What is Pleural Effusion?
According to Wikipedia,
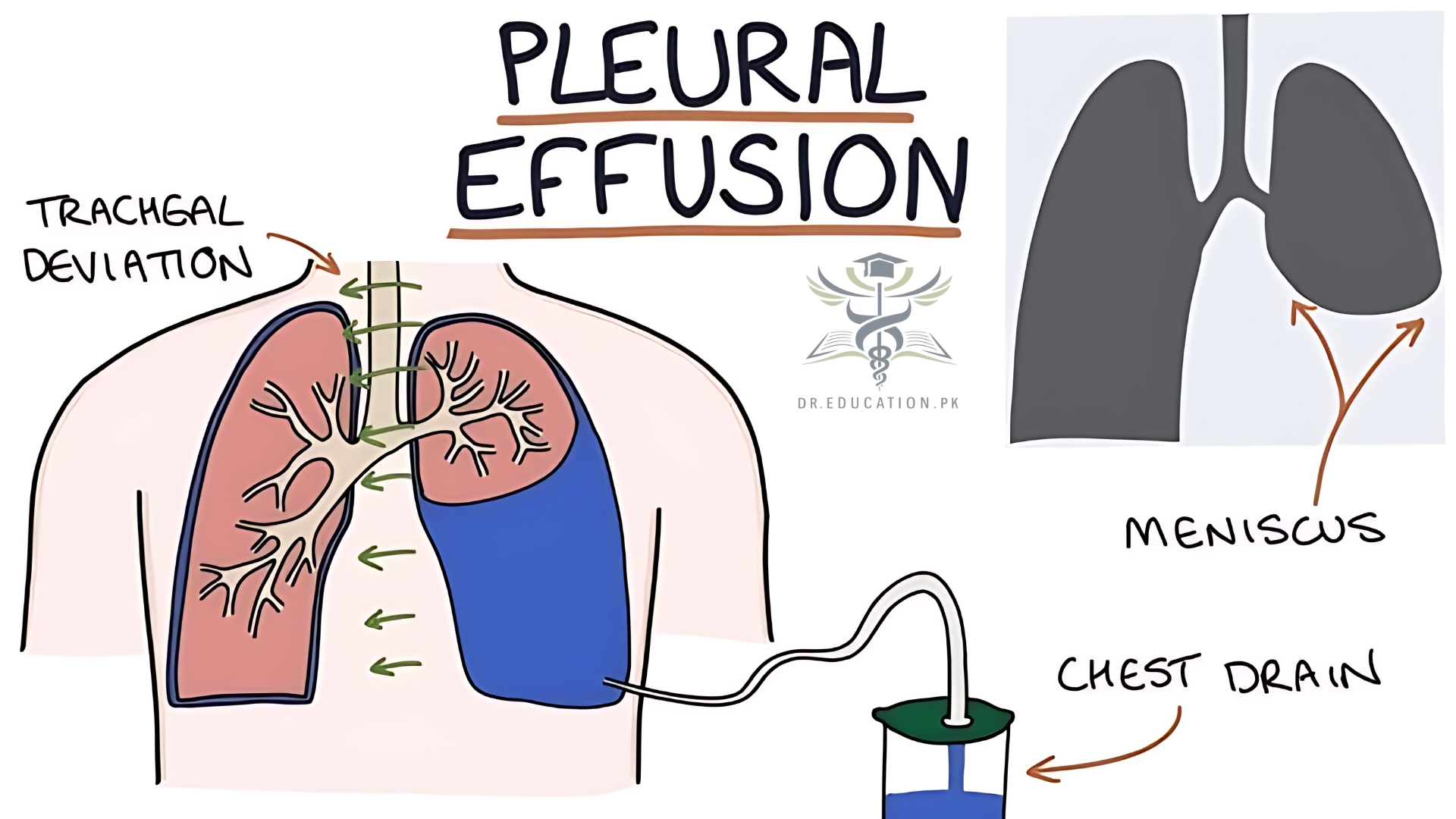
A pleural effusion is accumulation of excessive fluid in the pleural space, the potential space that surrounds each lung. Under normal conditions, pleural fluid is secreted by the parietal pleural capillaries at a rate of 0.6 millilitre per kilogram weight per hour, and is cleared by lymphatic absorption leaving behind only 5–15 millilitres of fluid, which helps to maintain a functional vacuum between the parietal and visceral pleurae. Excess fluid within the pleural space can impair inspiration by upsetting the functional vacuum and hydrostatically increasing the resistance against lung expansion, resulting in a fully or partially collapsed lung.
