What is Pericardial Effusion?
Pericardial effusion is the presence of an abnormal amount of fluid and/or an abnormal character to fluid in the pericardial space. It can be caused by a variety of local and systemic disorders, or it may be idiopathic.
Overview
What is pericardial effusion?
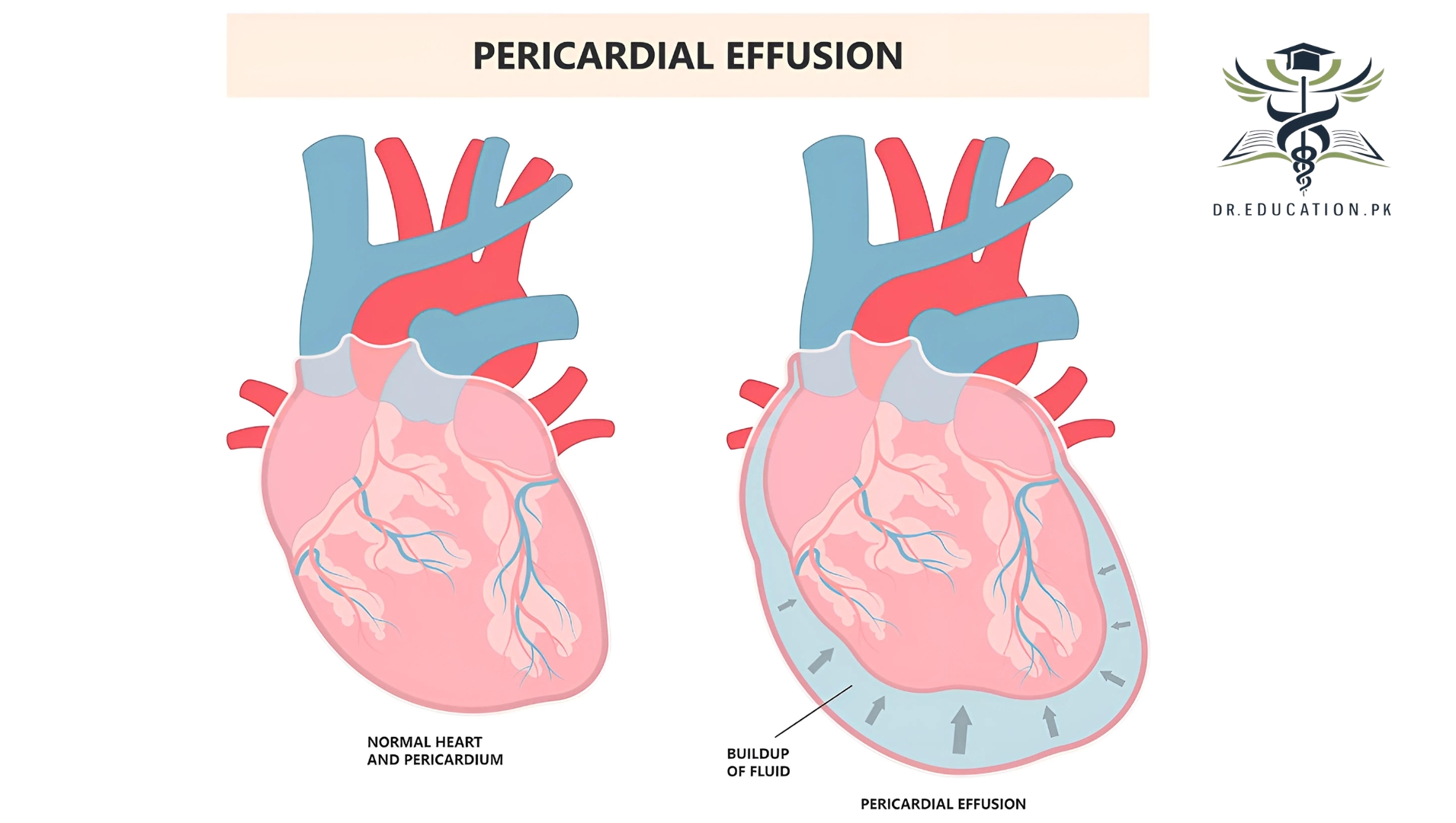
Pericardial effusion is the build-up of extra fluid in the space around the heart. If too much fluid builds up, it can put pressure on the heart. This can prevent it from pumping normally.
A fibrous sac called the pericardium surrounds the heart. This sac consists of two thin layers. Normally, there is a small amount of fluid between them. The fluid reduces friction between the two layers as they rub against each other during each heartbeat. In some cases, extra fluid can build up between these two layers leading to a pericardial effusion.
