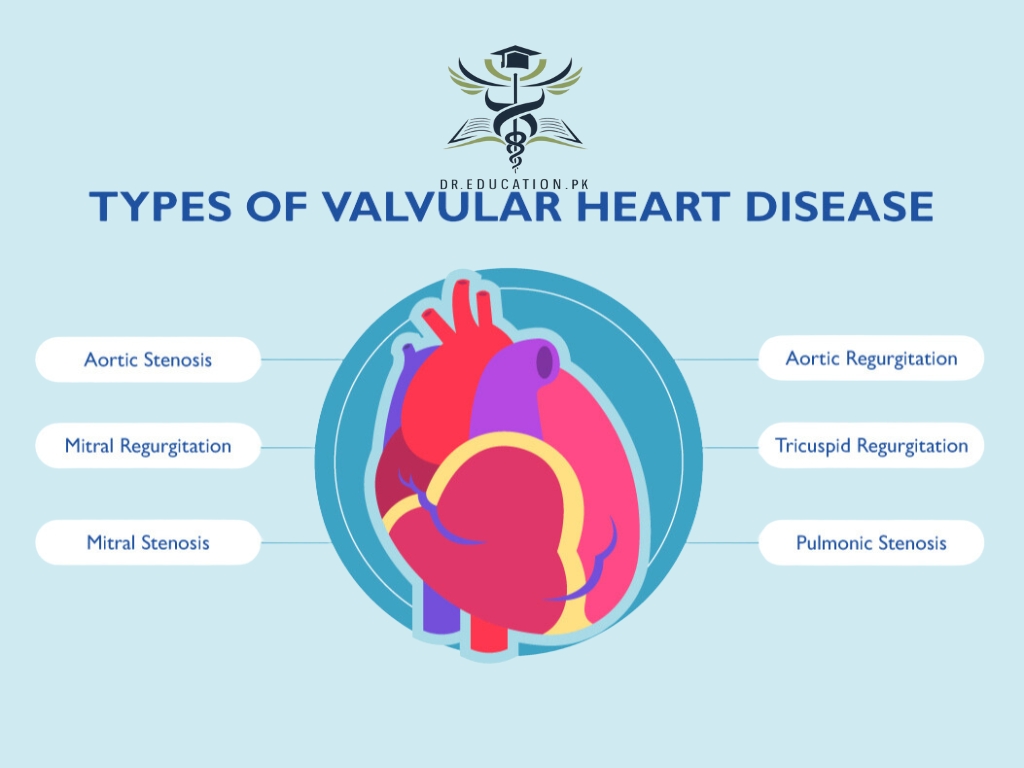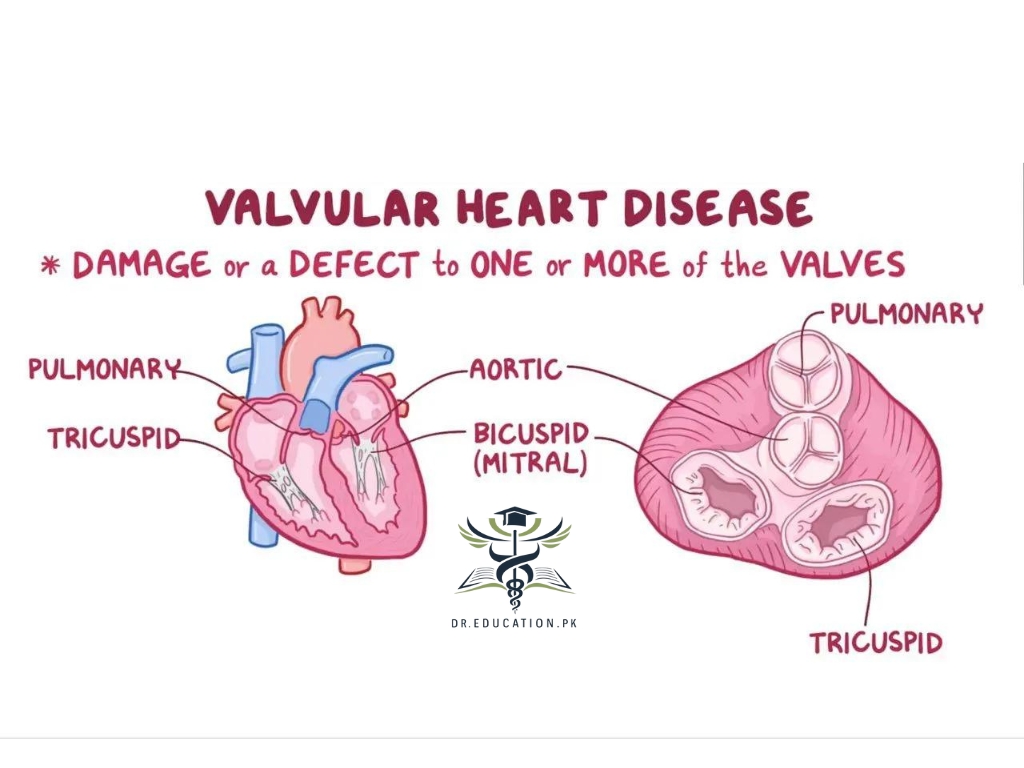
What is Valvular Heart Disease?
