What is COVID-19?
According to WHO,
Coronavirus disease (COVID-19) is an infectious disease caused by the SARS-CoV-2 virus.
Most people infected with the virus will experience mild to moderate respiratory illness and recover without requiring special treatment. However, some will become seriously ill and require medical attention. Older people and those with underlying medical conditions like cardiovascular disease, diabetes, chronic respiratory disease, or cancer are more likely to develop serious illness. Anyone can get sick with COVID-19 and become seriously ill or die at any age.

Overview
What is coronavirus?
COVID-19, also known as Coronavirus Disease 2019, is a viral illness caused by the novel coronavirus SARS-CoV-2. The virus emerged in late 2019 in the city of Wuhan, Hubei province, China, and rapidly spread globally, leading to a pandemic. The World Health Organization (WHO) officially declared the outbreak a Public Health Emergency of International Concern (PHEIC) on January 30, 2020, and it was characterized as a pandemic on March 11, 2020. COVID-19 has since caused widespread illness, significant morbidity and mortality, and has profoundly impacted global economies, healthcare systems, and daily life.
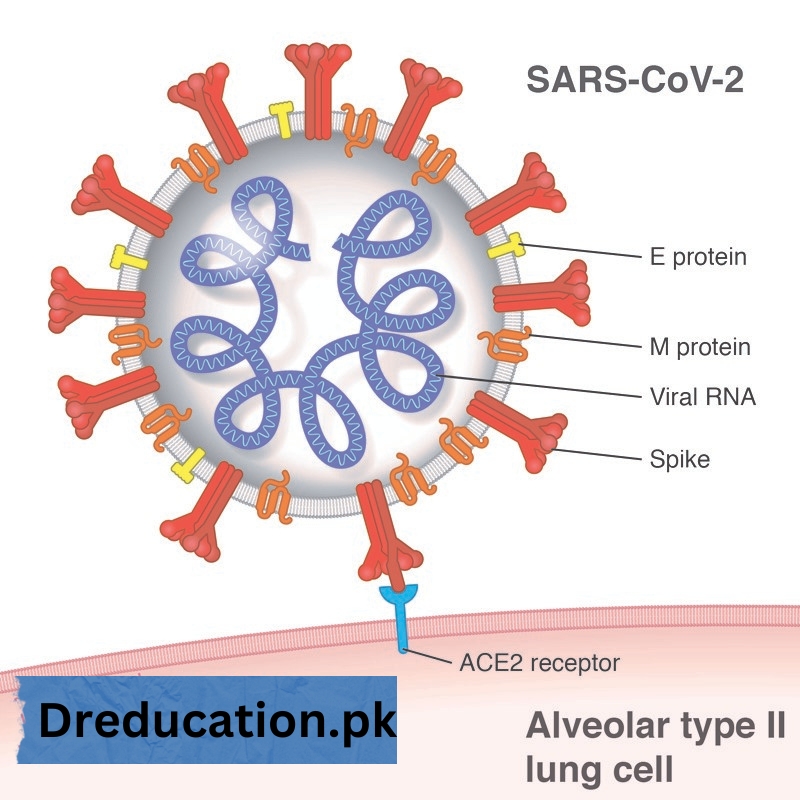
The Virus: SARS-CoV-2
SARS-CoV-2 is a novel strain of coronavirus, a family of viruses known to cause respiratory infections in humans and animals. Coronaviruses are named for the crown-like spikes on their surface (corona is Latin for crown). Other notable coronaviruses that caused severe human diseases in the past include SARS-CoV (which caused Severe Acute Respiratory Syndrome or SARS in 2003) and MERS-CoV (which caused Middle East Respiratory Syndrome or MERS in 2012).
SARS-CoV-2 is a positive-sense single-stranded RNA virus. It primarily targets the human respiratory system, binding to the ACE2 (angiotensin-converting enzyme 2) receptor on the surface of cells in the lungs and other organs. Once inside a host cell, the virus replicates and spreads to neighboring cells, causing inflammation and damage to tissues, especially the lungs.
How does the new coronavirus (SARS-CoV-2) spread from person to person?
COVID-19 spreads through multiple modes, primarily:
- Respiratory Droplets: The virus spreads from person to person mainly through respiratory droplets when an infected individual coughs, sneezes, talks, or breathes. These droplets can land in the mouths or noses of nearby people or be inhaled into the lungs.
- Airborne Transmission: In certain conditions, such as poorly ventilated indoor environments, smaller particles known as aerosols can remain suspended in the air for longer periods and can be inhaled by individuals over a distance.
- Surface Transmission (Fomite Transmission): Although less common, the virus can be transmitted by touching surfaces or objects that have been contaminated with the virus and then touching the face, particularly the mouth, nose, or eyes.
- Close Contact: Physical proximity to an infected individual increases the risk of transmission, particularly in settings like households, public gatherings, and healthcare facilities.
