Phimosis
According to Wikipedia,
Phimosis is a condition in which the foreskin of the penis cannot stretch to allow it to be pulled back past the glans. A balloon-like swelling under the foreskin may occur with urination. In teenagers and adults, it may result in pain during an erection, but is otherwise not painful. Those affected are at greater risk of inflammation of the glans, known as balanitis, and other complications.
Overview
How to Pronounce Phimosis?
Phimosis is Pronounced as (fie-MOH-sis).
What is phimosis?
Phimosis is a condition of the penis that occurs in some uncircumcised adults and children. If you have phimosis, you can’t pull back (retract) the foreskin (prepuce). It may look like your penis has rings around the tip. Under typical circumstances, you should be able to pull back your foreskin easily and see the entire head (glans) of your penis.
Having phimosis isn’t necessarily a problem. Babies have phimosis at birth, and their tight foreskin will usually loosen as they get older without treatment. Phimosis becomes a problem when it causes symptoms, such as a pinhole-sized opening or you can’t pull back your foreskin enough to clean the area underneath.
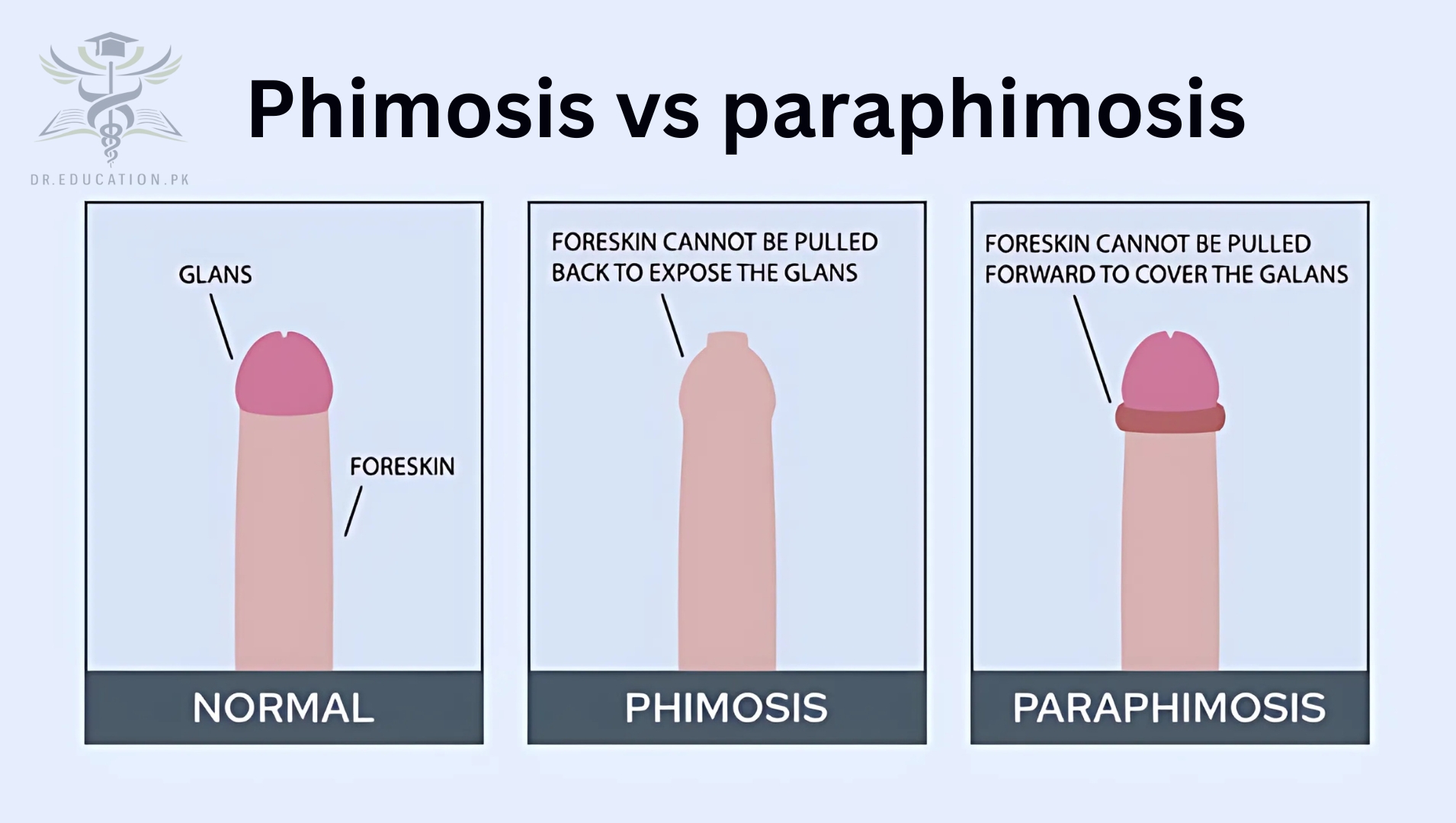
Phimosis vs. paraphimosis
Phimosis can sometimes lead to a dangerous condition called paraphimosis. That’s when the foreskin gets stuck behind the head of the penis and can’t be pushed back into place. It can happen when the foreskin is tight and you force it to retract. It can cut off the flow of blood to your penis and needs to be treated right away.
