Heart Murmur- Causes, Symptoms & Treatment

What is Heart Murmur?
Heart murmurs are unique heart sounds produced when blood flows across a heart valve or blood vessel. This occurs when turbulent blood flow creates a sound loud enough to hear with a stethoscope. The sound differs from normal heart sounds by their characteristics. For example, heart murmurs may have a distinct pitch, duration and timing.
Overview
What is a heart murmur?
A heart murmur is an extra, unusual sound in your heartbeat. It can sound like a whooshing or swishing noise. The extra noise happens when your blood doesn’t flow smoothly through your heart.
Your doctor can hear the sounds your heart makes through a stethoscope. They will listen to the blood flowing through your heart, and your heart valves opening and closing.
Types of heart murmur
Heart murmurs are sounds produced by turbulent blood flow within the heart, which can be innocent (harmless) or pathological (indicating underlying heart conditions). Here are the main types of heart murmurs:
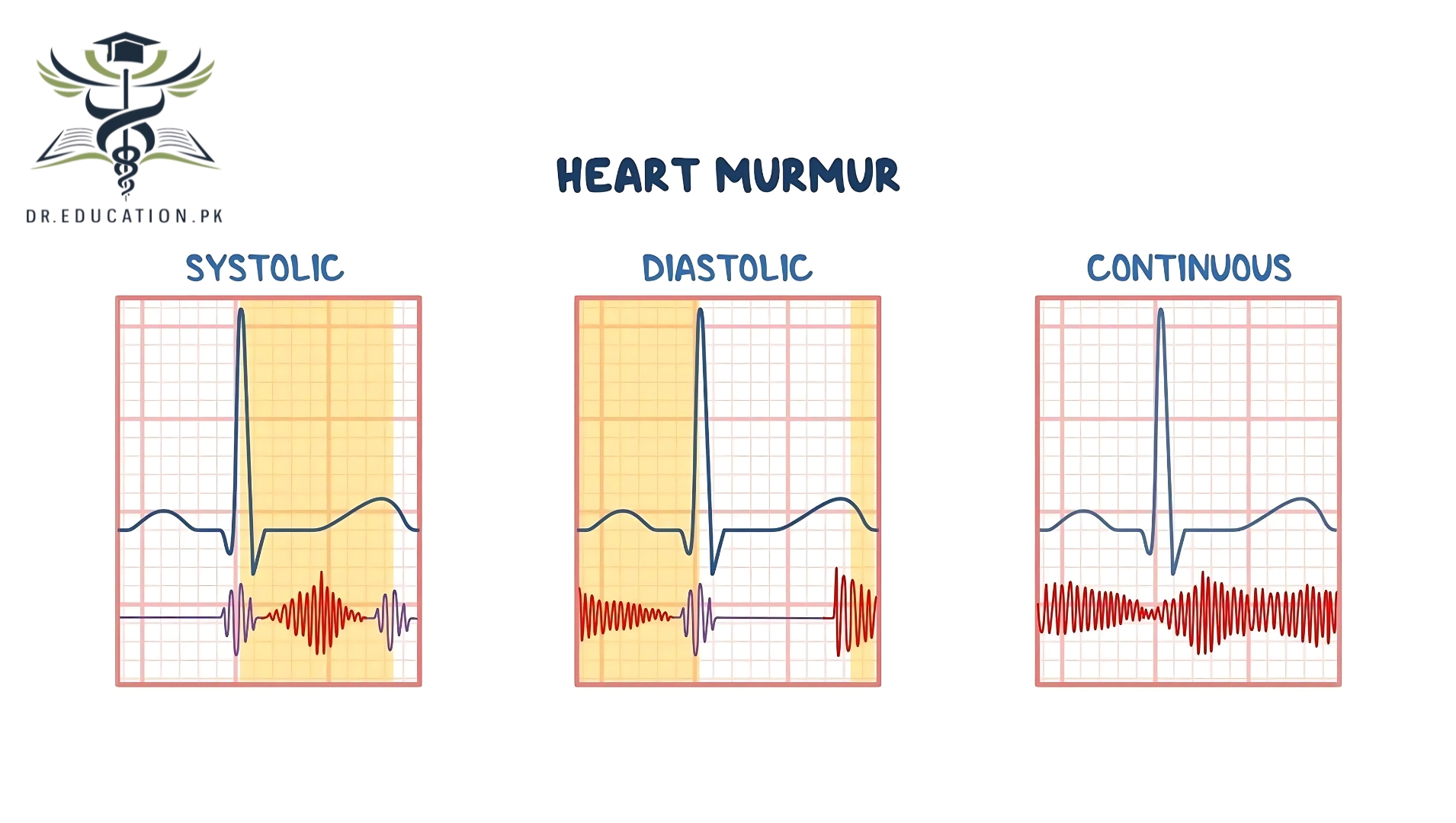
1. Systolic Murmurs
These occur during the heart’s contraction (systole).