The virus can be spread by individuals who are symptomatic, pre-symptomatic, or asymptomatic, making it more difficult to control its spread.
How long is a person with COVID-19 considered contagious?
If you have COVID-19 it can take several days to develop symptoms — but you’re contagious during this time. You are no longer contagious 10 days after your symptoms began.
The best way to avoid spreading COVID-19 to others is to:
- Stay 6 feet away from others whenever possible.
- Wear a cloth mask that covers your mouth and nose when around others.
- Wash your hands often. If soap isn’t available, use a hand sanitizer that contains at least 60% alcohol.
- Avoid crowded indoor spaces. Open windows to bring in outdoor air as much as possible.
- Stay self-isolated at home if you are feeling ill with symptoms that could be COVID-19 or have a positive test for COVID-19.
- Clean and disinfect frequently touched surfaces.
Who’s most at risk for getting COVID-19?
Persons at greatest risk of contracting COVID-19 include those who:
- Live in or have recently traveled to any area with ongoing active spread.
- Have had close contact with a person who has a laboratory-confirmed or a suspected case of the COVID-19 virus. Close contact is defined as being within 6 feet of an infected person for a cumulative total of 15 minutes or more over a 24-hour period.
- Are over the age of 60 with pre-existing medical conditions or a weakened immune system.
How soon after becoming infected with SARS-CoV-2 will I develop COVID-19 symptoms?
The time between becoming infected and showing symptoms (incubation period) can range from two to 14 days. The average time before experiencing symptoms is five days. Symptoms can range in severity from very mild to severe. In about 80% of people, COVID-19 causes only mild symptoms, although this may change as variants emerge.
If I recover from a case of COVID-19, can I be infected again?
If you test positive for SARS-CoV-2 three months after your last positive test, it’s considered a reinfection. Before the omicron variant, reinfection with SARS-CoV-2 was rare but possible.
Omicron (B.1.1.529) was first reported in South Africa in November 2021 and quickly spread around the world. With many mutations, omicron was able to evade immune systems and we had more reinfections than ever before.
As the virus that causes COVID-19 continues to mutate, reinfection remains possible. Vaccination — including a booster dose — is the best protection against severe disease.
Symptoms
COVID-19 presents a wide range of symptoms, which can appear 2–14 days after exposure to the virus. The severity of symptoms varies greatly, ranging from mild to severe, and in some cases, individuals may be entirely asymptomatic but still able to transmit the virus.
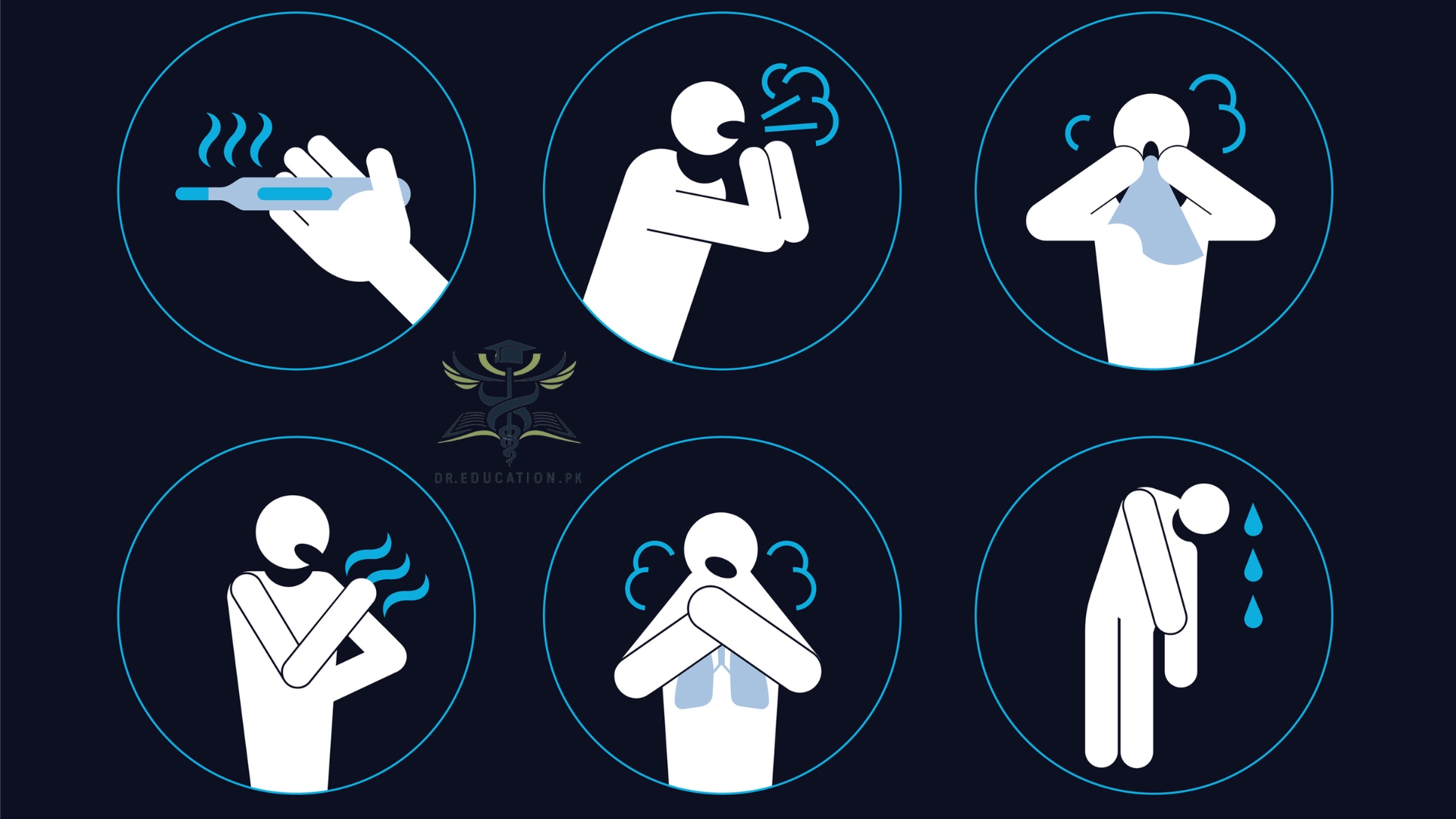
Common symptoms include:
- Fever
- Cough
- Fatigue
- Loss of taste or smell
- Sore throat
- Shortness of breath or difficulty breathing
- Headache
- Muscle or body aches
- Chills
In more severe cases, COVID-19 can lead to:
- Pneumonia
- Acute Respiratory Distress Syndrome (ARDS)
- Sepsis
- Multi-organ failure
Individuals with pre-existing conditions such as cardiovascular disease, diabetes, chronic respiratory diseases, obesity, or weakened immune systems are at higher risk for severe illness and complications from COVID-19. Older adults are also more vulnerable to the severe impacts of the disease.
