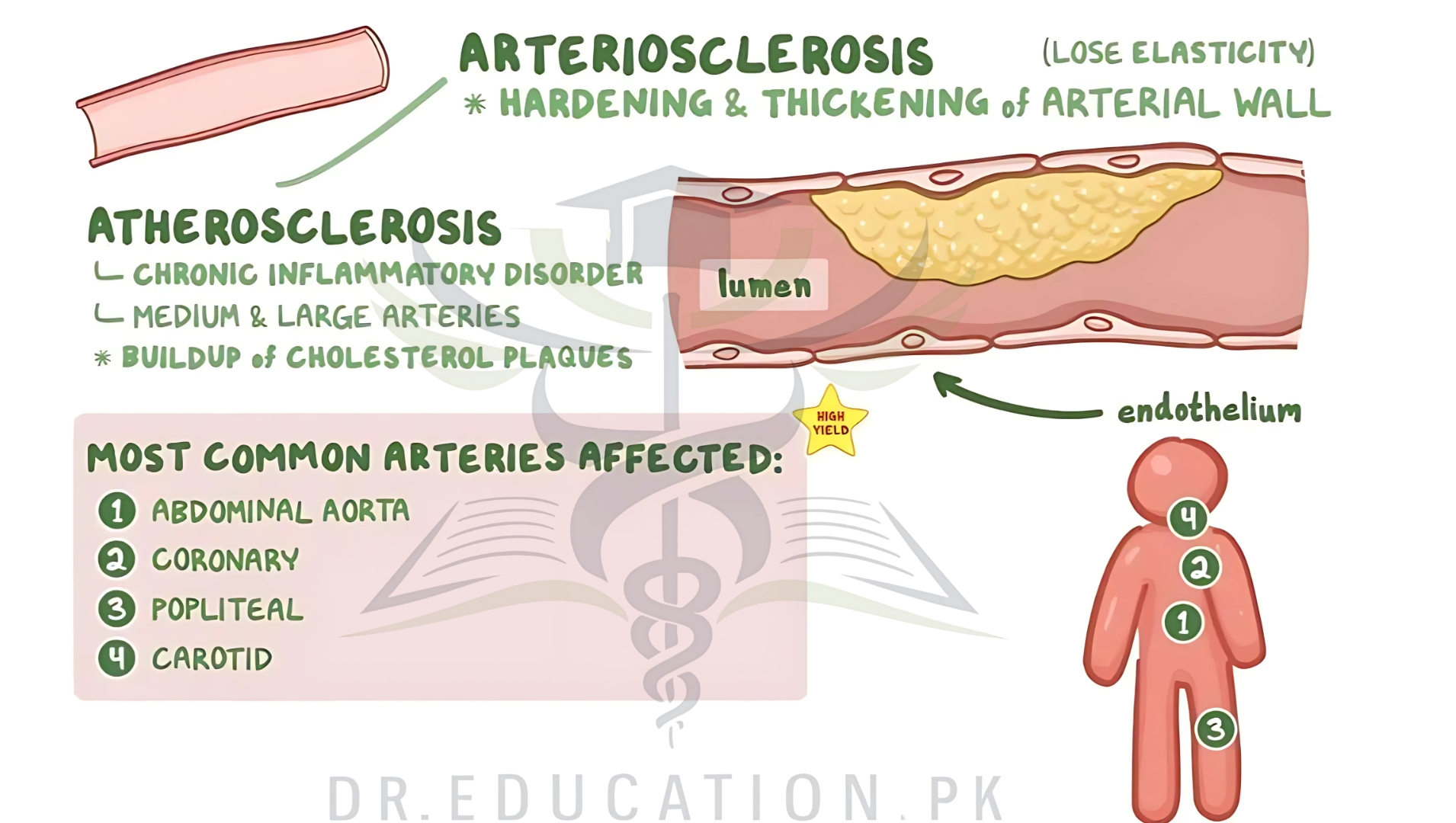
Atherosclerosis
According to Wikipedia,
Atherosclerosis is a pattern of the disease arteriosclerosis, characterized by development of abnormalities called lesions in walls of arteries. This is a chronic inflammatory disease involving many different cell types, and driven by elevated levels of cholesterol in the blood. These lesions may lead to narrowing of the arterial walls due to buildup of atheromatous plaques. At onset there are usually no symptoms, but if they develop, symptoms generally begin around middle age. In severe cases, it can result in coronary artery disease, stroke, peripheral artery disease, or kidney disorders, depending on which body part(s) the affected arteries are located in the body.