Overview
What is Pleural Effusion?
A pleural effusion is an unusual amount of fluid around the lung. Many medical conditions can lead to it, so even though your pleural effusion may have to be drained, your doctor likely will target the treatment at whatever caused it.
The pleura is a thin membrane that lines the surface of your lungs and the inside of your chest wall. When you have a pleural effusion, fluid builds up in the space between the layers of your pleura.
Normally, only teaspoons of watery fluid are in the pleural space, which allows your lungs to move smoothly in your chest cavity when you breathe.
Types of pleural effusion
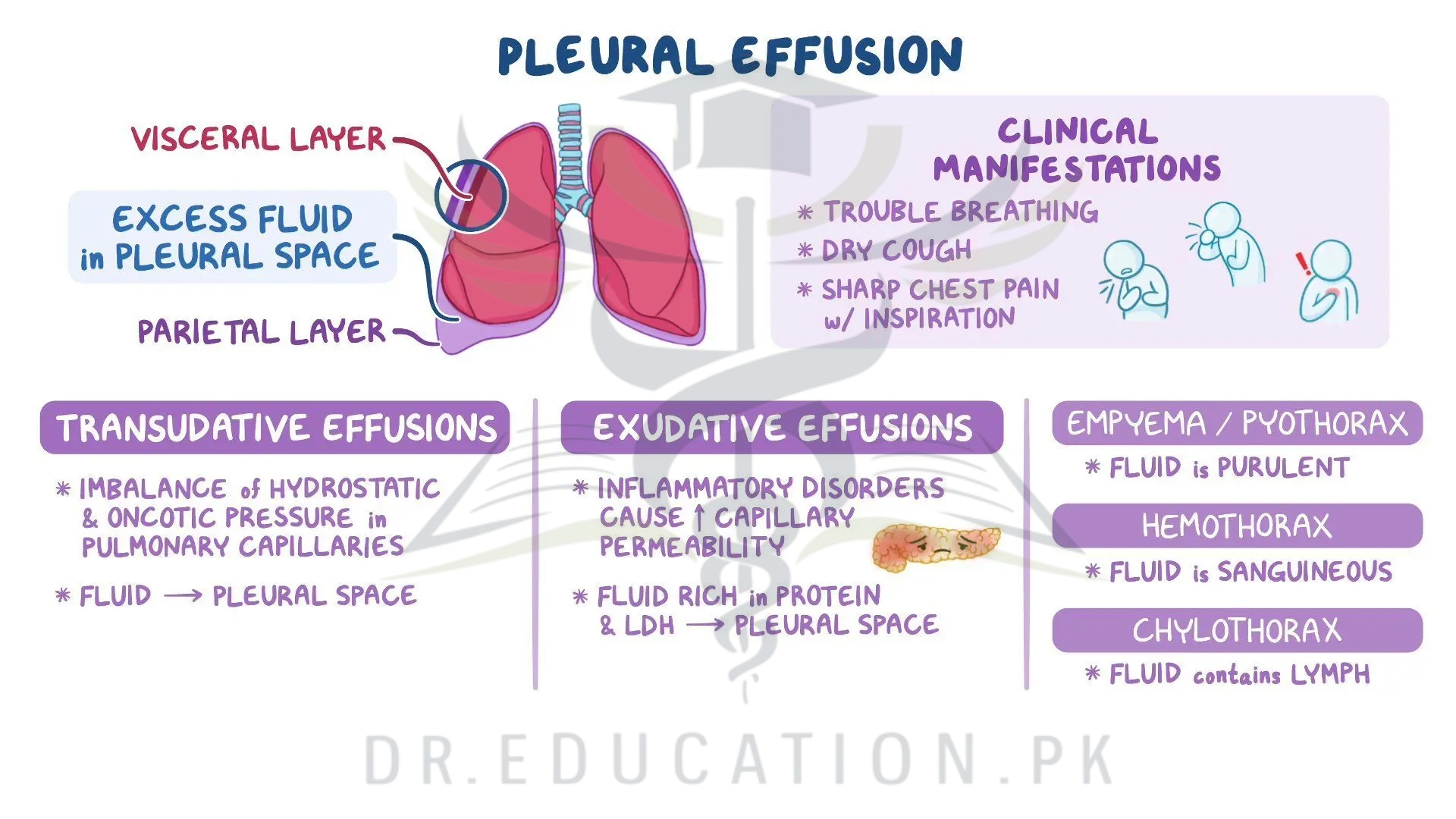
Healthcare providers split pleural effusion into two types, depending on the kind of fluid around your lungs.