In heart valve disease, one or more of the valves in the heart doesn’t work properly. There are four heart valves. They keep blood flowing through the heart in the correct direction. Sometimes a valve doesn’t open or close all the way. This can change how blood flows through the heart to the rest of the body.
Heart valve disease treatment depends on the heart valve affected and the type and severity of the disease. Sometimes surgery is needed to repair or replace the heart valve.
Causes
To understand the causes of heart valve disease, it may be helpful to know how the heart works.
Four valves in the heart keep blood flowing in the right direction. These valves are:
- Aortic valve.
- Mitral valve.
- Pulmonary valve.
- Tricuspid valve.
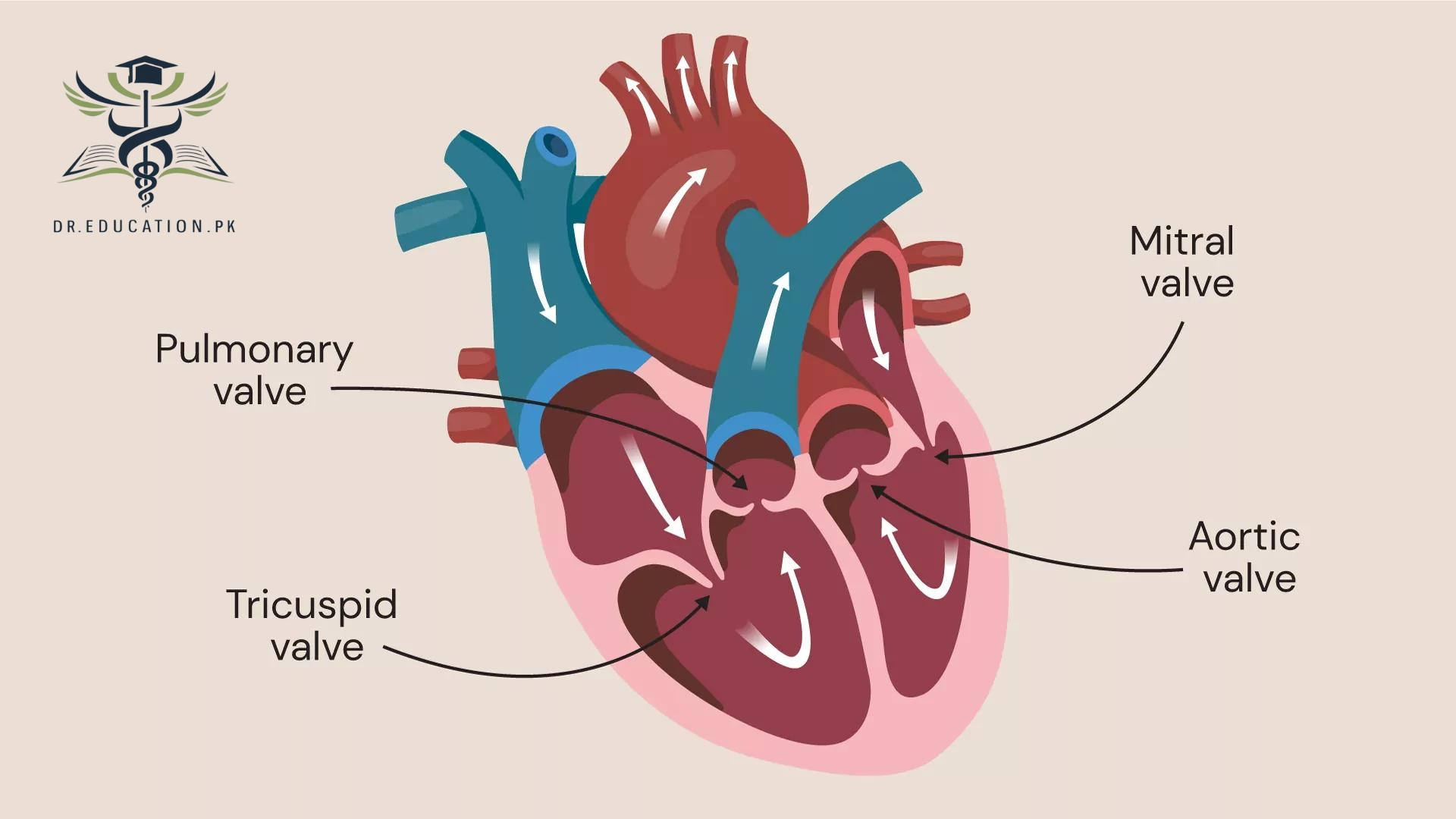
Each valve has flaps, called leaflets or cusps. The flaps open and close once during each heartbeat. If a valve flap doesn’t open or close properly, less blood moves out of the heart to the rest of the body.