Overview
What Is Atherosclerosis?
Atherosclerosis is when plaque — a sticky substance made of cholesterol, fat, calcium, and other materials — builds up inside the walls of your arteries. Arteries are the blood vessels that carry blood from your heart throughout your body.
Atherosclerosis can put blood flow at risk as your arteries become blocked, and it can cause clots to form. It’s the usual cause of heart attacks, strokes, and peripheral artery disease (PAD) — which together are called cardiovascular disease.
The condition doesn’t just affect blood vessels in your heart. It can happen in any of your body’s arteries. But it most often appears in the major arteries that supply blood to your heart, brain, stomach, lower body, and kidneys. You can both prevent and treat this process.
Arteriosclerosis. The names are similar, but atherosclerosis isn’t exactly the same as arteriosclerosis. Arteriosclerosis is a stiffening and thickening of blood vessels that can restrict blood flow to the heart and other organs. It’s sometimes called hardening of the arteries. Atherosclerosis is a type of arteriosclerosis.
How common is atherosclerosis?
Atherosclerosis is very common. The complications of plaque buildup (including heart attacks and strokes) are the leading cause of death worldwide.
In America, about half of people age 45 to 84 have atherosclerosis but aren’t aware of it, according to the U.S. National Institutes of Health.
Stages of Atherosclerosis
When “bad” (LDL) cholesterol in your blood crosses a damaged endothelium, it enters the wall of your artery. Your white blood cells stream in to digest the LDL. Over the years, cholesterol and cells become plaque in the artery wall.
This plaque creates a bump on your artery wall. As atherosclerosis gets worse, the bump gets bigger. When it gets big enough, it can create a blockage.
That slow and gradual process goes on throughout your entire body. Atherosclerosis usually doesn’t cause symptoms until you’re middle-aged or older.
Plaques from atherosclerosis can behave in different ways.
They can stay in your artery wall. There, the plaque grows to a certain size and then stops. Since this plaque doesn’t block blood flow, it may never cause symptoms.
Plaque can grow in a slow, controlled way into the path of blood flow. Over time, it causes significant blockages. Pain in your chest or legs when you exert yourself is the usual symptom.
They can suddenly rupture. This allows blood to clot inside an artery. In your brain, this causes a stroke; in your heart, a heart attack.
The process of atherosclerosis begins with:
Fatty streak. A yellow strip lining the walls of major arteries, fatty streak has been found in children as young as 10. In the fatty streak stage, you feel no symptoms.
Fibrous plaque. The second and more dangerous phase of atherosclerosis begins when the cholesterol-containing plaque expands into blood vessels — the bump.

Complicated lesion. In the last and most serious stage of atherosclerosis, the plaque begins to break up. This exposes the cholesterol and tissue beneath it, causing unseen but serious harm that your immune system tries to fight off. Blood clotting cells, which block blood flow, are formed in response. The blood clots, combined with the exposed plaque, create what’s called a complicated lesion.
Causes of Atherosclerosis
Doctors don’t know exactly how atherosclerosis starts. But it’s believed to begin when the endothelium, the thin layer of cells that lines your arteries, somehow gets damaged. It’s a progressive disease that can begin in childhood.
Common causes of damage to the endothelium include:
- High cholesterol
- High blood pressure
- Inflammation, like from arthritis or lupus
- Obesity or diabetes
- Smoking

What are the symptoms?
