What is Stroke?
According to Wikipedia,
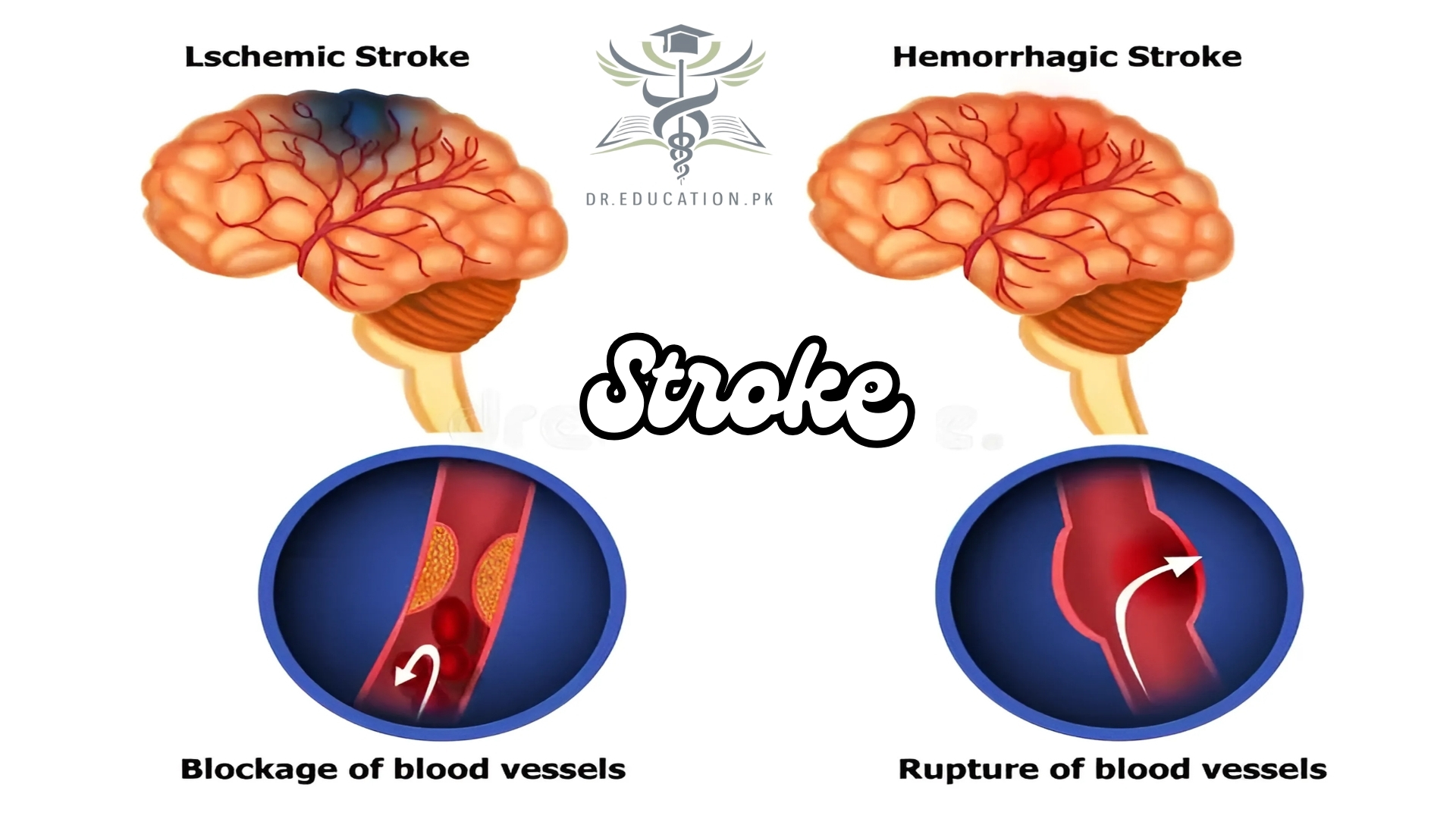
Stroke (also known as a cerebrovascular accident (CVA) or brain attack) is a medical condition in which poor blood flow to the brain causes cell death. There are two main types of stroke:
- ischemic, due to lack of blood flow, and
- hemorrhagic, due to bleeding.