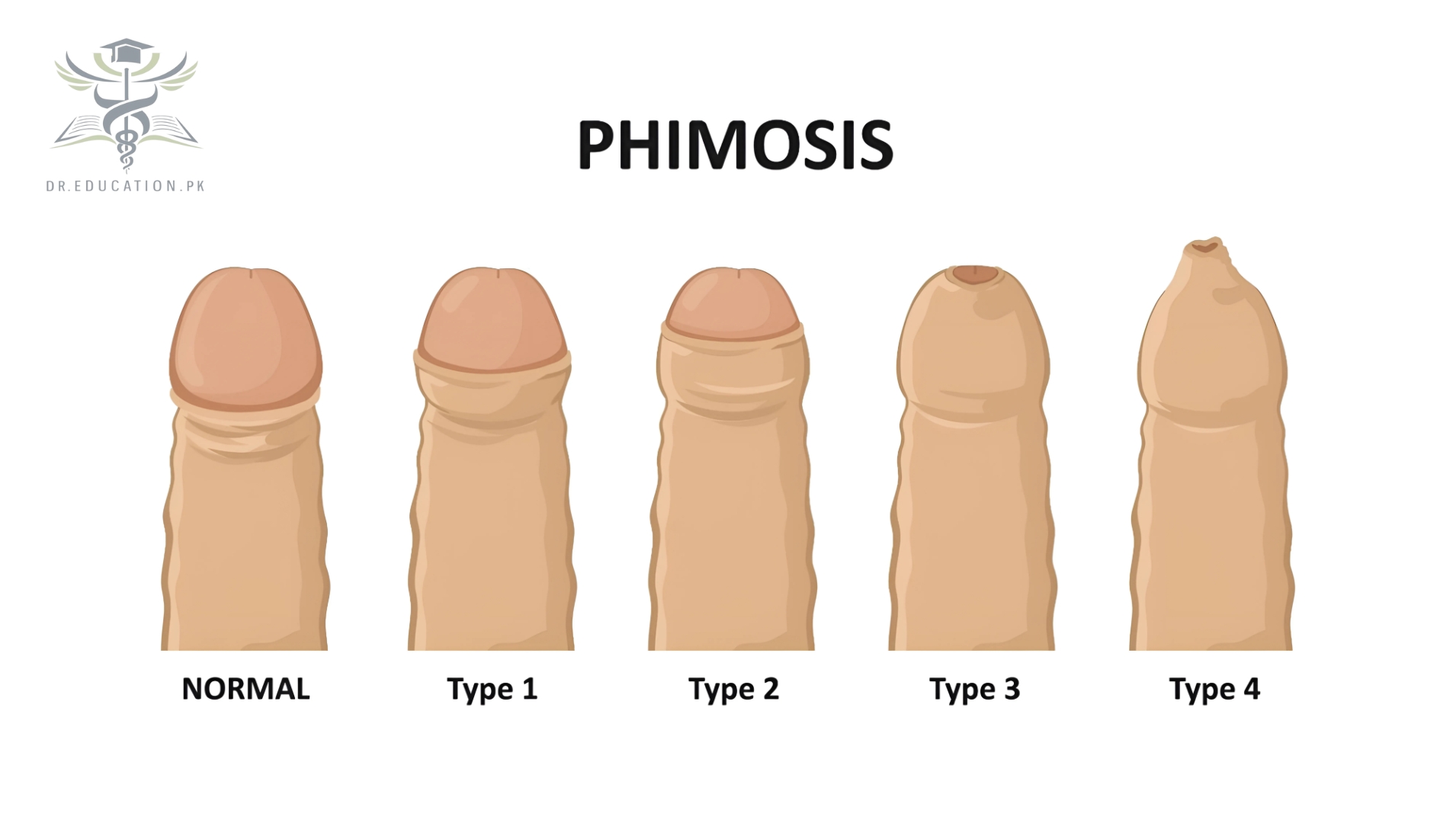
What are the types of phimosis?