Excess fluid may be:
- Protein-poor and watery (transudative). Fluid of this kind comes from cirrhosis or heart failure, for example. This type of pleural effusion happens when there’s an increase in pressure from the fluid.
- Protein-rich (exudative). Fluid of this kind comes from cancer or an infection, for example. This type of pleural effusion happens because too much fluid is getting through your smallest blood vessels or your lymphatic system isn’t draining enough.
Treatment varies by type and cause.
Causes
There are many causes of pleural effusion, and some people have more than one.
Depending on the cause, the excess fluid may be either protein-poor (transudative) or protein-rich (exudative). These two categories help providers determine the cause of the pleural effusion. A pulmonary embolism (PE) can fall under either category.
The most common causes of transudative (watery fluid) pleural effusions include:
- Heart failure.
- Cirrhosis.
- Nephrotic syndrome (a kidney issue).
Common causes of exudative (protein-rich fluid) pleural effusions include:
- Pneumonia.
- Cancer (lung cancer, breast cancer or lymphoma).
- Kidney disease.
- Inflammatory disease.
- Post open-heart surgery.
Less common causes of pleural effusion include:
- Tuberculosis.
- Autoimmune disease.
- Bleeding from chest trauma.
- Chylothorax (chyle from your lymphatic system after trauma).
- Rare chest and abdominal infections.
- Exposure to asbestos.
- Esophageal rupture.
- Pancreatitis.
- Meig’s syndrome (from a benign ovarian tumor).
- Ovarian hyperstimulation syndrome.
- Certain medications.
- Abdominal surgery.
- Radiation therapy.
In some cases, the fluid itself may have malignant (cancerous) cells or may be a direct result of chemotherapy.
Symptoms
Pleural effusion may often be asymptomatic. When present, symptoms include:
- Chest pain
- Coughing
- Shortness of breath
- Fever
- Difficulty in breathing
- Hiccups
As mentioned, a pleural effusion is usually caused by an underlying condition such as heart failure, pneumonia, cancer or liver disease, so symptoms of these diseases may also manifest themselves.
What are the risk factors for pleural effusion?
Risk factors for pleural effusion include:
- Medical conditions that cause it.
- Tobacco products.
- Exposure to asbestos.
What are the complications of pleural effusion?
Pleural effusion can lead to:
- An infection that becomes an abscess.
- Scarring around the lungs.
- Damage to your lungs.
Diagnosis and Test
If your doctor suspects a pleural effusion, he/she will elicit a medical history, as well as perform a physical examination. Tests for pleural effusion include:
- Chest X-ray – a detailed image of your heart and lungs is captured by an X-ray machine which the doctor examines to check for the presence of fluid.
- Blood tests may be conducted to check for infection or signs of underlying diseases such as lupus.
- ECG/EKG (Electrocardiogram) – this procedure is used to test your heartbeat to detect unusual patterns.
- Cardiac CT (Computerized Tomography) scan – this provides images of your heart and lungs to show if there are any signs of clotting or other causes of pleural effusion.
- Ultrasound – In this procedure, high frequency sound waves are used through a device known as a transducer. These waves create a moving image on a computer screen, which can then be checked for the presence of clots, excessive fluids or other abnormalities.
Additional procedures may sometimes be necessary. These include:
- Thoracentesis: Your doctor will inject a local anaesthetic between your ribs and then insert a needle through your chest wall to remove fluid and send for laboratory analysis.