Both cause parts of the brain to stop functioning properly.
Overview
What is Stroke?
A stroke is a life-threatening condition that happens when part of your brain doesn’t have enough blood flow. This most commonly happens because of a blocked artery or bleeding in your brain. Without a steady supply of blood, the brain cells in that area start to die from a lack of oxygen.
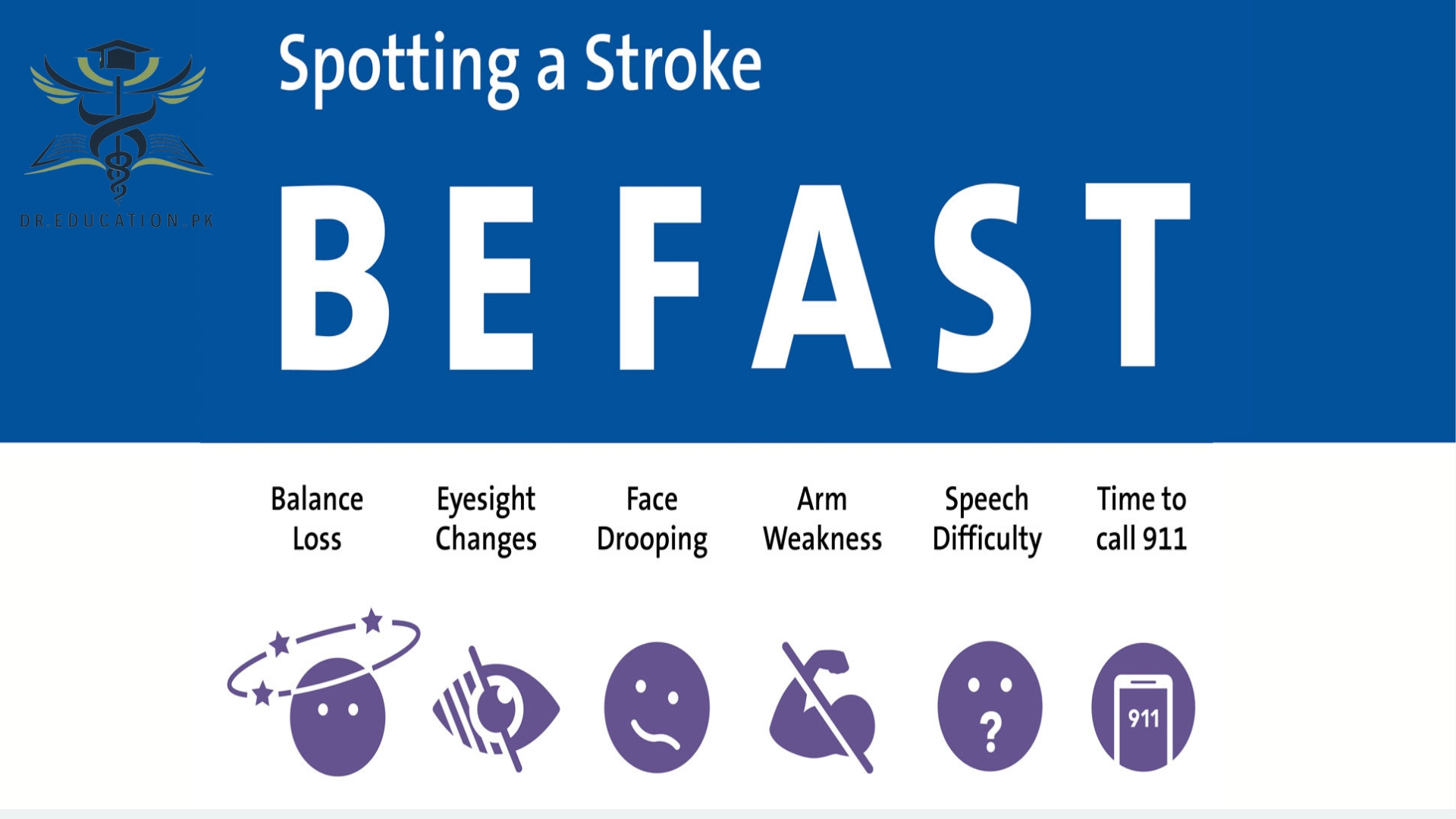
To recognize the warning signs of a stroke, remember to think BE FAST:
| Acronym | Warning Sign | Description |
|---|---|---|
| B | Balance | Be watchful for a sudden loss of balance. |
| E | Eyes | Look out for sudden loss of vision in one or both eyes. Are they experiencing double vision? |
| F | Face | Ask the person to smile. Look for a droop on one or both sides of their face, which is a sign of muscle weakness or paralysis. |
| A | Arms | A person having a stroke often has muscle weakness on one side. Ask them to raise their arms. If they have one-sided weakness (and didn’t have it before), one arm will stay higher while the other will sag and drop downward. |