There are two types of phimosis:
- Physiologic phimosis. Physiologic phimosis occurs more often in children. It usually resolves as they get older.
- Pathologic (congenital) phimosis. Infection, inflammation or scarring cause pathologic phimosis. Lichen sclerosus is a common cause.
Phimosis in adults
Phimosis is natural in young children. In older children or adults, it can be caused by an infection, inflammation, or a skin condition.
How common is phimosis?
Nearly all babies assigned male at birth (AMAB) have physiological phimosis. As new-borns age, the foreskin changes gradually so it can pull back. Medical professionals estimate only about 1% of people still have physiologic phimosis when they’re 16 or older.
Less than 1% of children have pathologic phimosis.
Phimosis Causes
In babies and young children, phimosis is something they’re born with, and they usually grow out of it. That’s called physiologic phimosis. Pathologic phimosis is caused by something else, such as:
Scar tissue. Infections can scar the foreskin, which might make the skin less stretchy. The tough tissue can be hard to pull back.
Injury. Don’t forcefully move your foreskin. Go easy on it. Pulling or stretching it can cause tiny tears and inflammation that eventually lead to phimosis.
Skin conditions. A skin condition called penile lichen sclerosus or balanitis xerotic obliterans is a leading cause of phimosis in adults. It can also be caused by eczema and psoriasis.
Medical conditions. If you have diabetes, you’re more likely to have balanitis, an infection of the tip of penis. Talk to your doctor about your complete medical history so they can treat you properly.
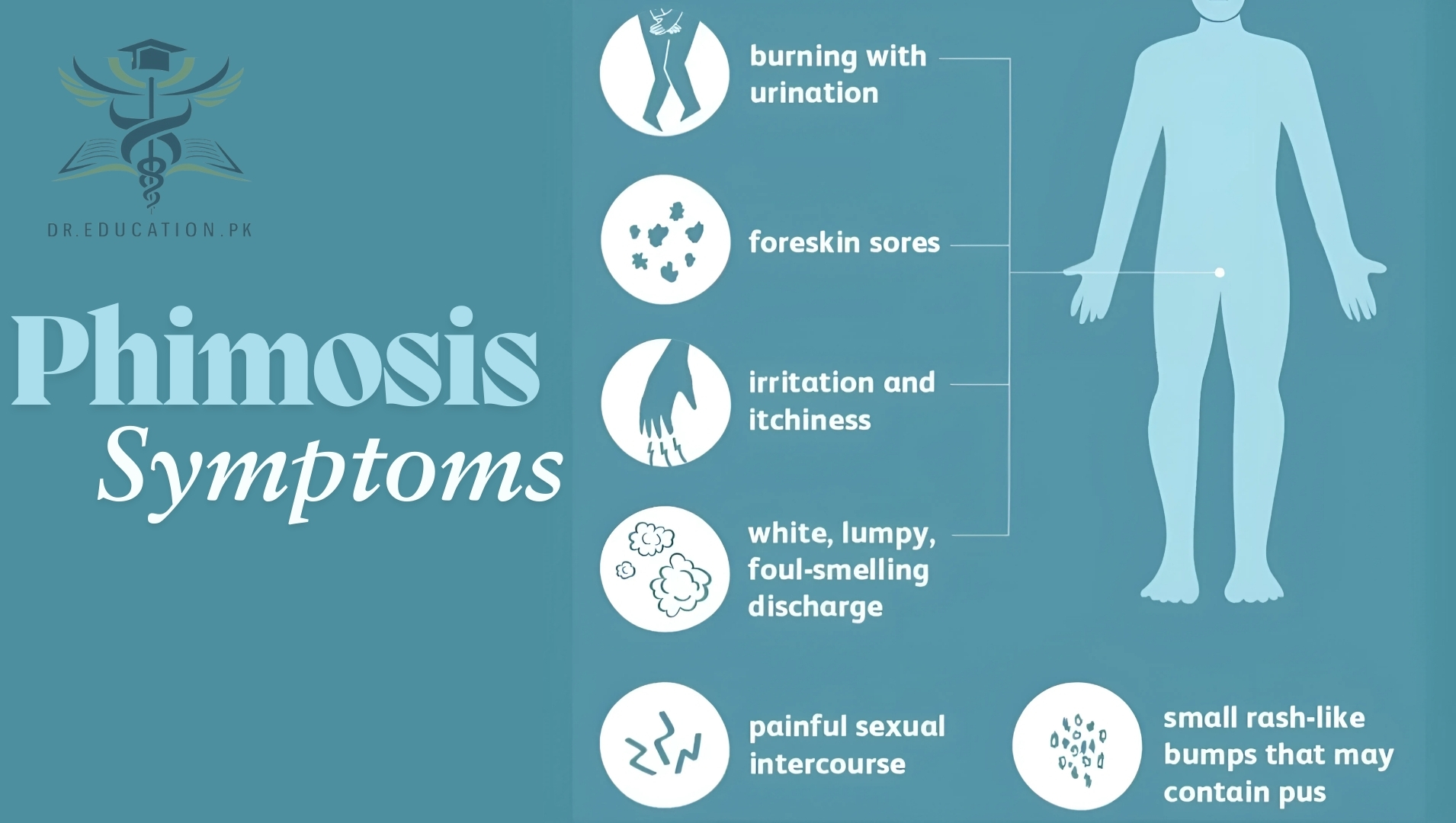
What are the symptoms of phimosis?