Types of heart valve disease include:
- Stenosis. The valve flaps become thick or stiff and sometimes can join together. The valve opening becomes narrowed. Less blood can flow through the narrowed valve.
- Regurgitation. The valve flaps may not close tightly, causing blood to leak backward.
- Prolapse. The valve flaps become stretched out and floppy. They bulge backward like a parachute. This condition can lead to regurgitation.
- Atresia. The valve isn’t formed. A solid sheet of tissue blocks the blood flow between the heart chambers. This type usually affects the pulmonary valve.
Some people are born with heart valve disease. This is called congenital heart valve disease. But adults can get heart valve disease too. Causes of heart valve disease in adults may include infections, age-related changes and other heart conditions.
How common is heart valve disease?
About 2.5% of Americans — many of them older adults — have heart valve disease. Each year, roughly 28,000 people die from heart valve disease in the United States. Mitral valve prolapse is a common heart valve problem.
How does heart valve disease affect my body?
When a heart valve isn’t working right, it puts a strain on your heart because it makes it work harder. Also, it can cause less blood flow to your body.
Symptoms
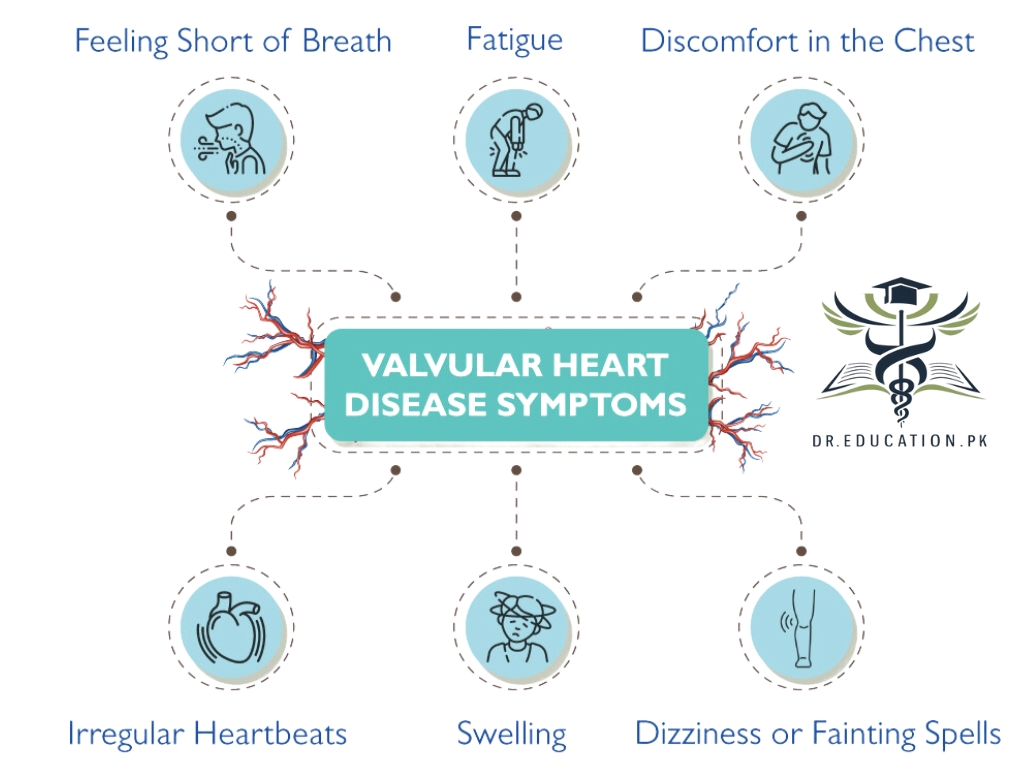
Some people with heart valve disease might not have symptoms for many years. When symptoms occur, they might include:
- Shortness of breath at rest or when active or lying down.