| S | Speech | Strokes often cause a person to lose their ability to speak. They might slur their speech or have trouble choosing the right words. |
| T | Time | Time is critical, so don’t wait to get help! If possible, look at your watch or a clock and remember when symptoms start. Telling a healthcare provider when symptoms started can help the provider know what treatment options are best. |
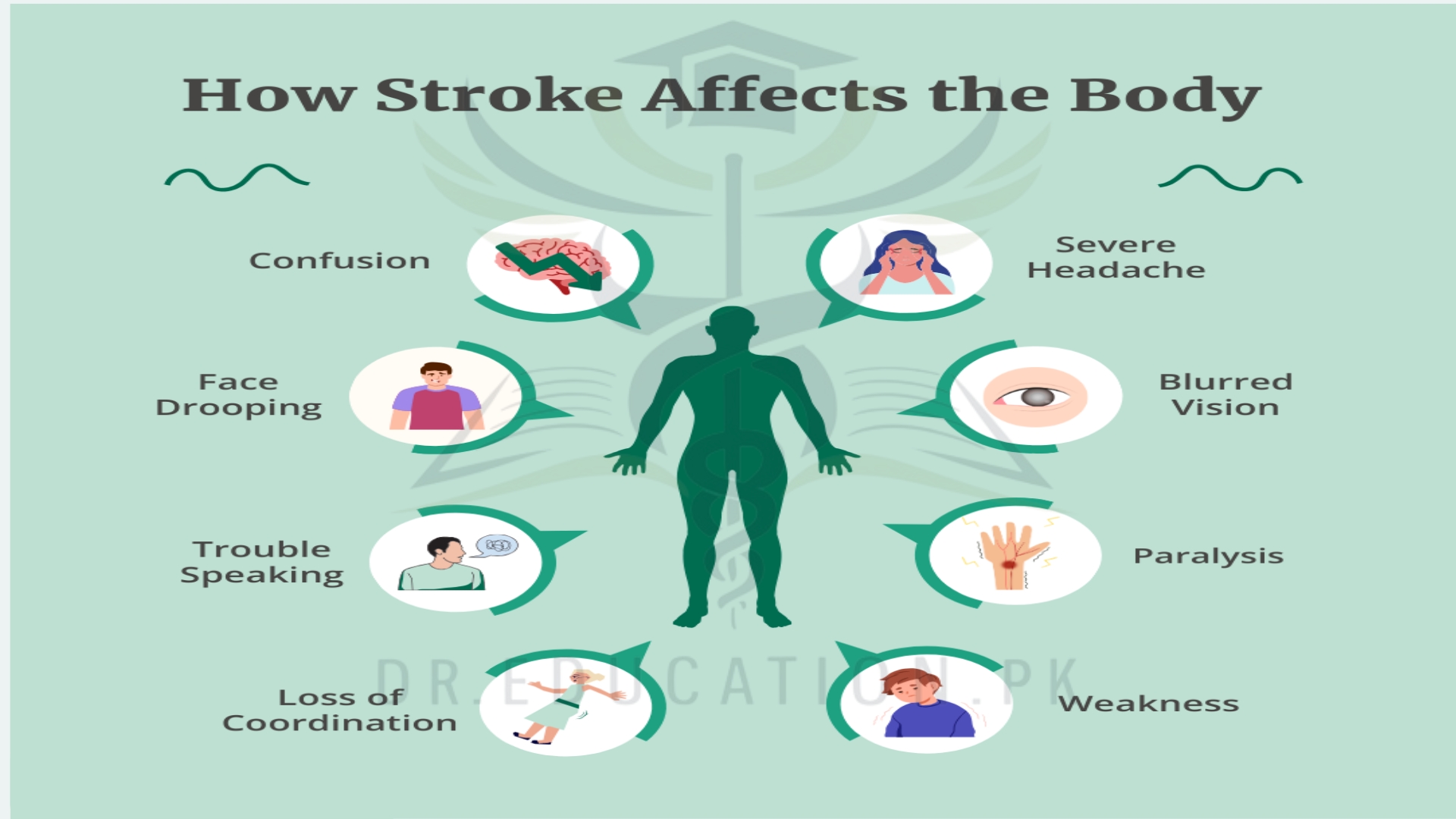
Symptoms of a stroke
The main symptoms of a stroke can happen suddenly. They may include:
- face weakness – one side of your face may droop (fall) and it might be hard to smile
- arm weakness – you may not be able to fully lift both arms and keep them there because of weakness or numbness in 1 arm
- speech problems – you may slur your words or sound confused
The easiest way to remember these symptoms is the word FAST. This stands for: face, arms, speech and time to call.