- Pleural biopsy: This procedure is done to remove a sample of pleural tissue for examination under a microscope.
- Medical Pleuroscopy: This procedure is performed under local anaesthesia and sedation. During this procedure a sample of pleural tissue is obtained for further testing under direct visualization with a camera.
- Chest tube placement (tube thoracostomy): Sometimes a chest tube may need to be placed in the pleural effusion, e.g. with bad infections or recurrent pleural effusions.
- Surgery: This can be performed for diagnostic or therapeutic purposes.
Treatment
Your doctor may need to treat only the medical condition that caused the pleural effusion. You would get antibiotics for pneumonia, for instance, or diuretics for congestive heart failure.
Large, infected, or inflamed pleural effusions often need to get drained to help you feel better and prevent more problems.
Procedures for treating pleural effusions include:
Thoracentesis. If the effusion is large, your doctor may take more fluid than they need for testing, just to ease your symptoms.
Tube thoracostomy (chest tube). Your doctor makes a small cut in your chest wall and puts a plastic tube into your pleural space for several days.
Pleural drain. If your pleural effusions keep coming back, your doctor may put a long-term catheter through your skin into the pleural space. You can then drain the pleural effusion at home. Your doctor will tell you how and when to do that.
Pleurodesis. Your doctor injects an irritating substance (such as talc or doxycycline) through a chest tube into the pleural space. The substance inflames the pleura and chest wall, which then bind tightly to each other as they heal. Pleurodesis can prevent pleural effusions from coming back in many cases.
Pleural decortication. Surgeons can operate inside the pleural space, removing potentially dangerous inflammation and unhealthy tissue. To do this, your surgeon may make small cuts (thoracoscopy) or a large one (thoracotomy).
Complications/side effects of the treatment
Complications of treatment may include:
- Pulmonary edema.
- Blood clots.
- Abnormal heart rhythms.
- Pneumothorax (collapsed lung).
Prevention
You may not be able to avoid the many causes of pleural effusion. But you can lower your risk of pleural effusions in these ways:
- Avoiding tobacco products.
- Avoiding asbestos.
- Sticking to low-salt meals if your provider instructs you to.
- Taking prescribed diuretics (water pills).
- Limiting fluid intake if your provider tells you to.
When to see a Doctor?
If you suspect you have pleural effusion (fluid buildup between the layers of tissue lining the lungs and chest), it’s essential to see a doctor as soon as possible. Some signs that indicate you should seek medical help include:
- Shortness of Breath: Difficulty breathing or breathlessness, especially when lying down, is a common symptom and can worsen as fluid accumulates.
- Chest Pain: Persistent or sharp chest pain that worsens with deep breathing or coughing may indicate pleural effusion.
- Cough: An unexplained or persistent cough, especially if it’s not due to a respiratory infection, can be a sign of fluid buildup.
- Fever or Chills: If pleural effusion is due to an infection (e.g., pneumonia), you may experience fever, chills, or night sweats.
- Rapid Weight Loss: Weight loss without trying, especially if combined with other symptoms, could suggest an underlying cause like cancer.
- Other Respiratory Issues: If you have a history of heart disease, liver disease, kidney disease, or cancer, and you experience respiratory symptoms, it’s particularly important to see a doctor for evaluation.
Seeing a Doctor: A healthcare provider will typically order imaging tests like a chest X-ray, ultrasound, or CT scan to confirm the presence of fluid. They may also recommend a procedure called thoracentesis to remove and analyze the fluid, helping to determine the underlying cause.
If symptoms are severe or suddenly worsen, you should seek immediate medical care.
Conclusion from Dreducation.pk
In conclusion, pleural effusion is a condition involving excess fluid in the pleural space around the lungs, often caused by underlying health issues like heart failure, infection, or cancer. This fluid buildup can impair breathing and may lead to severe complications if untreated. Diagnosis involves imaging tests and sometimes fluid analysis, with treatments tailored to the underlying cause and may include procedures to drain excess fluid. Recognizing symptoms like shortness of breath, chest pain, and fever early and consulting a doctor promptly can help prevent complications and support recovery.