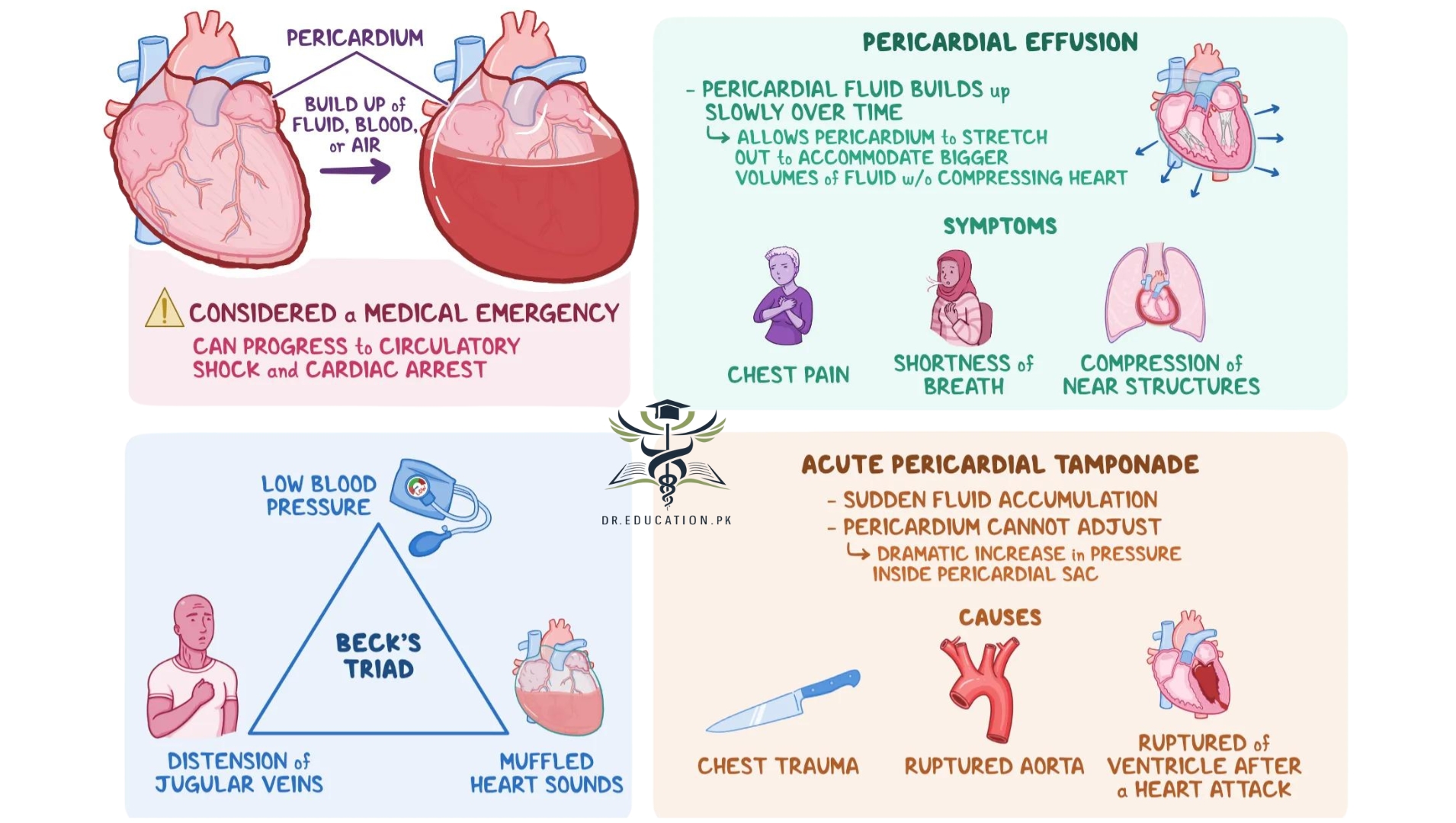
A little fluid won’t cause much of a problem. But if too much fluid builds up, it can make it hard for the heart to expand normally. This condition is called cardiac tamponade. It usually requires emergency treatment. Because the heart can’t expand normally, less blood can enter the heart from the body. This can reduce the amount of oxygenated blood going out to the body. But not all pericardial effusions cause cardiac tamponade.
In some cases, pericardial effusion develops quickly. This is known as acute pericardial effusion. Other times, the fluid builds up slowly. This is known as subacute pericardial effusion. Chronic pericardial effusion occurs when cardiac effusion happens more than once over time.