Other symptoms of a stroke
There are other signs that you or someone else is having a stroke. These include:
- weakness or numbness down 1 side of your body
- blurred vision or loss of sight in 1 or both eyes
- finding it difficult to speak or think of words
- confusion and memory loss
- feeling dizzy or falling over
- a severe headache
Symptoms of a stroke can sometimes stop after a short time, so you may think you’re OK. Even if this happens, get medical help straight away.
A stroke is more likely to happen if you’re older, but it can happen at any age.
How common is a stroke?
Strokes are very common. Worldwide, strokes rank second among the top causes of death. In the United States, stroke is the fifth cause of death. Strokes are also a leading cause of disability worldwide.
How does a stroke affect my body?
Strokes are to your brain what a heart attack is to your heart. When you have a stroke, part of your brain loses its blood supply, which keeps that brain area from getting oxygen. Without oxygen, the affected brain cells become oxygen-starved and stop working properly.
If your brain cells go too long without oxygen, they’ll die. If enough brain cells in an area die, the damage becomes permanent, and you may lose the abilities that area once controlled. However, restoring blood flow may prevent that kind of damage or at least limit how severe it is. That’s why time is critical in treating a stroke.
Who does it affect?
Anybody can have a stroke, from children to adults, but there are some people who have a greater risk than others. Strokes are more common later in life (about two-thirds of strokes happen in people over age 65).
There are also certain medical conditions that increase the risk of stroke, including high blood pressure (hypertension), high cholesterol (hyperlipidemia), Type 2 diabetes, and people who have a history of stroke, heart attack or irregular heart rhythms like atrial fibrillation.
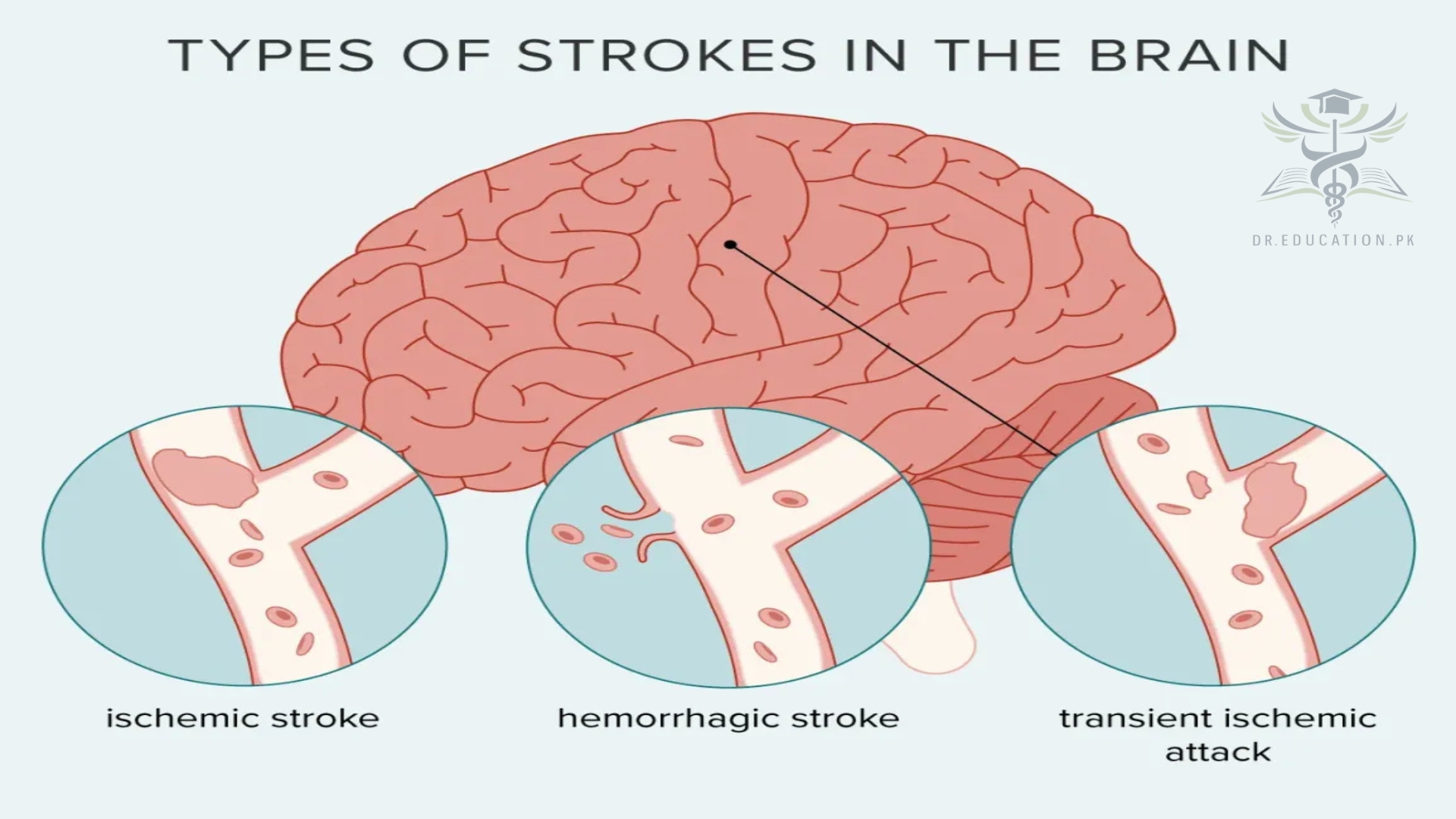
What are the types of stroke?
There are two main ways that strokes can happen: ischemia and hemorrhage.
