Angina Pectoris
According to Wikipedia,
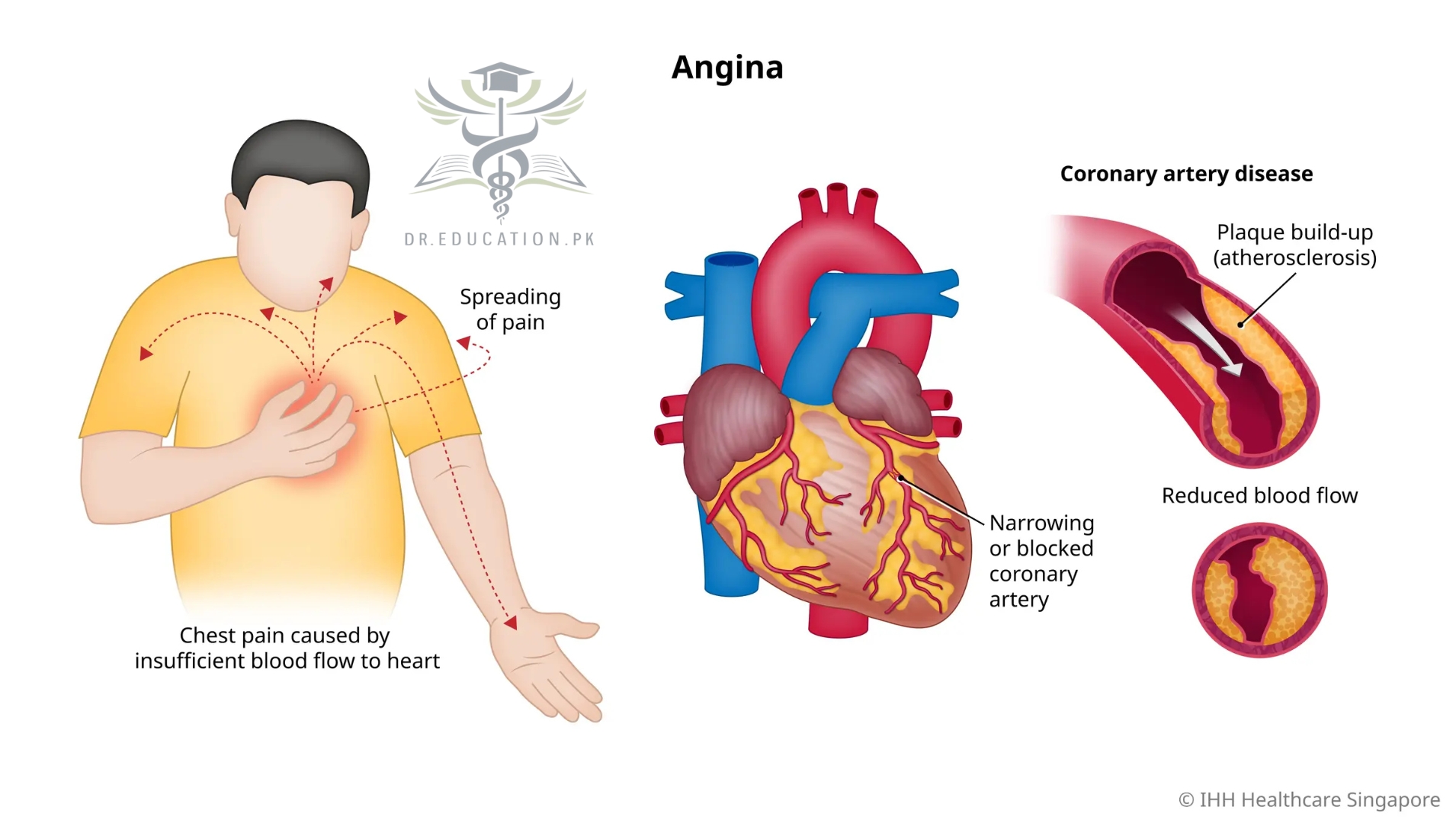
Angina pectoris, is chest pain or pressure, usually caused by insufficient blood flow to the heart muscle (myocardium). It is most commonly a symptom of coronary artery disease.
Overview
What is Angina Pectoris?