The primary symptom of phimosis is that you can’t pull the foreskin back from the head of your penis. But other phimosis symptoms may include:
- Discoloration (red, purple, dark brown or black), which may occur if there’s irritation or you have an infection.
- Swelling, which may occur if there’s irritation or you have an infection.
- Soreness or pain.
- Pain while peeing (dysuria).
- Weak pee stream.
- Blood in your pee (hematuria).
- Smegma.
- Pain when you get an erection or have sexual intercourse.
What does phimosis look like?
If you have phimosis, it may look like your penis has rings or rubber bands around the tip. Most importantly, you can’t pull back your foreskin.
Phimosis Complications
Phimosis can lead to a number of complications, including:
- Infections in your foreskin and urinary tract
- Paraphimosis, when the foreskin gets stuck behind the head of the penis
- Tears in your foreskin. Be gentle when you try to pull it back, and use a condom and plenty of lubrication when you have sex.
If you have phimosis, you’re also more likely to get penile cancer
How is phimosis diagnosed?
A healthcare provider can diagnose phimosis by reviewing your symptoms and performing a physical exam.
They may also order tests to determine if you have an infection. Tests may include:
- Pee test (urinalysis).
- Urethral discharge culture.
Phimosis Treatment
You can get treatment in an outpatient setting by a urologist. How they treat you depends on how serious your condition is and what symptoms you’re having. They’ll also consider the cause of the problem and ask what kind of solutions you prefer.
Phimosis treatment without surgery
For a young child, treatment usually isn’t needed. Phimosis will go away on its own as the child grows and the foreskin loosens naturally. That process can be helped along if they work on gently retracting and stretching their foreskin a few times day, only as far as it can be moved without pain. Bath time is a good opportunity.
Phimosis cream
Another option is a medicated cream or ointment that you apply to your foreskin several times a day for several weeks. It usually contains a steroid, like betamethasone, fluticasone propionate, hydrocortisone, or triamcinolone. This can soften and loosen the skin, and is often combined with stretching exercises.
Phimosis surgery
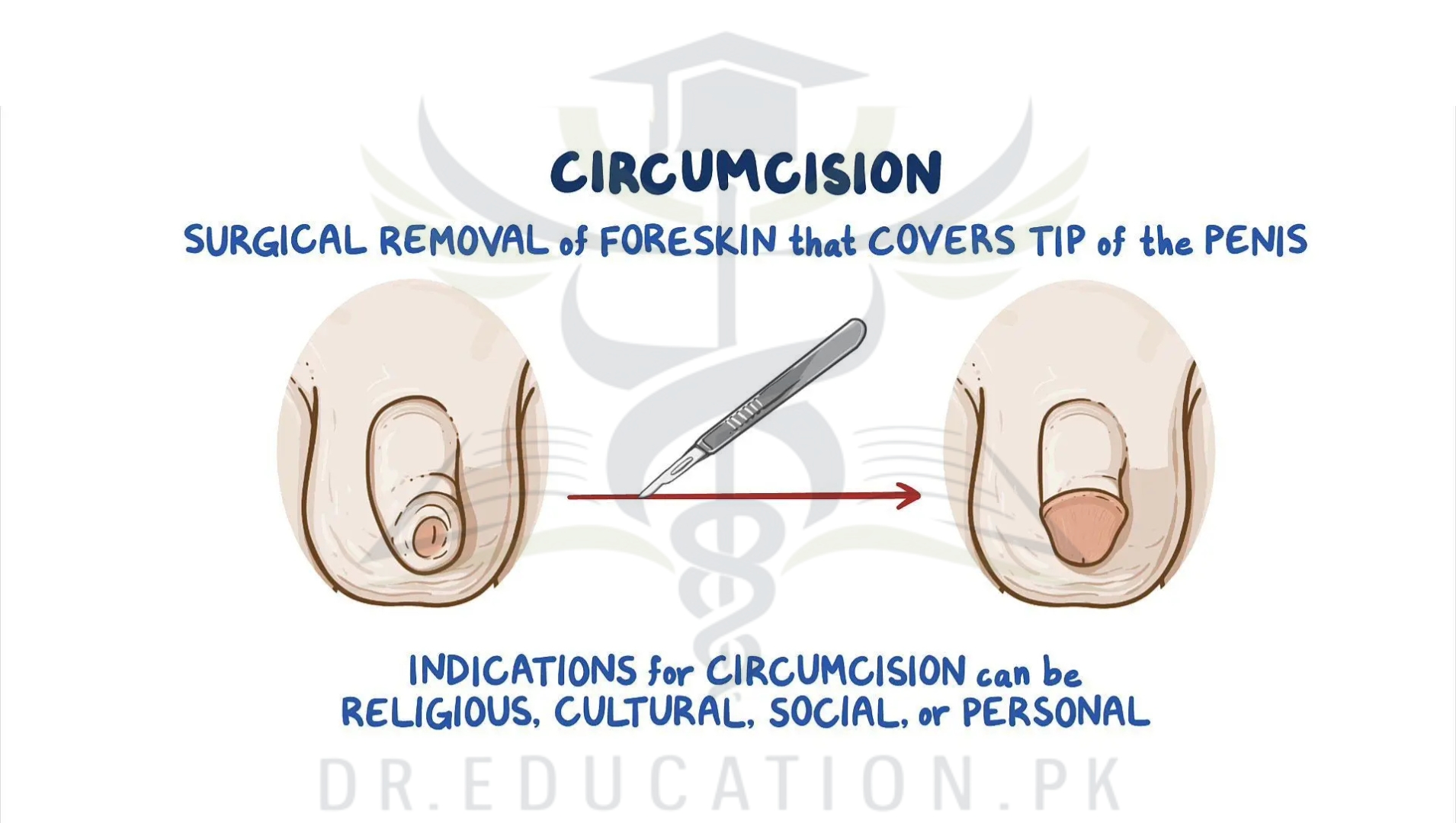
If other treatments don’t work, phimosis can be fixed with surgery. In one procedure, a surgeon makes small cuts in the foreskin that make it easier to pull it back. Another procedure, called circumcision, removes the foreskin entirely.