Atherosclerosis symptoms often don’t start until an artery is very narrow or blocked. Many people don’t know they have plaque buildup until they have a medical emergency like a heart attack or stroke.
You may notice symptoms of atherosclerosis if your artery is more than 70% blocked. You can have symptoms in different parts of your body, depending on the location of the blockage. Affected locations may include:
Heart
Coronary artery disease (CAD, which can lead to a heart attack) happens in the arteries that supply blood to your heart.
You may experience:
- Shortness of breath (dyspnea) during light physical activity.
- Chest pain or discomfort (angina).
- Pain in your back, shoulders, neck, arms or belly.
- Feeling dizzy or lightheaded.
- Heart palpitations.
- Fatigue.
- Nausea or vomiting that may feel like indigestion.
Digestive system
Mesenteric ischemia happens when you don’t have enough blood flow in parts of your digestive system. You may experience:
- Pain or cramping in your belly (abdomen) after eating.
- Bloating, nausea and vomiting.
- Diarrhea.
- Unintentional weight loss due to “food fear” (fear of pain after eating).
Legs and feet
Peripheral artery disease (PAD) refers to poor blood flow in the arteries in your limbs.
You may experience:
- Muscle pain (intermittent claudication).
- Burning or aching pain in your feet and toes when you rest, especially when lying flat.
- Changes in skin color (like redness).
- Cool skin on your feet.
- Frequent skin and soft tissue infections, often in your legs or feet.
- Sores on your feet or toes that don’t heal.
Kidneys
With renal artery stenosis (narrowing of the arteries that take blood to your kidneys), you may experience:
- Markedly elevated blood pressure that doesn’t respond to multiple medications.
- Changes in how often you pee.
- Swelling (edema).
- Feeling drowsy or tired.
- Skin that feels dry, itchy or numb.
- Headaches.
- Unexplained weight loss.
- Nausea, vomiting or loss of appetite.
With carotid artery disease, the first symptoms are usually a transient ischemic attack (TIA) or stroke.
You may experience:
- Dizziness.
- Drooping on one side of your face.
- Loss of feeling, loss of muscle strength or weakness on one side of your body.
- Severe headache.