- Aortic Stenosis: Caused by narrowing of the aortic valve, it produces a crescendo-decrescendo (diamond-shaped) murmur.
- Mitral Regurgitation: Results from a leaky mitral valve, creating a holosystolic murmur (heard throughout systole).
- Pulmonary Stenosis: Narrowing of the pulmonary valve, which produces a crescendo-decrescendo systolic murmur.
- Tricuspid Regurgitation: Backflow of blood from the right ventricle into the right atrium, causing a holosystolic murmur.
- Ventricular Septal Defect (VSD): A hole between the ventricles causes a harsh holosystolic murmur.
2. Diastolic Murmurs
These occur during the heart’s relaxation (diastole).
- Aortic Regurgitation: Backflow of blood from the aorta into the left ventricle, producing an early decrescendo diastolic murmur.
- Mitral Stenosis: Narrowing of the mitral valve, leading to a low-pitched rumbling murmur, often with an opening snap.
- Pulmonary Regurgitation: Backflow of blood into the right ventricle from the pulmonary artery, causing a decrescendo diastolic murmur.
- Tricuspid Stenosis: Narrowing of the tricuspid valve, producing a rumbling murmur in diastole.
3. Continuous Murmurs
These are heard throughout both systole and diastole.
- Patent Ductus Arteriosus (PDA): A persistent connection between the aorta and the pulmonary artery causes a continuous “machinery-like” murmur.
- Arteriovenous Fistula: An abnormal connection between an artery and a vein, producing continuous murmurs.
4. Innocent (Physiologic) Murmurs
- Still’s Murmur: A common benign murmur in children, often heard at the lower left sternal border.
- Flow Murmurs: Due to increased blood flow across normal valves (e.g., during pregnancy or fever), these murmurs are typically soft and not associated with heart disease.
Also Read:
What is Heart?-Functions & Anatomy.
Symptoms of Heart Murmur
Symptoms that can be associated with heart murmurs include:
- shortness of breath (either when exercising or at rest)
- light-headedness or dizziness
- blackouts
- rapid or irregular heart beat, or heart palpitations
- chest pain
- fatigue (tiredness)
- swelling of the feet and/or legs
- difficulty doing normal daily activities
Babies or children with a heart murmur due to a heart problem may also have:
- a bluish tinge on the skin around their lips or under the fingernails
- poor growth
- pale skin
Babies might have difficulty feeding. This includes getting sweaty when feeding.
Causes
The causes of heart murmurs vary depending on whether the murmur is innocent (harmless) or pathological (due to an underlying condition). Below are the common causes for both types:
Innocent (Physiologic) Murmurs
These murmurs are not associated with structural heart abnormalities and are generally benign. They can occur when blood flows more rapidly than usual through the heart.
Common Causes:
- Increased Blood Flow (Hyperdynamic Circulation):
- Pregnancy: Increased blood volume and cardiac output.
- Fever: Elevated heart rate increases blood flow.
- Exercise: Temporary increase in cardiac output.