Ischemic stroke
Ischemia (pronounced “iss-key-me-uh”) is when cells don’t get enough blood flow to supply them with oxygen. This usually happens because something blocks blood vessels in your brain, cutting off blood flow. Ischemic strokes are the most common and account for about 80% of all strokes.
Ischemic strokes usually happen in one of the following ways:
- Formation of a clot in your brain (thrombosis).
- A fragment of a clot that formed elsewhere in your body that breaks free and travels through your blood vessels until it gets stuck in your brain (embolism).
- Small vessel blockage (lacunar stroke), which can happen when you have long-term, untreated high blood pressure (hypertension), high cholesterol (hyperlipidemia) or high blood sugar (Type 2 diabetes).
- Unknown reasons (these are cryptogenic strokes; the word “cryptogenic” means “hidden origin”).
Hemorrhagic stroke
Hemorrhagic (pronounced “hem-or-aj-ick”) strokes cause bleeding in or around your brain. This happens in one of two ways:
- Bleeding inside of your brain (intracerebral). This happens when a blood vessel inside of your brain tears or breaks open, causing bleeding that puts pressure on the surrounding brain tissue.
- Bleeding into the subarachnoid space (the space between your brain and its outer covering). The arachnoid membrane, a thin layer of tissue with a spiderweb-like pattern on it, surrounds your brain. The space between it and your brain is the subarachnoid space (“sub” means “under”). Damage to blood vessels that pass through the arachnoid membrane can cause a subarachnoid hemorrhage, which is bleeding into the subarachnoid space, putting pressure on the brain tissue underneath.
Transient ischemic attack (TIA)
A transient ischemic attack (TIA) — sometimes called a “mini-stroke” — is like a stroke, but the effects are temporary. These are often warning signs that a person has a very high risk of having a true stroke in the near future. Because of that, a person who has a TIA needs emergency medical care as soon as possible.