- Slurred speech or difficulty forming words.
- Vision loss in one eye. You may notice a dark shade coming down over your field of sight.
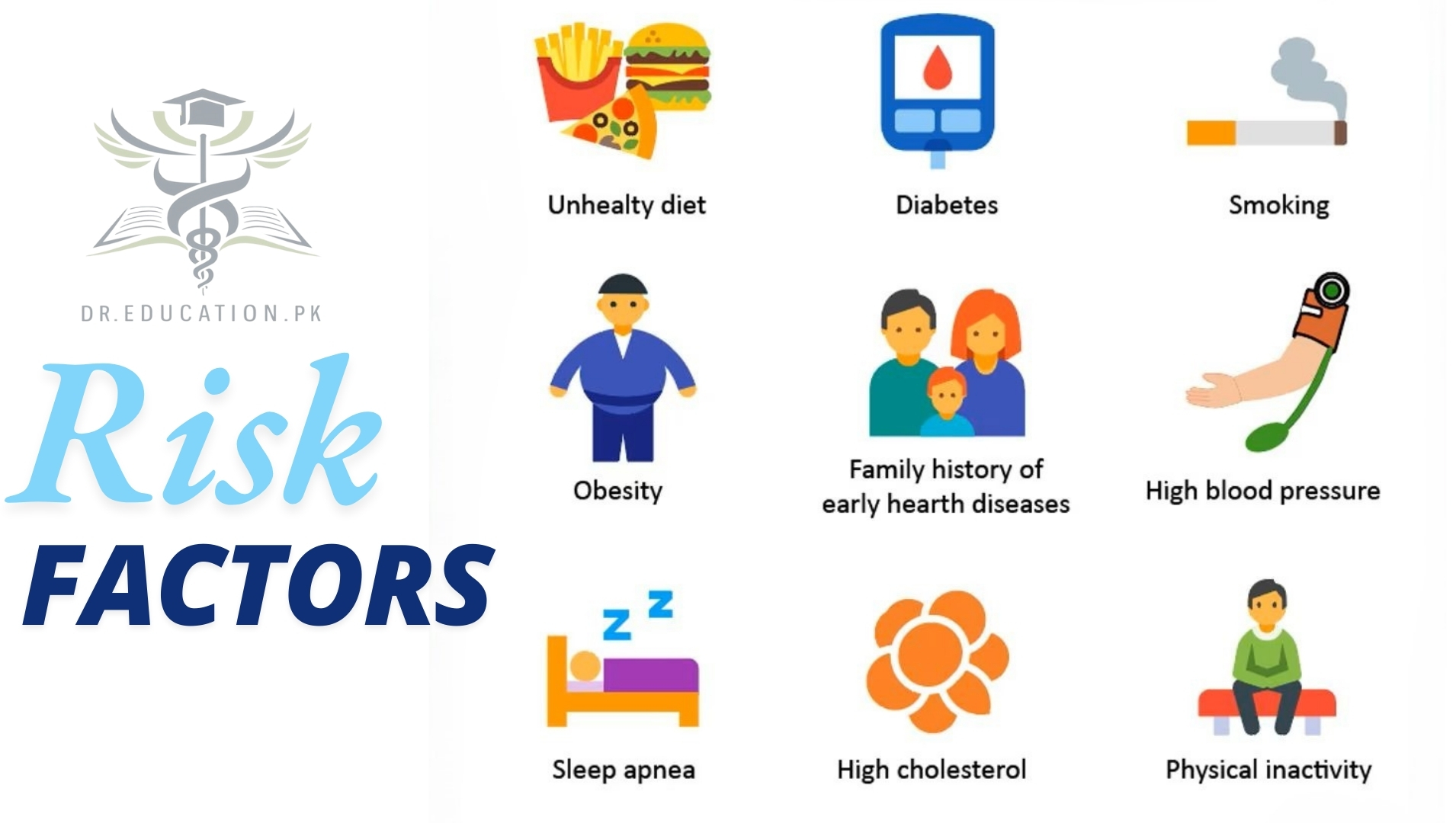
What are the risk factors for atherosclerosis?
Risk factors for atherosclerosis, include:
- High cholesterol and triglyceride levels
- High blood pressure
- Smoking
- Type 1 diabetes
- Obesity
- Physical inactivity
- High saturated fat diet
Complications of Atherosclerosis
Complications of atherosclerosis include:
- Aneurysms
- Angina
- Chronic kidney disease
- Coronary or carotid heart disease
- Heart attack
- Heart failure
- Peripheral artery disease
- Stroke
- Unusual heart rhythms
The plaques of atherosclerosis cause the three main kinds of cardiovascular disease:
- Coronary artery disease: Stable plaques in your heart’s arteries cause angina (chest pain). Sudden plaque rupture and clotting cause heart muscle to die. This is a heart attack.
- Cerebrovascular disease: Ruptured plaques in your brain’s arteries cause strokes with the potential for permanent brain damage. Temporary blockages in your artery can also cause something called transient ischemic attacks (TIAs), which are warning signs of a stroke. They don’t cause any brain injury.
- Peripheral artery disease: When the arteries in your legs narrow, it can lead to poor circulation. This makes it painful for you to walk. Wounds also won’t heal as well. If you have a severe form of the disease, you might need to have a limb removed (amputation).
How is atherosclerosis diagnosed?
First, your doctor will do a complete medical history and physical exam. You may also have one or more of these tests:
- Cardiac catheterization. With this procedure, a long thin tube (catheter) is passed into the coronary arteries. X-rays are taken after a dye is injected into an artery to locate the narrowing, blockages, and other abnormalities of specific arteries.
- Doppler sonography. A special probe is used to direct sound waves into a blood vessel to evaluate blood flow. An audio receiver amplifies the sound of the blood moving though the vessel. Faintness or absence of sound may mean there is a blockage. This is used to identify narrowing of the blood vessels of the abdomen, neck, or legs.