- Anemia: The heart works harder to compensate for reduced oxygen-carrying capacity.
- Hyperthyroidism: Increased metabolism leads to increased heart rate and blood flow.
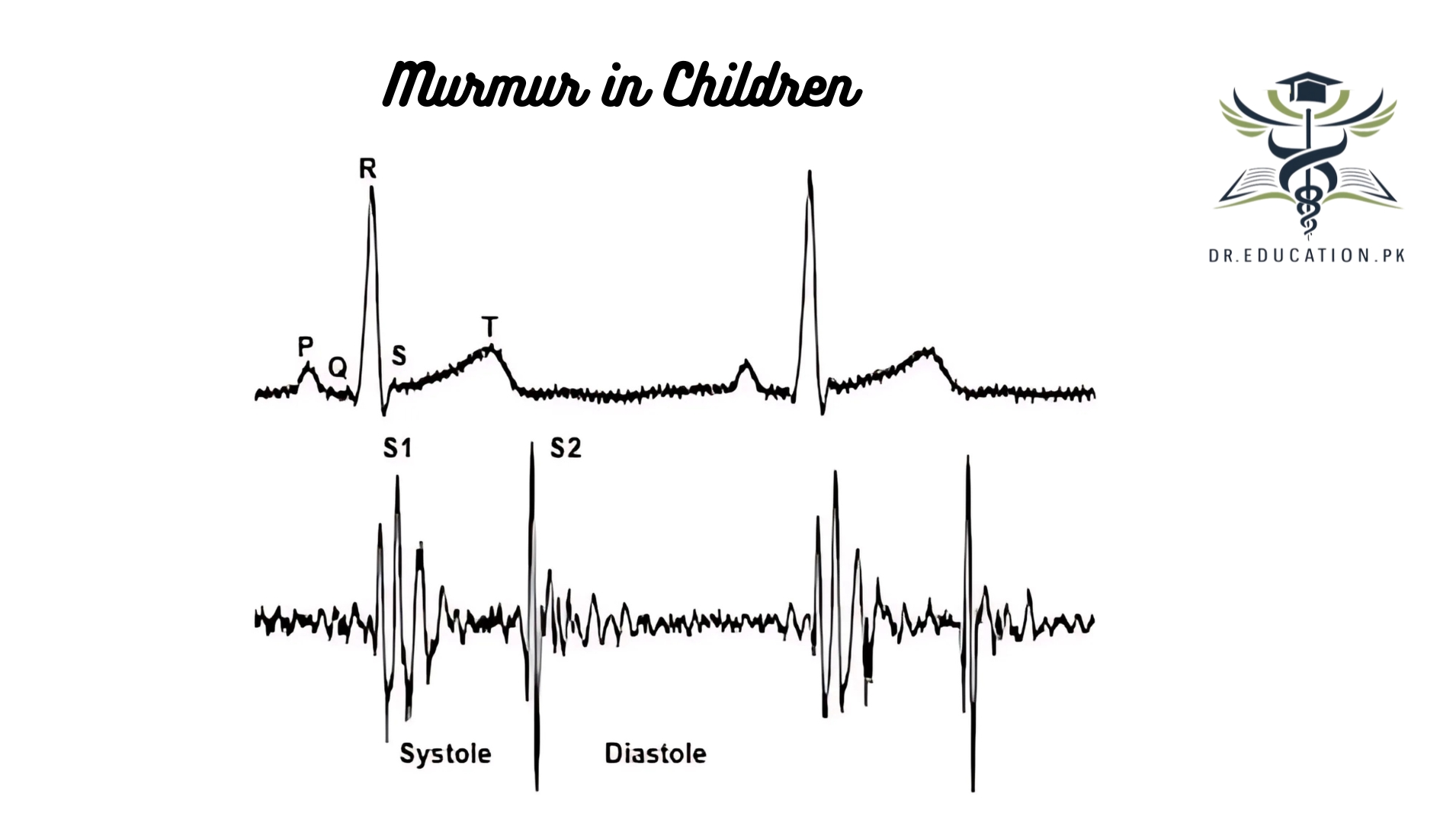
- Childhood Growth: Innocent murmurs are more common in children due to the high velocity of blood flow through smaller cardiac structures.