Causes of a stroke
A stroke can happen to anyone at any age, but your risk may increase if:
- you’re over 50 years old
- you’re from a Black or South Asian background
- you have sickle cell disease (SCD)
- you have an unhealthy lifestyle
- you have migraines
- you take the combined contraceptive pill
- you’re pregnant and have pre-eclampsia
- you’ve just had a baby
Certain conditions also increase the risk of stroke. These include:
- high blood pressure (hypertension)
- diabetes
- irregular and fast heartbeats (atrial fibrillation)
- high cholesterol
- a transient ischaemic attack (TIA or mini stroke)
Risk factors
Many factors can increase the risk of stroke. Potentially treatable stroke risk factors include:
Lifestyle risk factors
- Being overweight or obese.
- Physical inactivity.
- Heavy or binge drinking.
- Use of illegal drugs such as cocaine and methamphetamine.
Medical risk factors
- High blood pressure.
- Cigarette smoking or secondhand smoke exposure.
- High cholesterol.
- Diabetes.
- Obstructive sleep apnea.
- Cardiovascular disease, including heart failure, heart defects, heart infection or irregular heart rhythm, such as atrial fibrillation.
- Personal or family history of stroke, heart attack or transient ischemic attack.
- COVID-19 infection.
Other factors associated with a higher risk of stroke include:
- Age — People age 55 or older have a higher risk of stroke than do younger people.
- Race or ethnicity — African American and Hispanic people have a higher risk of stroke than do people of other races or ethnicities.
- Sex — Men have a higher risk of stroke than do women. Women are usually older when they have strokes, and they’re more likely to die of strokes than are men.
- Hormones — Taking birth control pills or hormone therapies that include estrogen can increase risk.
Diagnosing a stroke
If a doctor thinks you’ve had a stroke, they’ll do tests such as:
- blood tests
- CT, MRI and ultrasound scans to check in and around your brain
- an electrocardiogram (ECG) to check your heart
These tests can show what type of stroke you’ve had. The different types of stroke include:
- an ischaemic stroke – this happens when a blood clot blocks blood flow to the brain. It’s the most common type of stroke
- a haemorrhagic stroke – this happens when a blood vessel bursts
- a transient ischaemic attack (TIA or mini stroke) – this is when the symptoms of a stroke do not last very long (less than 24 hours)
A TIA should be treated as urgent. If you do not get immediate medical attention, you could be at risk of having a full stroke.
Management and Treatment
How are strokes treated?
Treating a stroke depends on many different factors. The most important factor in determining treatment is what kind of stroke a person has.
- Ischemic: With ischemic strokes, the top priority is restoring circulation to affected brain areas. If this happens fast enough, it’s sometimes possible to prevent permanent damage or at least limit a stroke’s severity. Restoring circulation usually involves a certain medication type called thrombolytics, but may also involve a catheterization procedure.
- Hemorrhagic: With hemorrhagic strokes, treatment depends on the location and severity of the bleeding. Reducing blood pressure is often the top priority because this will reduce the amount of bleeding and keep it from getting worse. Another treatment option is to improve clotting so the bleeding will stop. Surgery is sometimes necessary to relieve pressure on your brain from accumulated blood.
What medications or treatments are used?
The medications and treatments used vary depending on the type of stroke and how soon a person receives treatment after the stroke. There are also long-term treatments for stroke. These happen in the days and months after emergency treatment deals with a stroke’s immediate threat.
Overall, your healthcare provider is the best person to tell you what kind of treatment(s) they recommend. They can tailor the information they provide to your specific case, including your medical history, personal circumstances and more.
Thrombolytic drugs
Thrombolytic drugs (their name is a combination of the Greek words “thrombus,” which means “clot,” and “lysis,” which means “loosening/dissolving”) are an option within the first three hours after stroke symptoms start. These medications dissolve existing clots. But they’re only an option within that three- to four-and-a-half hour time frame because after that, they increase the risk of dangerous bleeding complications.
