions of infected animals.
- Bites or scratches from infected animals.
- Handling of infected wild animals, such as during hunting, may increase exposure risk.
- Consumption of improperly cooked meat from infected animals (a practice known as “bushmeat” consumption) is another possible route.
Human-to-Human Transmission
While animal-to-human transmission is more common in endemic areas, person-to-person transmission has been responsible for recent outbreaks. Human-to-human transmission occurs via:
- Direct contact with infectious sores, scabs, or bodily fluids from an infected person.
- Respiratory droplets during prolonged face-to-face contact (especially in household settings or healthcare facilities).
- Fomites, which are contaminated objects, such as bedding, towels, or clothing, that come into contact with an infected person.
The risk of transmission is higher in situations involving close, sustained contact, including sexual contact. While mpox is not classified as a sexually transmitted infection (STI), intimate physical interactions can facilitate the spread of the virus.
Diagnosis and Tests
How is mpox diagnosed?
Because mpox is rare, a healthcare provider may first suspect other rash illnesses, such as measles or chickenpox. But swollen lymph nodes usually distinguish mpox from other poxes.
To diagnose mpox, your healthcare provider takes a tissue sample from an open sore (lesion). Then, they send it to a lab for polymerase chain reaction (PCR) testing (genetic fingerprinting). You may also need to give a blood sample to check for the mpox virus or antibodies your immune system makes.
Treatment
There is no specific treatment for mpox, but supportive care and symptom management play a central role in patient recovery. In severe cases, antiviral treatments and immune therapies may be employed.
Supportive Care
- Hydration and nutritional support.
- Fever management with antipyretics.
- Pain management for severe headache, muscle aches, or lesions.
Antiviral Treatment
- Tecovirimat: An antiviral drug approved for the treatment of smallpox that has shown efficacy against mpox in animal studies. It is now being used in certain severe or high-risk mpox cases, though access is limited.
- Cidofovir: Another antiviral used in treating severe poxvirus infections, including mpox, particularly in immunocompromised patients.
- Vaccinia Immune Globulin (VIG): Used in some cases to boost immunity, particularly in severe or complicated infections.
Prevention
How do you prevent mpox?
If you’re at risk for mpox, getting vaccinated helps stop the spread. Other forms of prevention include decreasing human contact with infected animals and limiting person-to-person spread.

Mpox vaccines
Vaccines developed for smallpox also provide protection against mpox. Mpox vaccines are currently only recommended for people who’ve been exposed to, or are likely to be exposed to, mpox. You might be at higher risk of exposure if:
- You’ve been in close contact with someone with mpox.
- Someone you’ve had sex with in the past two weeks has been diagnosed with mpox.
- You’ve had sex at a sex club, bathhouse or other commercial sex venue in the past six months.
- You’ve had sex at an event or location where mpox was spreading.
- You have a sex partner who’s been in any of the above situations.
- You expect to be in one of the above situations.
If you’re a man who has sex with men, a transgender person or a nonbinary person, you may also be at risk if you’ve:
- Been diagnosed with one or more sexually transmitted infections (STIs) in the past six months. This includes acute HIV, gonorrhea, syphilis, chancroid or chlamydia.
- Had sex with more than one person in the past six months.
It’s important to get vaccinated before or as soon as possible after exposure. Talk to a healthcare provider if you’re unsure if you should get vaccinated. If you’d like to get your shot in a more concealed location on your body, your provider can give it to you in your shoulder blade instead of your forearm.
Other ways to prevent mpox
In addition to vaccines, other ways to help prevent the spread of mpox include:
- Avoiding contact with infected animals (especially sick or dead animals).
- Avoiding contact with bedding and other materials contaminated with the virus.
- Thoroughly cooking all foods that contain animal meat or parts.
- Washing your hands frequently with soap and water.
- Avoiding contact with people who may be infected with the virus.
- Practicing safe sex, including the use of condoms and dental dams.
- Wearing a mask that covers your mouth and nose when around others.
- Cleaning and disinfecting frequently touched surfaces.
- Using personal protective equipment (PPE) when caring for people infected with the virus.