Pathological Murmurs
These murmurs are caused by structural heart problems and indicate an underlying cardiac condition.
1. Valve Abnormalities
- Aortic Stenosis: Narrowing of the aortic valve, which impedes blood flow from the left ventricle to the aorta.
- Mitral Regurgitation: Incomplete closure of the mitral valve, leading to backflow of blood into the left atrium.
- Pulmonary Stenosis: Narrowing of the pulmonary valve, obstructing blood flow from the right ventricle to the pulmonary artery.
- Tricuspid Regurgitation: Backflow of blood from the right ventricle to the right atrium due to improper valve closure.
- Mitral Stenosis: Narrowing of the mitral valve, restricting blood flow from the left atrium to the left ventricle.
- Aortic Regurgitation: Backflow of blood into the left ventricle due to a leaky aortic valve.
2. Congenital Heart Defects
- Ventricular Septal Defect (VSD): A hole between the ventricles allowing blood to flow between them abnormally.
- Atrial Septal Defect (ASD): A hole between the atria causing abnormal blood flow.
- Patent Ductus Arteriosus (PDA): Persistence of a fetal connection between the aorta and pulmonary artery.
- Tetralogy of Fallot: A combination of four congenital defects, often leading to a significant murmur.
3. Infectious or Inflammatory Conditions
- Rheumatic Fever: Can cause valve damage, particularly affecting the mitral valve, leading to stenosis or regurgitation.
- Endocarditis: Infection of the heart valves, leading to damage and leakage.
4. Cardiomyopathy
- Hypertrophic Cardiomyopathy (HCM): Thickening of the heart muscle can obstruct blood flow, leading to a murmur.
- Dilated Cardiomyopathy: Enlargement of the heart chambers can result in valve regurgitation and a murmur.
5. Aging-Related Changes
- Calcification of Valves: With age, valves (especially the aortic and mitral valves) can become stiff and calcified, leading to stenosis or regurgitation.
- Degenerative Valve Disease: Wear and tear on heart valves over time can cause malfunction.
6. Other Causes
- High Blood Pressure (Hypertension): Chronic hypertension can lead to left ventricular hypertrophy, which may result in a murmur.
- Pulmonary Hypertension: Increased pressure in the pulmonary arteries can cause murmurs due to strain on the right heart.
Diagnosis
Heart murmurs may be detected when a physical exam is done for another reason. You’ll be asked questions about your personal and family medical history.
A health care provider can listen to the heart using a device called a stethoscope. The provider considers several things when listening to the heart to tell if a murmur is innocent or worrisome. Some of those things are:
- Volume. How loud is the heart murmur on a scale from 1 to 6? The loudest heart murmur is 6.
- Location. Where in the heart is it? Does the sound spread to the neck or back?
- Pitch. Is it high-, medium- or low-pitched?
- Timing of the murmur. A murmur that occurs when blood leaves the heart (systolic murmur) generally is an innocent heart murmur. One that happens when the heart fills with blood (diastolic murmur) or throughout the heartbeat (continuous murmur) may signal a heart problem.
- Sound changes. Does exercising or changing body position affect the sound?
Tests
Tests are done to determine the cause of worrisome heart murmurs. Heart murmur tests may include:
- Echocardiogram. This is the main test used to determine the cause of a heart murmur. An echocardiogram uses sound waves to create pictures of the beating heart. It shows how blood flows through the heart and heart valves.
- Chest X-ray. A chest X-ray is a picture of the heart and lungs. It can tell whether the heart is enlarged. Heart enlargement may cause some heart murmurs.
- Electrocardiogram (ECG or EKG). This quick and painless test measures the electrical activity of the heart. During an electrocardiogram (ECG), sensors (electrodes) are attached to the chest and sometimes to the arms or legs. Wires from the sensors connect to a machine, which prints or displays results. A health care provider can look at the signal patterns for signs of heart problems.