Mechanical thrombectomy
In some cases, especially ones where thrombolytic drugs aren’t an option, a catheterization procedure known as mechanical thrombectomy is an option. Thrombectomy procedures are also time-sensitive, and the best window for these procedures is within 24 hours after symptoms start. This procedure involves inserting a catheter (tube-like) device into a major blood vessel and steering it up to the clot in your brain. Once there, the catheter has a tool at its tip that can remove the clot.
Blood pressure management
Because high blood pressure is usually why hemorrhagic strokes happen, lowering blood pressure is a key part of treating them. Lowering blood pressure limits bleeding and makes it easier for clotting to seal the damaged blood vessel.
Clotting support
Your body’s clotting ability relies on a process called hemostasis to stop bleeding and repair injuries. Supporting hemostasis involves infusion of medications or blood factors that make it easier for clotting to happen. Examples include vitamin K therapy, prothrombin or clotting factor infusions, and more. This treatment is most common with hemorrhagic strokes, and can help control bleeding (especially for people who take blood-thinning medications).
Surgery
In some cases, surgery is necessary to relieve the pressure on your brain. This is especially true with subarachnoid hemorrhages, which are easier to reach because they’re on the outer surface of your brain.
Supportive treatments and other methods
There are several other ways that stroke treatment can happen. Some of these treatments are supportive directly, while others help avoid complications. Your healthcare provider can tell you more about these other treatments and which ones they recommend and why.
Stroke rehabilitation
One of the most important ways to treat stroke is to help a person recover or adapt to the changes in their brain. That’s especially true when it comes to helping them regain abilities they had before the stroke. Stroke rehabilitation is a major part of recovery for most people who have a stroke. That rehabilitation can take many forms, including:
- Speech therapy: This can help you regain language and speaking abilities and improve your ability to control muscles that help you breathe, eat, drink and swallow.
- Physical therapy: This can help you improve or regain the ability to use your hands, arms, feet and legs. This can also help with balance issues, muscle weakness and more.
- Occupational therapy: This can help retrain your brain so you can go about your activities of daily life. This therapy is especially helpful with improving precise hand movements and muscle control.
- Cognitive therapy: This can be helpful if you’re having memory problems. It can also help if you have difficulty with activities that require focus or concentration that you could do before.
Other therapies are possible, depending on your case and circumstances. Your healthcare provider is the best person to tell you what kind of treatments can benefit you.
Complications
A stroke can sometimes cause temporary or permanent disabilities. Complications depend on how long the brain lacks blood flow and which part is affected. Complications may include:
- Loss of muscle movement, known as paralysis. You may become paralyzed on one side of the body. Or you may lose control of certain muscles, such as those on one side of the face or one arm.
- Trouble talking or swallowing. A stroke might affect the muscles in the mouth and throat. This can make it hard to talk clearly, swallow or eat. You also may have trouble with language, including speaking or understanding speech, reading or writing.
- Memory loss or trouble thinking. Many people who have had strokes experience some memory loss. Others may have trouble thinking, reasoning, making judgments and understanding concepts.
- Emotional symptoms. People who have had strokes may have more trouble controlling their emotions. Or they may develop depression.
- Pain. Pain, numbness or other feelings may occur in the parts of the body affected by stroke. If a stroke causes you to lose feeling in the left arm, you may develop a tingling sensation in that arm.
- Changes in behavior and self-care. People who have had strokes may become more withdrawn. They also may need help with grooming and daily chores.
Prevention
There are many things you can do to reduce your risk of having a stroke. While this doesn’t mean you can prevent a stroke, it can lower your risk. Actions you can take include:
- Improve your lifestyle. Eating a healthy diet and adding exercise to your daily routine can improve your health. You should also make sure to get enough sleep (the recommended amount is seven to eight hours).
- Avoid risky lifestyle choices or make changes to your behaviors. Smoking and tobacco use, including vaping, recreational drug use or prescription drug misuse, and alcohol misuse can all increase your risk of having a stroke. It’s important to stop these or never start them. If you struggle with any of these, talking to your healthcare provider is important. Your provider can offer you guidance and resources that can help you change your lifestyle to avoid these behaviors.