Circumcision may be the best option if you get infections often, if you have a lot of scar tissue, or if the phimosis is caused by balanitis xerotic obliterans.
Should I get circumcised if I have phimosis?
Healthcare providers recommend circumcision for adults if:
- Lichen sclerosus causes phimosis.
- The phimosis is severe.
- A corticosteroid cream doesn’t work.
- Sexual intercourse, including masturbation, is painful.
What are the complications or side effects of phimosis treatment?
Topical corticosteroid creams don’t typically have side effects.
Common circumcision complications may include:
- Bleeding.
- Infection.
- Your foreskin is too short or long.
- Pain.
How soon after treatment will I feel better?
It takes about a week to 10 days to feel better after circumcision.
Phimosis Prevention
Getting circumcised will keep phimosis from happening.
You can also prevent infections that cause phimosis by keeping your penis clean and taking steps to prevent sexually transmitted infections.
The penis head and the foreskin need to be washed and dried regularly. Be gentle with the skin when you pull it back, and put it back in place when you finish.
When to see a doctor?
You should consider seeing a doctor for phimosis if you experience any pain, especially while urinating or during erections. If you notice any swelling, redness, or unusual odor, or if there’s difficulty with urination, it’s a good idea to get it checked out. Repeated infections under the foreskin, or if it becomes increasingly hard to retract the foreskin over time, are also signs that medical advice could be helpful. A doctor can offer guidance on safe, effective treatments to improve comfort and manage the condition properly.
Conclusion from Dreducation.pk
In conclusion, phimosis is a common condition in children and often resolves naturally as they grow. However, in adults, phimosis may lead to discomfort, difficulty with hygiene, or complications like infections if left untreated. Understanding the symptoms, causes, and types of phimosis, as well as when to seek medical advice, can help manage the condition effectively. With options ranging from stretching exercises to medicated creams and, in severe cases, surgical interventions, treatment is available based on individual needs. Maintaining proper hygiene and monitoring symptoms are key to preventing complications and ensuring overall well-being.