Cardiac Tamponade vs. Pericardial Effusion
Cardiac tamponade (pronounced tam-puh-naad) happens when so much fluid gathers in your pericardium that it prevents your heart from filling with blood and working properly. Cardiac tamponade is a life-threatening condition, and you need to go to the doctor right away.
Causes
Causes of pericardial effusion include:
- Pericarditis (inflammation of the pericardium).
- Infections, most often caused by viruses (such as HIV) and bacteria (such as tuberculosis), but they can be due to fungus or parasites, too.
- Autoimmune conditions, such as systemic lupus erythematosus (SLS), rheumatoid arthritis, and Sjogren syndrome.
- Hormone disorders or problems, such as severe hypothyroidism, or ovarian hyperstimulation syndrome.
- Trauma or injury to your chest, such as those from a car crash or punctures from knives or bullets.
- Heart problems, such as a heart attack, heart failure, or aortic dissection (where the main blood vessel leading to your heart separates or tears).
- Side effects from medical treatments, such as heart surgery, radiation therapy for cancer, or certain medications.
- Complications from medical conditions, such as chronic kidney disease, kidney failure, or liver cirrhosis.
Symptoms
You may not have any symptoms. This is more often the case with a mild effusion. You might be more likely to have symptoms from whatever is causing the pericardial effusion. For example, you might have fever if you have an infection of the pericardial sac.
When effusion is more severe, you may have symptoms such as:
- Chest pain or discomfort
- Enlargement of the veins of the neck
- Fainting
- Fast breathing
- Increased heart rate
- Nausea
- Pain in the right upper abdomen
- Shortness of breath
- Swelling in the arms and legs
If the effusion is very severe, it can also lead to very low blood pressure. This can cause symptoms of shock. These include:
- Light-headedness or dizziness
- Cool arms and legs
- Clammy skin
- Weakness
- Rapid breathing
- Nausea or vomiting
- Pale skin
- Less urine output
Diagnosis
Pericardial effusion is the accumulation of fluid in the pericardial sac around the heart. Diagnosing pericardial effusion involves clinical evaluation and various diagnostic tools:
1. Clinical Assessment
- History: Look for symptoms like chest pain (worse with inspiration or when lying down), dyspnea, fatigue, palpitations, and light-headedness.
- Physical Examination:
- Muffled heart sounds: Due to the fluid acting as a barrier.
- Pericardial friction rub: A scratching sound heard with auscultation (more common in pericarditis).
- Jugular Venous Distension (JVD): Indicates increased central venous pressure.
- Pulsus paradoxus: A drop in systolic BP (>10 mmHg) during inspiration, indicating cardiac tamponade.
2. Electrocardiogram (ECG)
- Low voltage QRS complexes: Due to electrical dampening by the pericardial fluid.
- Electrical alternans: Varying QRS amplitude due to the heart swinging in the fluid.
3. Chest X-ray
- Enlarged cardiac silhouette: Indicates a significant effusion.
- “Water bottle” heart shape may be observed in large effusions.
4. Echocardiography (ECHO)
- Gold standard for diagnosis.
- Shows the size of the effusion and whether there is any associated cardiac tamponade.
- Can assess hemodynamic impact, such as right atrial or ventricular collapse.
5. Computed Tomography (CT) or Magnetic Resonance Imaging (MRI)
- Useful in cases where echocardiography is inconclusive.
- Provides detailed information about the pericardium and surrounding structures.
6. Pericardiocentesis
- Diagnostic and therapeutic procedure.
- Fluid analysis can help determine the cause (infection, malignancy, etc.).
7. Blood Tests
- May include markers for inflammation (ESR, CRP), infection (e.g., viral serologies), or autoimmune conditions (e.g., ANA for lupus).
Differential Diagnosis
- Cardiac tamponade: When the pericardial effusion compresses the heart, leading to hemodynamic instability.
- Constrictive pericarditis: A chronic condition where the pericardium thickens and stiffens.
Treatment
The treatment of a pericardial effusion depends on its severity and cause.
For a large effusion or cardiac tamponade, the fluid must be drained. This will likely be done through one of the following methods:
Pericardiocentesis to pull the extra fluid out with a needle. If necessary, your doctor may leave a tube in your chest (pericardial drain) for a few days to drain the fluid completely.
Surgery to remove the extra fluid. The type of procedure your doctor uses will depend on what’s causing your effusion, how you are doing physically, and how well your doctors think you will handle the surgery.
This may be done using any of several procedures, such as:
Percutaneous balloon pericardiotomy. Your surgeon will use X-rays to guide them as they insert a long, thin tube with a small balloon on the end into your pericardium. They will make a small hole in it and inflate the balloon to make the hole bigger so that the extra fluid can drain out.