- Fatigue.
- Chest pain.
- Dizziness.
- Swelling of the ankles and feet.
- Fainting.
- Irregular heartbeat.
What causes heart valve disease?
Common heart valve disease causes include:
- Rheumatic fever from strep throat that wasn’t treated.
- Heart attack that damages your heart.
- High blood pressure (advanced).
- A congenital problem that’s been present since birth, such as a pulmonary or aortic valve that didn’t develop right.
- Degeneration or calcification of the valve tissue, with loss of function over time.
- Thoracic aortic aneurysm(dilation of the aorta, which stretches the aortic valve leaflets and can cause leakage).
- Heart failure.
- Infection in your heart (infective endocarditis).
Risk factors
Several things can increase the risk of heart valve disease, including:
- Older age.
- Some infections, such as rheumatic fever or blood infections.
- A heart attack or some types of heart disease.
- High blood pressure, high cholesterol, diabetes and other heart disease risk factors.
Complications
Heart valve disease can cause many complications, including:
- Heart failure
- Stroke
- Blood clots
- Heart rhythm abnormalities
- Death
Diagnosis
To diagnose heart valve disease, a health care professional examines you and asks questions about your symptoms and health history. A whooshing sound called a heart murmur may be heard when listening to your heart with a device called a stethoscope.
Blood and imaging tests may be done to check your heart health.
Tests
Tests to diagnose heart valve disease may include:
- Echocardiogram. This test uses sound waves to create pictures of the beating heart. It shows how blood flows through the heart and the health of the heart valves. There are different types of echocardiograms. The type you have depends on the reason for the test and your overall health.
- Electrocardiogram (ECG or EKG). This quick test records the electrical signals in the heart. It shows how the heart is beating. Sensors, called electrodes, are attached to the chest and sometimes the legs. Wires connect the sensors to a computer, which displays or prints results.
- Chest X-ray. A chest X-ray shows the heart and lungs. The test can tell if the heart is larger than usual or if there is fluid around the lungs. Fluid could be due to some types of heart valve disease.
- Cardiac MRI. A cardiac MRI uses magnetic fields and radio waves to create detailed images of the heart. It can help determine the severity of heart valve disease.
- Exercise tests or stress tests. These tests often involve walking on a treadmill or riding a stationary bike while the heart is checked. Exercise tests show how the heart responds to physical activity and whether valve disease symptoms occur during exercise. If you can’t exercise, you might get medicines that mimic the effect of exercise on the heart.
- Cardiac catheterization. This test isn’t often used to diagnose heart valve disease. But it may be done if other tests can’t diagnose a heart valve problem. Or it might be used to tell how severe heart valve disease is. A long, thin flexible tube called a catheter is inserted in a blood vessel, usually in the groin or wrist. It’s guided to the heart. Dye flows through the catheter into the arteries in the heart. The dye helps the arteries show up more clearly on X-ray images and video.
Heart valve disease stages
After testing confirms a diagnosis of heart valve disease, your health care team may tell you the stage of disease. Staging helps determine the most appropriate treatment.
The stage of heart valve disease depends on many things, including symptoms, disease severity, the structure of the valve or valves, and blood flow through the heart and lungs.
Heart valve disease is staged into four basic groups:
- Stage A: At risk. Risk factors for heart valve disease are present.
- Stage B: Progressive. Valve disease is mild or moderate. There are no heart valve symptoms.
- Stage C: Asymptomatic severe. There are no heart valve symptoms but the valve disease is severe.
- Stage D: Symptomatic severe. Heart valve disease is severe and is causing symptoms.
Management and Treatment
How is heart valve disease treated?
A heart valve problem can be serious if it’s not treated. Although you can’t undo damage to a heart valve, you can treat the issue.
Heart valve disease treatments depend on the underlying cause and may include:
- Protecting your valve from further damage.
- Taking medications.
- Having surgery or invasive procedures if necessary.
- Seeing your heart doctor for regular visits.
The decision to prescribe medical treatment, surgical repair or surgical replacement depends on several factors, including:
- The type of valve disease.
- The severity of the damage.
- Your age.
- Your medical history.
If you’re pregnant and have heart valve disease, you can get extra rest and/or take certain medicines that are safe for your baby.
If you know about your valve disease before pregnancy, you should ask your healthcare provider if any tests or visits with a cardiologist are recommended before trying to become pregnant. This can help ensure that you are treated appropriately before and during pregnancy. If you have a severe valve problem, your doctor may recommend valve repair or replacement before pregnancy.