Angina is chest pain or discomfort that happens when your heart isn’t receiving enough oxygen-rich blood. As a result, your heart may beat faster and harder to gain more blood, causing you noticeable pain. Angina isn’t a disease. It’s a symptom and a warning sign of heart disease.
It’s a symptom of heart disease, and it happens when something blocks your arteries or there’s not enough blood flow in the arteries that bring oxygen-rich blood to your heart.
Angina usually goes away quickly. Still, it can be a sign of a life-threatening heart problem. It’s important to find out what’s going on and what you can do to avoid a heart attack.
Usually, medicine and lifestyle changes can control angina. If it’s more serious, you may need surgery. Or you may need what’s called a stent, a tiny tube that props open arteries.
About 10 million people in the U.S. experience angina. So, if you have this symptom, you’re certainly not alone. It’s important to learn more about angina, what causes it and how to manage it in your daily life.
What does angina feel like?
Most people with angina describe having chest pain or pressure. Or they describe a squeezing sensation or a tightness in their chest. Some people say it feels like indigestion. Others say it’s hard to describe angina with words.
The discomfort usually begins behind your breastbone. Sometimes, you may not be able to locate exactly where the pain is coming from.
Pain/discomfort you feel in your chest may spread to other parts of your upper body. These include your neck, jaw, shoulders, arms, back or belly.
Lack of oxygen to your heart can cause other symptoms, known as “angina equivalents.” These are symptoms that you don’t feel in your chest, including:
- Fatigue.
- Nausea or vomiting.
- Shortness of breath.
- Sweating a lot.
Angina vs. heart attack