Emergency room thoracotomy. Your doctor may do this procedure if you have cardiac tamponade and pericardiocentesis didn’t work. In this procedure, your chest is opened so that your doctor can get to your heart. They will make a cut in your pericardium and drain the fluid out.Pericardiotomy. During this procedure, your doctor will remove all or part of your pericardium so that no fluid can collect in it. Surgical pericardial window using video-assisted thoracoscopic surgery (VATS). Your doctor will make a small opening (a window) in your pericardium to let the fluid drain out.
Small effusions that don’t have symptoms and are due to known causes (for example, kidney failure) may require no special treatment. Your doctor will likely watch your effusion using an echocardiogram so they can see if it changes size or needs direct treatment.
If your effusion isn’t dangerous and doesn’t need to be drained immediately, your doctor will likely treat the cause. This will also treat the effusion. Such treatments may include:
- Antibiotics, which will treat any bacterial infections, such as tuberculosis
- Anti-inflammatory drugs, which will reduce any inflammation and swelling
- Chemotherapy and radiation therapy if you have cancer
- Diuretics and other medicines if you have heart failure
When to see a Doctor?
You should see a doctor if you experience symptoms that may indicate a pericardial effusion, particularly because it can progress to a life-threatening condition like cardiac tamponade. Here are some key indicators of when to seek medical attention:
1. Emergency Symptoms (Immediate Medical Attention)
- Severe chest pain: Particularly if it’s sharp and worsens with deep breaths or lying down.
- Shortness of breath: Especially if it worsens with exertion or lying flat.
- Fainting or near-fainting: This could indicate reduced cardiac output due to a large effusion or tamponade.
- Rapid heartbeat (palpitations): Especially if accompanied by weakness or dizziness.
- Low blood pressure: Could be a sign of impending cardiac tamponade, requiring urgent medical intervention.
- Swelling in legs or abdomen: This could indicate right-sided heart failure due to pressure on the heart from the effusion.
- Sudden cold sweats, light-headedness, or confusion: Signs of low perfusion, possibly due to cardiac tamponade.
2. Moderate Symptoms (Schedule an Appointment)
- Ongoing chest discomfort or pressure: Not necessarily severe, but persistent.
- Mild to moderate shortness of breath: Especially if it occurs with exertion or worsens over time.
- Fatigue or general malaise: Symptoms of heart failure, which can occur as the heart’s function is compromised by the effusion.
- Swelling of the veins in the neck (jugular venous distension): Could indicate increased pressure inside the heart.
3. Following a Recent Infection or Injury
- If you’ve recently had a viral illness, chest infection, or injury to the chest and start experiencing chest pain or breathing difficulty, you should see a doctor to rule out complications like pericardial effusion.
4. People with Known Heart or Autoimmune Conditions
- If you have a history of pericarditis, autoimmune diseases (e.g., lupus), or other heart conditions, you should see a doctor if any new symptoms arise, as you’re at higher risk of developing pericardial effusion.
What are complications of pericardial effusion?
Many times, there are no complications of pericardial effusion. The most serious possible complication is cardiac tamponade. If untreated, it can lead to shock, which can cause serious complications. For example, reduced blood flow to the kidneys during shock can cause the kidneys to fail. If left untreated, shock can lead multiple organs to fail, causing death. In rare cases, the pericardium can become scarred and prevent the heart from filling correctly.
What can I do to prevent pericardial effusion?
You can reduce your risk of some of the medical problems that can lead to pericardial effusion. For example, take care of your heart by:
- Limiting alcohol.
- Eating a heart-healthy diet.
- Getting enough exercise
- Staying at a healthy weight.
- Seeing a healthcare provider regularly to treat your medical problems.
Conclusion from Dreducation.pk
Pericardial effusion is a potentially serious condition involving the build-up of excess fluid around the heart. While small amounts of fluid may not cause immediate issues, larger effusions can lead to life-threatening complications like cardiac tamponade, which requires urgent medical treatment. The causes of pericardial effusion are varied, ranging from infections and autoimmune diseases to heart conditions and trauma.
Early diagnosis is crucial, often through clinical evaluation, imaging techniques like echocardiography, and sometimes procedures like pericardiocentesis. Depending on the underlying cause and severity, treatment can range from medication to surgical interventions aimed at relieving the pressure on the heart.
Timely medical attention and preventive measures, such as managing underlying conditions and maintaining heart health, are key to avoiding severe outcomes. Recognizing symptoms early and seeking prompt care can greatly improve prognosis and reduce complications associated with pericardial effusion.
READ BOOKS