- Manage your health conditions and risk factors. There are several conditions, such as obesity, abnormal heart rhythms, sleep apnea, high blood pressure, Type 2 diabetes or high cholesterol, which can increase your risk of having an ischemic stroke. If you have one or more of these conditions, it’s very important that you do what you can to manage them, especially by taking medications — such as blood thinners — as prescribed by your provider. Doing that earlier in life can you avoid severe stroke-related problems later in life.
- See your primary care provider for a checkup or wellness visit annually. Yearly wellness visits can detect health problems — especially ones that contribute to having a stroke — long before you feel any symptoms.
Preventive medicines
If you have had an ischemic stroke, you may need medicines to help lower your risk of having another stroke. If you have had a TIA, medicines can lower your risk of having a stroke in the future. These medicines may include:
- Anti-platelet drugs. Platelets are cells in the blood that form clots. Anti-platelet medicines make these cells less sticky and less likely to clot. The most commonly used anti-platelet medicine is aspirin. Your healthcare professional can recommend the right dose of aspirin for you.If you’ve had a TIA or minor stroke, you may take both an aspirin and an anti-platelet medicine such as clopidogrel. These medicines may be prescribed for a period of time to reduce the risk of another stroke. If you can’t take aspirin, you may be prescribed clopidogrel alone. Ticagrelor is another anti-platelet medicine that can be used for stroke prevention.
- Blooding-thinning medicines, known as anticoagulants. These medicines reduce blood clotting. Heparin is a fast-acting anticoagulant that may be used short-term in the hospital. Slower acting warfarin may be used over a longer term. Warfarin is a powerful blood-thinning medicine, so you need to take it exactly as directed and watch for side effects. You also need regular blood tests to monitor warfarin’s effects. Several newer blood-thinning medicines are available to prevent strokes in people who have a high risk. These medicines include dabigatran, rivaroxaban, apixaban and edoxaban. They work faster than warfarin and usually don’t require regular blood tests or monitoring by your healthcare professional. These medicines also are associated with a lower risk of bleeding complications compared to warfarin.
Is there anything I shouldn’t eat or drink with this condition?
If you’re at risk for any kind of stroke, your healthcare provider may recommend changing your diet to avoid increases in blood pressure. Examples of this include:
- Beverages that contain caffeine, such as coffee, tea, soft drinks, etc.
- Foods that contain a lot of salt or sodium, which can increase blood pressure.
- Foods that are high in saturated fats, such as fried foods, etc.
- Alcohol or recreational stimulant drugs (cocaine, amphetamines/methamphetamine, etc.).
Living With
How do I take care of myself?
If you have a stroke, your healthcare provider will talk with you about a plan for treatment and the timeline for your recovery. They may also prescribe medications, recommend therapy options and more. It’s important to talk with your healthcare provider about why they recommend these and what they can do for you.
Once you and your provider finalize the treatment plan, it’s very important that you follow it as closely as possible. Doing that will give you the best chance to maximize how much you recover. Other things you can do include:
- Take your medication. Medications that you take after a stroke can prevent having another.
- Go to rehabilitation/therapy appointments. These appointments are critical to your recovery. Going to these appointments and putting in your best effort can make a big difference in how much you recover from a stroke.
- Take care of your mental health. Depression and anxiety are extremely common after having a stroke. Experiencing these doesn’t mean you’re weak or hopeless, but letting them go untreated can make it harder for you to recover. Talk to your healthcare provider about these feelings if you have them. They can recommend care that can help keep mental health concerns from standing in the way of your recovery.
- Make recommended lifestyle changes as best you can. Health concerns like your blood pressure, blood sugar and cholesterol can all play a role in your recovery from a stroke. Managing these can also help you avoid another stroke in the future. If you use tobacco products (including vaping products) of any kind, quitting them can also help greatly.
Conclusion from Dreducation.pk
In conclusion, a stroke is a serious medical condition that occurs when blood flow to the brain is disrupted, either by a blockage (ischemic stroke) or bleeding (hemorrhagic stroke). Recognizing early warning signs, like sudden vision changes, arm weakness, facial drooping, and speech difficulties, can be life-saving. Since strokes can cause lasting complications, prompt medical intervention is crucial to improve recovery outcomes. Lifestyle adjustments, managing existing health conditions, and taking preventive medications are key strategies in reducing stroke risk. With the right treatment and rehabilitation, many individuals can regain functionality and improve their quality of life post-stroke.