Heart disease can also cause a heart attack. The decrease in blood flow to your heart in a heart attack is longer than that in angina. This causes part of the heart muscle to die, which is permanent damage. The drop in blood flow to your heart in angina is short. So it doesn’t cause permanent damage.

Angina Types
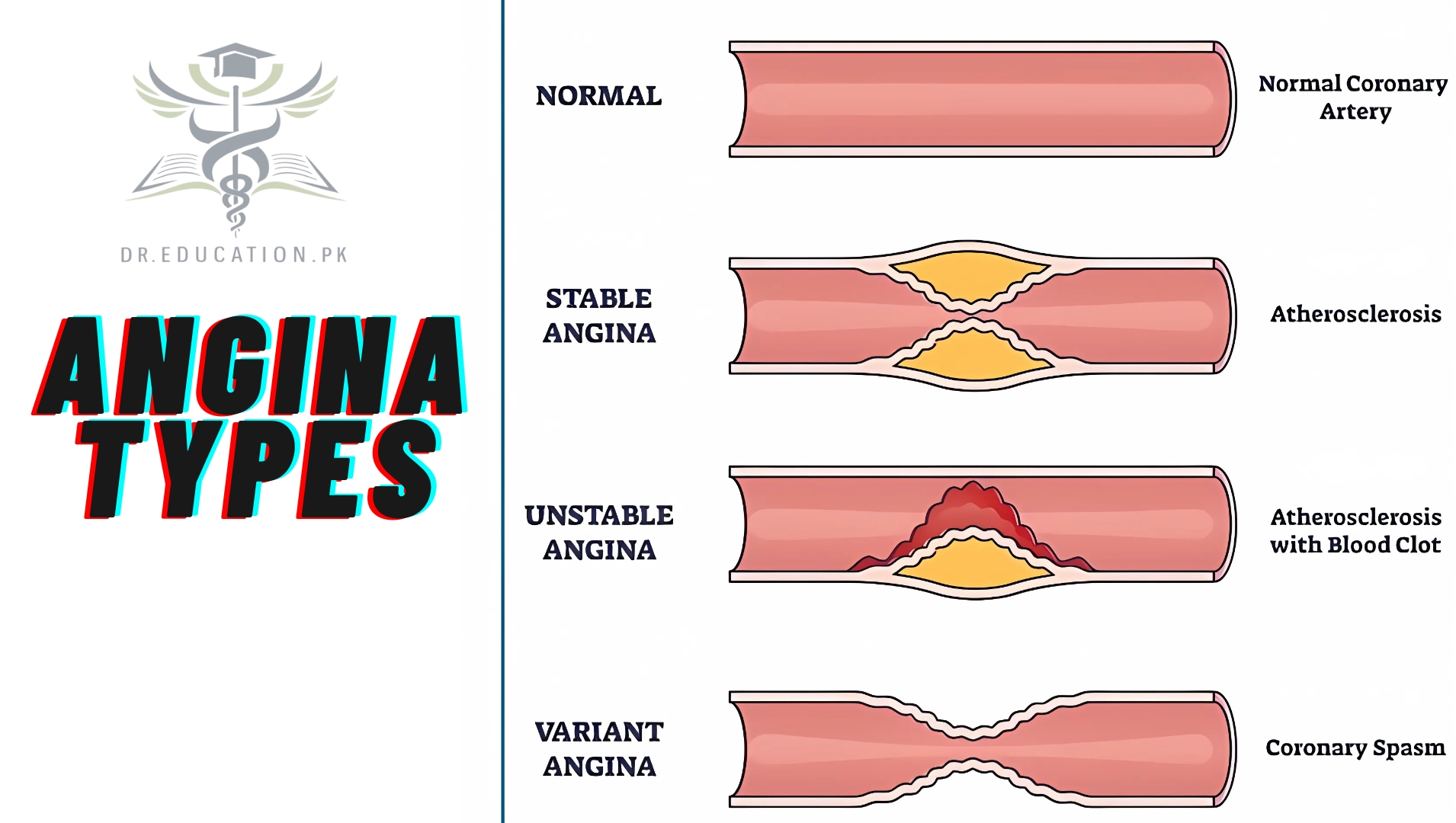
There are different types of angina:
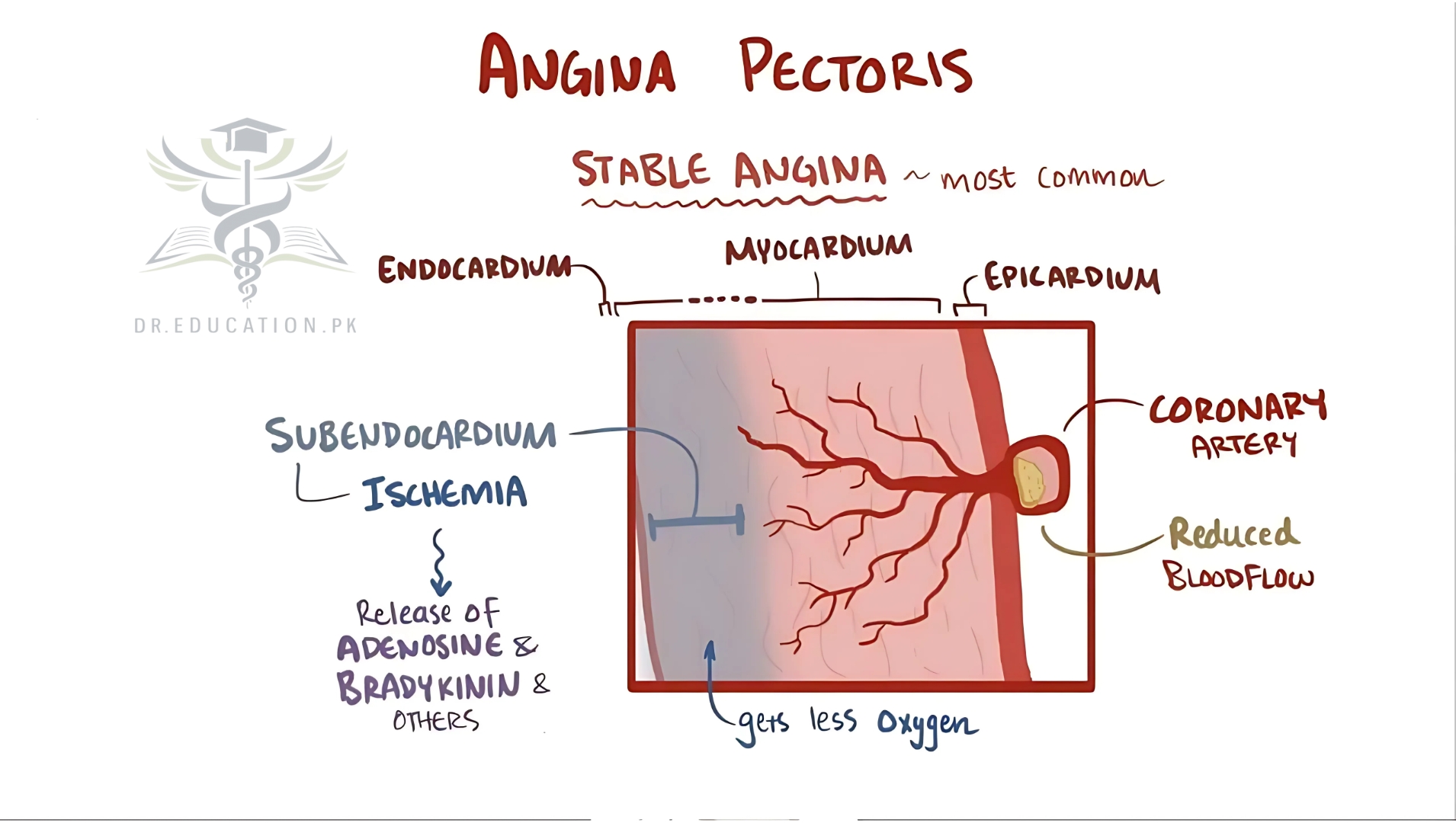
Stable angina
This is the most common type of angina. Physical activity or stress can trigger it. It usually lasts a few minutes, and it goes away when you rest. It isn’t a heart attack, but it can be a sign that you’re more likely to have one. Tell your doctor if this happens to you.
Unstable angina
You can have unstable angina while you’re at rest or not very active. The pain can be strong and long-lasting, and it may come back again and again. It can be a signal that you’re about to have a heart attack, so see a doctor right away.
Microvascular angina
With microvascular angina, you have chest pain but no coronary artery blockage. Instead, it happens because your smallest coronary arteries aren’t working the way they should, so your heart doesn’t get the blood it needs. The chest pain usually lasts more than 10 minutes. This type is more common in women.
Prinzmetal’s angina (variant angina)
This type of angina is rare. It might happen at night while you’re sleeping or resting. Your heart arteries suddenly tighten or narrow. It can cause a lot of pain, and you should get it treated.
What causes angina pectoris?
Angina pectoris occurs when your heart muscle (myocardium) does not get enough blood and oxygen. Not enough blood supply is called ischemia.
Angina can be a symptom of coronary artery disease (CAD). This is when arteries that carry blood to your heart become narrowed and blocked. This can happen because of:
- Hardening of arteries (atherosclerosis)
- A blood clot
- Plaque in an artery that can rupture (unstable plaque)