- Blood pressure comparison. Comparing blood pressure measurements in the ankles and in the arms helps determine any constriction in blood flow. Significant differences may mean blood vessels are narrowed due to atherosclerosis.
- MUGA/radionuclide angiography. This is a nuclear scan to see how the heart wall moves and how much blood is expelled with each heartbeat, while the person is at rest.
- Thallium/myocardial perfusion scan. This is a nuclear scan given while the person is at rest or after exercise that may reveal areas of the heart muscle that are not getting enough blood.
- Computerized tomography or CT. This is a type of X-ray test that can see if there is coronary calcification that may suggest a future heart problem.
Management and Treatment
How is atherosclerosis treated?
Atherosclerosis treatment includes lifestyle changes, medications, procedures or surgeries. Depending on the location of your atherosclerosis, you may see a cardiologist (heart), nephrologist (kidneys), neurologist (brain and spine) or vascular surgeon (blood vessels).
Your healthcare providers will develop a plan based on your needs. Common treatment goals include:
- Lowering your risk of blood clots.
- Preventing complications like a heart attack or stroke.
- Easing symptoms.
- Helping you develop patterns of eating that support your heart and blood vessels.
- Slowing or stopping plaque buildup in your arteries.
- Improving blood flow by widening your arteries or bypassing (avoiding) blockages.
Lifestyle changes
Lifestyle changes may lower your risk of complications. Your provider will create a plan specific to your needs. General tips include:
- Avoid all tobacco products (including smoking and vaping).
- Follow a heart-healthy eating plan like the Mediterranean Diet.
- Build physical activity into your daily routine.

Medications
Medications target risk factors for plaque buildup and may help slow the progression of atherosclerosis. Your provider may prescribe medications that lower your blood pressure or cholesterol, manage your blood sugar levels and prevent blood clots.
Procedures or surgeries
Various minimally invasive procedures and complex surgeries can help people with severe blockages or a high risk of complications. Common treatment options include:
- Angioplasty.
- Atherectomy.
- Carotid endarterectomy.
- Coronary artery bypass grafting (CABG).
- Peripheral artery bypass.
- Stent placement.
- Vascular disease bypass.
Atherosclerosis Prevention
You can make changes to your lifestyle to prevent atherosclerosis or slow down its progression. Some things that may help:
- Lower your stress through yoga, mindfulness, or deep breathing. These practices can help lower your blood pressure too.
- Stop smoking (and vaping), which raises your risk for heart disease. Nicotine narrows blood vessels, forcing your heart to work harder. Quitting smoking is one of the most important lifestyle changes you can make to prevent damage to your heart from atherosclerosis.
- Follow a healthy diet rich in low-fat proteins, fish, fruits, vegetables, and whole grains. This will help you manage your weight and lower cholesterol, blood pressure, and blood sugar levels.
- Lose weight and keep it off. Even a small amount will help lower your risk.
- Exercise regularly to maintain a healthy blood pressure and improve blood flow. Aim for at least 150 minutes of moderate exercise or 75 minutes of brisk exercise a week.
- Keep on top of your other health conditions by having regular checkups and following your doctor’s treatment plan.
Conclusion from Dreducation.pk
In conclusion, atherosclerosis is a progressive and often silent disease that can have severe consequences, including heart attacks, strokes, and peripheral artery disease. The condition develops over time as plaque builds up in the arteries, gradually narrowing them and restricting blood flow.
Although symptoms may not appear until the disease is advanced, early diagnosis and intervention are crucial for preventing complications. By adopting a heart-healthy lifestyle—such as maintaining a balanced diet, regular exercise, quitting smoking, and managing chronic conditions like high blood pressure or diabetes—individuals can significantly reduce their risk of developing atherosclerosis or slow its progression.
Early medical intervention, medications, and in some cases, surgery, can help manage the disease and improve outcomes. Regular check-ups and awareness of risk factors are essential to protect against this potentially life-threatening condition.