Surgical repair or replacement
Heart valve disease is a mechanical problem in the opening or closing of the leaflets, and you may eventually need surgery to repair or replace your valve. Some infants and children who are born with a valve problem need surgery during childhood.
Usually, the surgeon and cardiologist will know which treatment will be best before surgery day. Other times, the surgeon makes the decision during surgery, when they can see your valve.
Often, valve surgery may be combined with other procedures (such as more than one valve procedure, bypass surgery or surgery to treat atrial fibrillation) to fully treat your heart disease.
Heart valve repair allows your surgeon to fix your faulty valve, often without the use of artificial parts. In some cases, such as a narrow mitral valve, your provider may use a balloon on a catheter to widen your valve.
The advantages of valve repair are:
- Lower risk of infection.
- Decreased need for lifelong blood thinner medication.
- Preserved heart muscle strength and function.
Surgeons have to replace valves they can’t repair. Replacing your heart valve involves removing your old valve and sewing a new valve to the ring-shaped part of your old valve. The new valve could be a mechanical or biological (made with tissue from a human, cow or pig) valve. These replacement valves can provide adequate function when repair can’t. However, depending on the type of valve your provider uses, you may have to take certain medications to prevent blood clots or get a new valve again in 10 or 15 years.
Depending on the type of valve problem and your other medical conditions, you may be a candidate for minimally invasive valve repair or replacement. Ask your cardiologist if a minimally invasive procedure may be right for you.
What medications are used?
Although medicines can’t cure heart valve disease, they — and a healthier lifestyle — can help with symptoms and decrease your chance of having a stroke or sudden cardiac arrest. You may be able to stop taking some medications after valve surgery, but you may need to take other medicines for the rest of your life.
Your healthcare provider may prescribe medications to help you with:
- Preventing arrhythmias or blood clots.
- Bringing down your blood pressure or cholesterol levels.
- Treating heart failure or coronary artery disease.
Your provider will review your medication information with you before you leave the hospital. It’s important to know:
- The names of your medications.
- Their purpose.
- How often and at what times to take them.
Complications/side effects of the treatment
Older people and those whose health is not good to begin with have a higher risk of complications from valve replacement surgery.
Complications, which are rarely fatal, may include:
- Infection.
- Atrial fibrillation or another type of abnormal heart rhythm.
- Bleeding.
- Blood clots.
- Kidney failure.
- Stroke or transient ischemic attack (TIA).
Prevention
How can I reduce my risk of heart valve disease?
Although you can’t change some risk factors, like growing older, there are things you can do that may reduce your risk of heart valve disease. These include:
- Getting treatment quickly for infections.
- Being physically active.
- Eating healthy foods.
- Staying at a healthy weight.
- Continuing to take medicine for high blood pressure and/or high cholesterol if you have those conditions.
- Not using tobacco products.
- Not using recreational drugs, especially IV drugs which increase your risk for heart valve infection.
Lifestyle and home remedies
If you have heart valve disease, your health care team may suggest making lifestyle changes. Try these steps:
- Eat a heart-healthy diet. Eat a variety of fruits and vegetables, low-fat or fat-free dairy products, poultry, fish, and whole grains. Avoid saturated and trans fats and excess salt and sugar.
- Get regular exercise. As a general goal, aim for at least 30 minutes of moderate physical activity every day. Talk to your health care team before starting a new exercise routine.
- Maintain a healthy weight. Being overweight raises the risk of heart problems. Talk with your care team to set realistic goals for weight.
- Don’t use tobacco. If you smoke or chew tobacco, quit. Smoking is a major risk factor for heart disease. Quitting is the best way to reduce the risk. If you need help quitting, talk to a health care professional.
- Practice good sleep habits. Poor sleep may increase the risk of heart disease. Adults should aim to get 7 to 9 hours of sleep daily. Go to bed and wake at the same time every day, including on weekends. If you have trouble sleeping, talk to your health care team about strategies that might help.
- Control blood pressure. Uncontrolled high blood pressure increases the risk of serious health problems. Get your blood pressure checked at least every two years if you’re 18 and older. If you have risk factors for heart disease or are over age 40, you may need more-frequent checks.
- Get a cholesterol test. Get a baseline cholesterol test when you’re in your 20s and then at least every 4 to 6 years. Some people may need to start testing earlier or have more-frequent checks.
- Manage diabetes. If you have diabetes, tight blood sugar control can help keep your heart healthy.
Pregnancy
Careful and regular checkups are needed for those who have heart valve disease during pregnancy. If you have a severe heart valve condition, you might be told not to get pregnant to reduce the risk of complications.