- Cardiac catheterization. This test may be done when other tests haven’t found a cause for the heart murmur. A heart doctor (cardiologist) inserts a flexible tube (catheter) into a blood vessel, usually in the groin or wrist. The catheter is gently guided to the heart. Dye may be injected through the catheter. The dye helps blood vessels show up better on the images made during the test.
Treatment
Treatment for heart murmurs depends on the underlying cause. Innocent (harmless) murmurs usually do not require any treatment, but pathological murmurs resulting from heart conditions may need medical, surgical, or lifestyle interventions. Here’s an overview of the treatment options:
1. Innocent (Physiologic) Murmurs
- No Treatment Needed: Innocent murmurs, especially those in children or during pregnancy, typically don’t require any treatment. They often resolve on their own.
- Monitoring: Regular check-ups to ensure the murmur remains benign.
2. Pathological Murmurs
Treatment for pathological murmurs depends on the underlying heart condition, the severity of symptoms, and the impact on heart function.
A. Medication
Medications may help manage symptoms or prevent complications, especially in cases of valvular disease or heart failure.
- Diuretics: Reduce fluid retention and help decrease the workload on the heart (e.g., in heart failure or regurgitant valve conditions).
- Beta-Blockers: Lower heart rate and blood pressure to reduce strain on the heart (useful in aortic stenosis or hypertrophic cardiomyopathy).
- ACE Inhibitors/ARBs: Help lower blood pressure and prevent heart remodeling, often prescribed for heart failure and regurgitant valve diseases.
- Anticoagulants (Blood Thinners): Used in cases of atrial fibrillation, mechanical heart valves, or other conditions to prevent blood clots.
- Antibiotics: May be necessary before certain procedures (like dental work) in people with damaged or prosthetic heart valves to prevent infective endocarditis.
- Vasodilators: Help open blood vessels and improve blood flow, often used in conditions like mitral regurgitation or aortic regurgitation.
B. Surgical Interventions
Surgery is often necessary when the murmur is caused by structural abnormalities or when medications are no longer effective.
- Valve Repair: Surgeons can repair a damaged valve (e.g., in mitral or tricuspid valve prolapse or stenosis) using techniques like leaflet repair, chordal repair, or valve ring annuloplasty.
- Valve Replacement: In cases of severe valve damage, the valve may be replaced with either a mechanical valve (requires lifelong anticoagulation) or a biological valve (from animal tissue, usually lasts 10-20 years).
- Aortic Valve Replacement: For severe aortic stenosis or regurgitation.
- Mitral Valve Replacement: For severe mitral stenosis or regurgitation.
- Transcatheter Aortic Valve Replacement (TAVR): A minimally invasive procedure used to replace the aortic valve without open-heart surgery, particularly for older or high-risk patients.
- Septal Defect Repair: For conditions like ventricular septal defect (VSD) or atrial septal defect (ASD), surgery is performed to close the hole between the heart chambers.
- Correction of Congenital Defects: In children with conditions like Tetralogy of Fallot or Patent Ductus Arteriosus (PDA), surgery is needed to correct the defect and restore normal blood flow.
C. Other Procedures
- Balloon Valvuloplasty: A minimally invasive procedure to widen a stenotic (narrowed) valve, typically used in aortic or pulmonary stenosis.
- Percutaneous Valve Repair: A catheter-based procedure used to repair certain types of valve problems (e.g., MitraClip for mitral regurgitation).
D. Lifestyle Changes
- Regular Monitoring: People with mild to moderate valve disease may need regular echocardiograms and cardiology visits to monitor their heart function.
- Exercise Restrictions: Depending on the severity of the condition, patients with heart murmurs may need to modify their activity level. High-intensity exercise may be restricted in severe aortic stenosis or hypertrophic cardiomyopathy.
- Diet and Blood Pressure Control: A heart-healthy diet, maintaining a normal weight, and controlling high blood pressure can reduce stress on the heart.