When to see a doctor
If you suspect that you have been exposed to mpox or are experiencing symptoms, it’s important to seek medical advice promptly. Here are the specific circumstances under which you should see a doctor:
1. Exposure to a Confirmed or Suspected Case
- Direct contact with someone diagnosed with or suspected of having mpox.
- Close contact with infected animals (particularly in regions where mpox is endemic).
- Handling contaminated items (like clothing, bedding, or towels) of an infected person.
If you’ve been exposed, even without symptoms, it’s important to inform your healthcare provider so they can monitor you for signs of infection and potentially recommend quarantine measures.
2. Development of Symptoms
Seek medical attention if you experience any of the following symptoms, especially if you have been in a high-risk area or had exposure to a suspected case:
- Fever, chills, or exhaustion that lasts for several days.
- Headache, muscle aches, or back pain.
- Swollen lymph nodes in the neck, armpits, or groin.
- Rash or skin lesions that start on the face, hands, or other areas of the body, evolving from flat spots to raised bumps and fluid-filled blisters.
- Difficulty breathing or chest pain (which can be a sign of respiratory involvement).
3. High-Risk Individuals
Certain groups are at higher risk of severe illness from mpox. If you belong to one of the following categories and notice any symptoms, seek medical attention right away:
- Immunocompromised individuals (e.g., those with HIV, cancer patients, transplant recipients).
- Pregnant women, as the infection can pose risks to the fetus.
- Children, especially under the age of 8.
- Individuals with skin conditions like eczema, which may worsen with mpox lesions.
4. Severe Symptoms or Complications
Immediate medical attention is required if you develop more severe symptoms, such as:
- Severe pain or infections around the lesions.
- Eye problems, such as redness or pain, which can indicate complications involving the cornea.
- Neurological symptoms, such as confusion, seizures, or changes in mental status, which may be signs of encephalitis.
- Signs of secondary bacterial infection around the lesions, such as redness, warmth, or pus, which might require antibiotics.
5. Persistent or Worsening Symptoms
Even if your initial symptoms seem mild, consult a doctor if:
- Symptoms persist beyond 2-4 weeks, as the illness should typically resolve by then.
- The rash or lesions do not heal or become more extensive.
- You develop new symptoms while recovering, such as high fever or worsening fatigue, which may signal a complication.
In summary, if you believe you are at risk for mpox or develop any associated symptoms, it’s crucial to consult a healthcare provider for proper diagnosis and guidance. Early intervention can help manage symptoms and prevent further spread.
Living With
How do I take care of myself?
If you have mpox symptoms, there are over-the-counter (OTC) medications that can help you feel better, including:
- Pain relievers and fever reducers. Medicines like ibuprofen (Advil®, Motrin®) and acetaminophen (Tylenol®) can help relieve your symptoms.
- Oatmeal baths. Soaking in a warm bath with colloidal oatmeal can relieve the dry, itchy feeling that comes with skin rashes.
- Isolate yourself if you’re infected. Avoid contact with others until all of your lesions have scabbed.
- Cover single or local ulcers or sores. Use gauze or bandages to limit the spread to others and the environment.
- Take good care. It’s important to stay home and rest when you’re sick, wear a mask around others and drink plenty of fluids.
- Avoid contact with pets (especially rodents).
What is the difference?
Mpox vs. chickenpox
Although they both cause skin rashes, different viruses cause mpox and chickenpox. Mpox is an orthopoxvirus, while chickenpox is a herpes virus. Both viruses can spread through skin-to-skin or prolonged face-to-face contact, but chickenpox is very contagious and spreads more easily than mpox. People with mpox are more likely to have swollen lymph nodes than people with chickenpox.
The rashes act differently, too. While the chickenpox rash can appear in waves, mpox sores develop at the same time. Chickenpox symptoms — including the rash — tend to get better within two weeks, while it takes two to four weeks for mpox to resolve.

Mpox vs. smallpox
Smallpox and mpox are both part of the Orthopoxvirus genus, so they’re caused by similar but distinct viruses. Thanks to effective vaccines, smallpox was eradicated (is no longer a circulating disease) by 1980. Smallpox was very contagious and spread more easily than mpox. Mpox symptoms are similar to smallpox, but milder.
Conclusion from Dreducation.pk
Mpox, previously known as monkeypox, is a viral infectious disease that primarily causes skin lesions, fever, and swollen lymph nodes. Although it has been endemic to parts of Africa for decades, recent outbreaks have brought global attention to its spread. Mpox is caused by a virus from the Orthopoxvirus genus, the same family as smallpox, but it is generally less severe.
Transmission occurs through close contact with infected individuals or animals, with symptoms ranging from flu-like conditions to painful skin rashes that evolve into pustules and scabs. Most people recover within 2-4 weeks, though complications can arise, especially in vulnerable groups like young children, pregnant women, and immunocompromised individuals.
While there is no specific cure, supportive care and antiviral treatments are available, and smallpox vaccines offer protection against mpox. Prevention focuses on reducing contact with infected individuals or animals, practicing good hygiene, and using protective measures like vaccination and personal protective equipment.
Understanding the risks, symptoms, and transmission modes is crucial for curbing the spread of mpox and managing outbreaks. Early detection, timely medical care, and preventive strategies can help minimize its impact, ensuring better outcomes for individuals and communities at risk.