READ BOOKS
Atherosclerosis
FAQs
What is atherosclerosis?
Atherosclerosis is a condition where plaque, made up of cholesterol, fat, and other substances, builds up in the walls of arteries, causing them to narrow and restrict blood flow.
What causes atherosclerosis?
Atherosclerosis is caused by damage to the artery walls, often due to high cholesterol, high blood pressure, smoking, diabetes, or inflammation.
What are the early signs of atherosclerosis?
In the early stages, atherosclerosis often has no symptoms, but as the condition progresses, it may cause chest pain, shortness of breath, or leg pain during exertion.
How does high cholesterol contribute to atherosclerosis?
High cholesterol, especially LDL (bad cholesterol), contributes to plaque formation in the arteries, which can narrow the vessels and restrict blood flow.
What are the main risk factors for atherosclerosis?
Risk factors include high cholesterol, high blood pressure, smoking, diabetes, obesity, poor diet, and a sedentary lifestyle.
Can atherosclerosis affect any part of the body?
Yes, atherosclerosis can affect any artery in the body, including those in the heart, brain, legs, kidneys, and other organs.
What is the difference between atherosclerosis and arteriosclerosis?
Atherosclerosis is a type of arteriosclerosis where plaque builds up inside the arteries. Arteriosclerosis refers more broadly to the stiffening or thickening of artery walls.
What are the symptoms of advanced atherosclerosis?
Symptoms of advanced atherosclerosis can include chest pain (angina), shortness of breath, leg pain while walking, fatigue, and in severe cases, heart attack or stroke.
How is atherosclerosis diagnosed?
Atherosclerosis is diagnosed through physical exams, blood tests, imaging techniques like Doppler ultrasound, CT scans, or angiography, and sometimes stress tests.
What are the stages of atherosclerosis?
Atherosclerosis progresses through three stages: fatty streaks, fibrous plaque formation, and complicated lesions, where plaques rupture and cause blood clots.
How can atherosclerosis lead to a heart attack?
If plaque in the coronary arteries ruptures, it can form a blood clot that blocks the flow of blood to the heart muscle, causing a heart attack.
What lifestyle changes can help prevent atherosclerosis?
Preventive lifestyle changes include eating a heart-healthy diet, exercising regularly, quitting smoking, maintaining a healthy weight, and managing conditions like high blood pressure and diabetes.
What role does inflammation play in atherosclerosis?
Inflammation can damage the endothelium (artery lining), making it easier for cholesterol to enter and form plaques, which contributes to the development of atherosclerosis.
Can atherosclerosis be reversed?
While atherosclerosis cannot typically be reversed, its progression can be slowed or managed through lifestyle changes, medications, and, in some cases, medical procedures.
What medications are used to treat atherosclerosis?
Common medications for atherosclerosis include statins to lower cholesterol, blood pressure medications, antiplatelets to prevent blood clots, and sometimes anticoagulants.
What surgical treatments are available for severe atherosclerosis?
Surgical treatments for severe atherosclerosis include angioplasty, stent placement, coronary artery bypass grafting (CABG), and carotid endarterectomy.
How does smoking affect atherosclerosis?
Smoking accelerates atherosclerosis by damaging the artery walls, increasing blood pressure, and promoting plaque buildup, making it a major risk factor for heart disease.
What role does diet play in managing atherosclerosis?
A heart-healthy diet rich in fruits, vegetables, whole grains, and lean proteins, while low in saturated fats, cholesterol, and sodium, can help manage atherosclerosis and reduce plaque buildup.
Can exercise help prevent atherosclerosis?
Yes, regular physical activity helps lower blood pressure, reduce cholesterol levels, improve blood circulation, and maintain a healthy weight, all of which reduce the risk of atherosclerosis.
Why is high blood pressure dangerous in atherosclerosis?
High blood pressure damages the arteries, making them more prone to plaque buildup, which increases the risk of heart attacks, strokes, and other complications related to atherosclerosis.