Long COVID
In addition to acute illness, some individuals experience prolonged symptoms and complications, a condition referred to as “Long COVID” or “Post-Acute Sequelae of SARS-CoV-2 infection” (PASC). Long COVID can affect both mild and severe cases and includes a variety of symptoms such as:
- Fatigue
- Brain fog
- Shortness of breath
- Joint pain
- Heart palpitations
Long COVID may persist for weeks or even months after the acute phase of the infection has passed, significantly affecting the quality of life for those impacted.
Diagnosis and Tests
How is coronavirus diagnosed?
COVID-19 is diagnosed with a laboratory test. Your healthcare provider may collect a sample of your saliva or swab your nose or throat to send for testing.
When should I be tested for the coronavirus (COVID-19)?
Call your healthcare provider if you:
- Feel sick with fever, cough or have difficulty breathing.
- Have been in close contact with a person known or suspected to have COVID-19.
Your healthcare provider will ask you questions about your symptoms and tell you if you need to be tested for COVID-19.
If I have a positive test for coronavirus, how long should I self-isolate?
According to current CDC recommendations, you should self-isolate until you’ve met both of the following criteria:
- It’s been five days since your symptoms first appeared and your symptoms are improving.
- You’ve not had a fever for 24 hours and you’ve not used fever-lowing medications during this time.
While at home, self-isolate within a separate room of your home if possible to limit interaction with other family members. If you can’t stay 100% isolated in a separate room, keep 6 feet away from others and wear a cloth mask, wash your/family members’ hands often and frequently disinfect commonly touched surfaces and shared areas.
You don’t need to be retested after your period of self-isolation. But every case is unique, so follow your healthcare provider’s recommendations for testing.
If you have a weakened immune system or have had a severe case of COVID-19, the CDC’s criteria don’t apply to you. You may need to stay home for up to 20 days after your symptoms first appeared. Talk with your healthcare provider about your situation.
How long do I need to isolate myself if I’ve been around a person with COVID-19?
You should quarantine for five days if:
- You haven’t been fully vaccinated.
- More than six months have gone by since your second vaccine dose and you haven’t been boosted.
After this time, you should wear a well-fitting mask whenever you’re around others for an additional five days. The CDC recommends testing on day five if possible. This quarantine period may vary depending on variant strains and the availability of testing.
Is it possible to test negative for coronavirus and still be infected with it?
Yes, it’s possible. There are several reasons for “false negative” test results — meaning you really do have COVID-19 although the test result says you don’t.
Reasons for a false negative COVID-19 test result include:
- You were tested too early in the course of illness. The virus hasn’t multiplied in your body to the level that it could be detected by the test.