- Avoiding Smoking and Alcohol: Reducing risk factors like smoking and excessive alcohol consumption helps protect heart health.
E. Special Considerations for Pregnancy
- Management During Pregnancy: Some women with valvular heart disease may need closer monitoring during pregnancy, as increased blood volume can exacerbate valve problems. Medications and surgical interventions might be necessary before or during pregnancy.
F. Treatment of Associated Conditions
- Infective Endocarditis Prophylaxis: In people with damaged or prosthetic valves, antibiotics may be needed before certain dental or surgical procedures to prevent infection.
- Heart Failure Management: If the murmur is associated with heart failure, the treatment includes diuretics, beta-blockers, ACE inhibitors, and lifestyle changes.
Summary of Treatment Options:
- Innocent Murmurs: No treatment needed, monitoring.
- Medication: For symptoms, heart failure, and preventing complications.
- Surgery: Valve repair/replacement, septal defect closure, correction of congenital defects.
- Lifestyle Changes: Heart-healthy diet, exercise moderation, regular monitoring.
Treatment will depend on individual factors, such as the type and severity of the murmur, symptoms, and underlying heart condition.
When to see a Doctor?
You should see a doctor if you experience any of the following signs or symptoms, especially if they could indicate a heart murmur that might be due to an underlying heart condition:
1. Unexplained Symptoms of Heart Problems
- Chest pain: Especially during physical activity or stress.
- Shortness of breath: Particularly if it occurs during exertion or when lying flat.
- Fatigue: Unusual tiredness or feeling easily fatigued, especially with activity.
- Palpitations: Feeling like your heart is racing, skipping beats, or beating irregularly.
- Swelling: Swelling in your ankles, feet, or abdomen (edema) could indicate heart failure.
- Syncope (fainting): Unexplained fainting spells, especially if they occur during activity or exertion.
2. Family History of Heart Conditions
If you have a family history of congenital heart defects, valve disease, or other heart conditions, especially if they occurred at a young age, you should be evaluated for a murmur or other cardiac issues.
3. Symptoms in Children
- Poor Growth: If a child isn’t growing or gaining weight as expected.
- Frequent Infections: Repeated respiratory infections (such as pneumonia) in children may indicate a heart issue.
- Difficulty Feeding or Sweating While Feeding: This may be a sign of congenital heart defects.
- Bluish Skin (Cyanosis): Especially around the lips or fingers, which can indicate poor oxygenation.
4. Presence of a New or Worsening Murmur
If you or your doctor detect a new murmur or if an existing murmur changes in intensity or character, further evaluation is needed. This could indicate worsening valve disease or other structural heart problems.
5. Symptoms of Infective Endocarditis
In people with pre-existing valve disease or prosthetic valves, see a doctor if you have:
- Fever or unexplained illness.
- Fatigue or night sweats.
- New murmur or worsening of an existing murmur.
- Unusual skin rashes or spots (petechiae).
6. Pregnancy
If you are pregnant and have a known heart murmur, it’s important to get evaluated, especially if you experience:
- Unusual fatigue.
- Shortness of breath.
- Swelling.
- Dizziness or fainting.
7. Heart Murmur Discovered During a Routine Checkup
If your doctor detects a murmur during a routine exam, they may recommend additional tests like an echocardiogram to determine whether it’s innocent or related to a heart condition.
Conclusion from Dreducation.pk
Heart murmurs, characterized by extra or unusual sounds in the heart due to turbulent blood flow, can be either harmless (innocent) or indicate underlying heart conditions (pathological). While innocent murmurs typically require no treatment, pathological murmurs resulting from structural heart issues like valve abnormalities or congenital defects may necessitate medical or surgical intervention. Recognizing symptoms like shortness of breath, chest pain, or fatigue and seeking timely medical evaluation is crucial, especially for individuals with worsening murmurs or a family history of heart disease. Early diagnosis and appropriate management can prevent complications and improve heart health.