- Poor blood flow through a narrowed heart valve
- Lessened pumping of the heart muscle
- Coronary artery spasm
Angina Symptoms
Chest pain is the symptom, but it affects people differently. You may have:
- Aching
- Burning
- Discomfort
- Dizziness
- Fatigue
- Feeling of fullness in your chest
- Feeling of heaviness or pressure
- Upset stomach or vomiting
- Shortness of breath
- Squeezing
- Sweating

You might mistake an aching or burning for heartburn or gas.
You’re likely to have pain behind your breastbone, which can spread to your shoulders, arms, neck, throat, jaw, or back.
Stable angina often gets better with rest. Unstable angina may not, and it could get worse. It’s an emergency that needs medical help right away.
Symptoms of angina pectoris?
These are the most common symptoms of angina:
- A pressing, squeezing, or crushing pain, usually in the chest under your breastbone
- Pain that may also occur in your upper back, both arms, neck, or ear lobes
- Chest pain that spreads to your arms, shoulders, jaw, neck, or back
- Shortness of breath
- Weakness
- Extreme tiredness (fatigue)
- Feeling faint
Angina chest pain is usually relieved within a few minutes by resting or by taking prescribed cardiac medicine, such as nitroglycerin.
Angina Risk Factors
Some things about you or your lifestyle could put you at a higher risk of angina, including:
- Older age
- Family history of heart disease
- High blood pressure
- High cholesterol
- Diabetes
- Obesity
- Stress
- Smoking
- Not getting enough exercise
How is angina pectoris diagnosed?
Your healthcare provider will ask about your medical history. They will give you a physical exam. A healthcare provider can often diagnose angina from symptoms and how and when they occur. You may also have tests such as:
- Electrocardiogram (ECG). This test records the electrical activity of the heart. It shows abnormal rhythms (arrhythmias). And it detects heart muscle damage.