- The swab didn’t get a good specimen. You or the healthcare personnel may not have swabbed deeply enough in your nasal cavity to collect a good sample. There could also be less likely handling errors and transportation errors.
- The test itself was not sensitive or specific enough to detect SARS-CoV-2, the virus that causes COVID-19. Sensitivity refers to the ability of the test to detect the smallest amount of virus. Specificity refers to the ability of the test to detect only the COVID-19 virus and not other similar viruses. Many different commercial and hospital laboratories have developed tests for SARS-CoV-2. All must meet standards, but there’s always the possibility of “false negative” and “false positive” tests.
If you think you might have COVID-19 even if your test is negative, it’s best to follow the current CDC recommendations. Stay home for 10 days if you think you are sick (“social distancing”). Stay 6 feet away from others (“physical distancing”) and wear a cloth mask. Contact your healthcare provider if your symptoms worsen. Don’t decide on your own if it’s safe for you to be around others. Instead, contact your healthcare provider when your symptoms improve.
Prevention
Several preventive measures can reduce the risk of contracting or spreading COVID-19:
- Vaccination: COVID-19 vaccines, developed in record time, have been a critical tool in controlling the pandemic. Vaccines from various manufacturers, including Pfizer-BioNTech, Moderna, AstraZeneca, and Johnson & Johnson, have been widely distributed. These vaccines significantly reduce the severity of the disease and lower hospitalization and death rates.
- Mask-Wearing: Wearing face masks, particularly in indoor or crowded settings, reduces the spread of respiratory droplets and aerosols.
- Social Distancing: Maintaining physical distance from others, especially in crowded or enclosed spaces, helps reduce transmission.
- Hand Hygiene: Frequent handwashing with soap and water or using alcohol-based hand sanitizers can prevent infection through contaminated surfaces.
- Ventilation: Ensuring good airflow in indoor spaces reduces the concentration of airborne viral particles.
- Isolation and Quarantine: Infected individuals are advised to isolate to prevent spreading the virus, while those exposed to COVID-19 should quarantine until they are confirmed negative.
Vaccination
Vaccines have been a major breakthrough in the fight against COVID-19. By the end of 2021, multiple vaccines had been authorized for emergency use around the world. These vaccines work by training the immune system to recognize and fight the virus without causing the disease.
- mRNA Vaccines: Pfizer-BioNTech and Moderna are examples of mRNA vaccines, which use a small piece of the virus’s mRNA to instruct cells to produce a protein found on the virus’s surface, triggering an immune response.
- Viral Vector Vaccines: AstraZeneca and Johnson & Johnson vaccines use a harmless virus (not the coronavirus) to deliver a gene that instructs cells to produce the spike protein found on SARS-CoV-2, eliciting an immune response.
- Protein Subunit Vaccines: These vaccines use harmless pieces of the virus (often proteins) to stimulate an immune response.
Treatment
Treatment for COVID-19 depends on the severity of the disease:
- Mild Cases: Most people with mild illness recover at home with rest, fluids, and over-the-counter medications to manage symptoms.
- Moderate to Severe Cases: Hospitalization may be required for individuals with difficulty breathing, low oxygen levels, or worsening symptoms. Treatments for severe cases include:
- Oxygen Therapy: Administered to patients with low oxygen levels.
- Antiviral Drugs: Remdesivir is an antiviral medication used to reduce viral replication in the body.
- Corticosteroids: Dexamethasone has been used to reduce inflammation in severe cases.
- Monoclonal Antibodies: These are lab-produced molecules that can mimic the immune system’s ability to fight off harmful pathogens like viruses.
- Mechanical Ventilation: In critical cases, patients may require ventilators to help them breathe.
There is no definitive cure for COVID-19, but ongoing clinical trials continue to explore potential therapies and treatments.
Global Impact
The COVID-19 pandemic has had a far-reaching impact on health, economies, and societies. Healthcare systems were overwhelmed by the surge in cases, especially in early 2020. Lockdowns and restrictions implemented to curb the spread of the virus caused significant economic disruptions, leading to job losses, business closures, and a global recession.
Education systems were also affected, with schools and universities around the world transitioning to remote learning. Mental health challenges increased due to isolation, uncertainty, and the stresses of the pandemic. The pandemic also highlighted inequalities in healthcare access and socioeconomic factors, disproportionately affecting marginalized and vulnerable populations.
Should I wear a face mask?
Your healthcare provider can answer any questions you have about when you should wear a face mask to help slow the transmission of COVID-19. In general, the CDC recommends wearing a face mask in the following situations:
- If you’re in an area with high community levels of COVID-19, wear a face mask in public.
- If you’re sick but can’t avoid being around others.
- If you’re caring for someone who has COVID-19.
- If you’re at higher risk for severe illness or live with someone who is.
When to see a Doctor.