- Stress test. This is done while you exercise on a treadmill or pedal a stationary bike. The test checks your heart’s ability to function when under stress such as exercise. Breathing and blood pressure rates are also watched. A stress test may be used to find coronary artery disease.
- Cardiac catheterization. A wire is passed into the coronary arteries. Then a contrast dye is injected into your artery. X-ray images are taken to see the narrowing, blockages, and other problems of certain arteries.
- Cardiac MRI. This test can look at the amount of blood flow to the heart muscle. It may not be available at all medical centers.
- Coronary CT scan. This test looks at the amount of calcium and plaque inside the blood vessels of the heart. It can also show blood flow through the coronary arteries.
Management and Treatment
How is angina treated?
Your healthcare provider will treat the underlying heart problem that’s causing your angina. The goals of treatment are to improve blood flow to your heart and lower your risk of complications. Your provider will give you a physical exam and perform testing to learn more about your condition and determine the best treatments.
Common treatment options include:
- Anticoagulants or antiplatelet drugs to lower your risk of blood clots.
- Blood pressure medications.
- Cholesterol medications.
- Medications used specifically to treat angina.
- Lifestyle changes.
- Coronary artery bypass grafting (CABG).
- Percutaneous coronary intervention (PCI), also called coronary angioplasty and stenting.
Even with treatment, some people still experience angina. Your provider may prescribe a medication to quickly open your blood vessels when you have pain. Nitroglycerin is a common angina medication.
Enhanced external counterpulsation (EECP) is another option for people with continued pain. This therapy applies pressure to your lower legs to help improve blood flow to your heart. It may help ease your angina.
Lifestyle changes
You can still be active, but it’s important to listen to your body. If you feel pain, stop what you’re doing and rest. Know what triggers your angina, like stress or intense exercise. Try to avoid things that tend to set it off. For example, if large meals cause problems, eat smaller ones and eat more often. If you still feel pain, talk to your doctor about having more tests or changing your medications. Because angina can be a sign of something dangerous, it’s important to get checked out.
These lifestyle tips may help protect your heart:
- If you smoke, stop because it can damage your blood vessels and increase your heart disease risk.
- Eat a heart-healthy diet to lower your blood pressure and cholesterol levels. When those are out of normal range, your chance for heart disease can rise. Eat mainly fruits and vegetables, whole grains, fish, lean meat, and fat-free or low-fat dairy. Limit salt, fat, and sugar.
- Do things to cut down on stress like meditation, deep breathing, or yoga to relax.
- Exercise most days of the week.
- See your doctor regularly.
How can I prevent angina?
You can help prevent angina by living a heart-healthy lifestyle. Take these steps for better heart health:
- Avoid smoking and all tobacco products. Also, avoid exposure to secondhand smoke.
- Eat a heart-healthy diet. The DASH Diet and the Mediterranean Diet are good options. Lower your intake of saturated fat, trans fat, sugar and sodium.
- Find new ways to manage stress. Try meditation, yoga or talking with a counselor or friend. Journal writing is another way to process emotions and concerns.
- Keep a weight that’s healthy for you. Ask your provider what you should aim for, and ask for advice on how to reach that goal.
- Manage risk factors for coronary artery disease. These include high blood pressure, high cholesterol, high triglycerides and diabetes.
- Move around more. Try to exercise for at least 150 minutes (2.5 hours) every week. Go for walks or find other activities you enjoy. Find a friend to join you.
- Take medications prescribed by your cardiologist. Many of these medications have been shown to reduce or eliminate the anginal symptoms you have.
Conclusion from Dreducation.pk
In conclusion, angina pectoris is a significant warning sign of underlying heart disease and often indicates restricted blood flow to the heart. Understanding the different types of angina, such as stable, unstable, microvascular, and Prinzmetal’s angina, helps in recognizing the severity and potential risk factors associated with this condition.
While stable angina can often be managed with lifestyle changes and medication, unstable angina requires immediate medical attention due to its association with impending heart attacks. Angina treatment typically involves a combination of lifestyle adjustments, medications, and, in severe cases, surgical interventions to improve blood flow to the heart.
Proactive management, including quitting smoking, following a heart-healthy diet, reducing stress, and regular physical activity, is crucial for preventing angina symptoms and lowering the risk of further heart complications.